Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Steven Lamb, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand. 2001. Updated by Hon A/Prof Amanda Oakley, September 2016. Minor update June 2023.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outcome
Benign familial pemphigus is also known as Hailey–Hailey disease. It is a rare hereditary blistering skin disease first described by the Hailey brothers in 1939.
Unrelated to pemphigus vulgaris, Hailey-Hailey disease is not an autoimmune condition and has a differing prognosis.
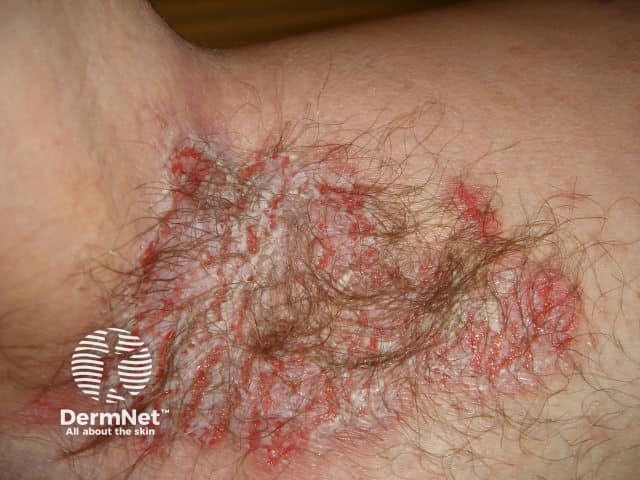
Hailey-Hailey disease in axilla
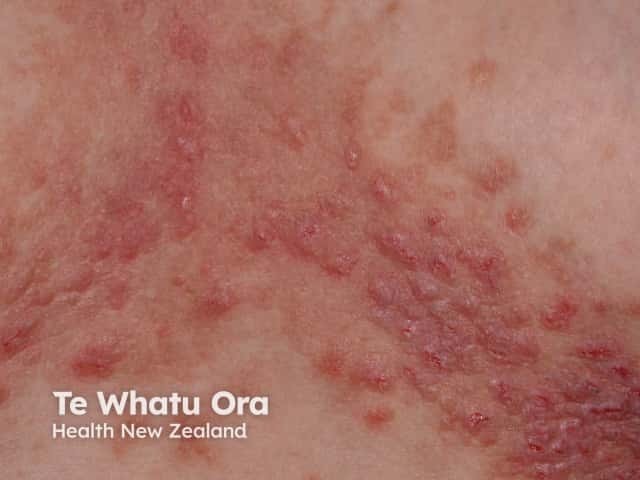
Hailey-Hailey disease of chest
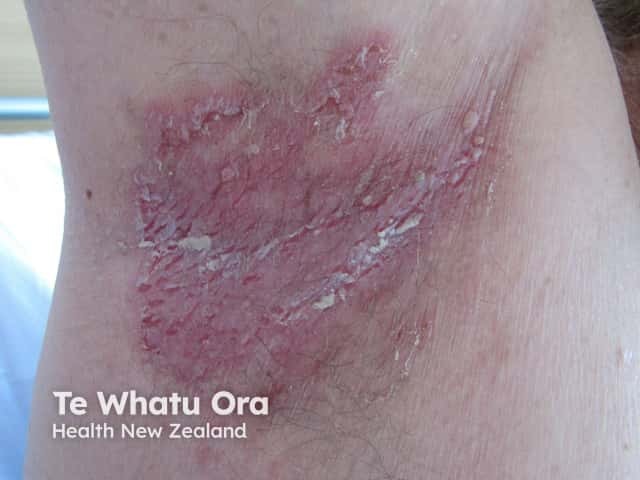
Hailey-Hailey disease in axilla
Benign familial pemphigus usually appears in the second to fourth decade, although it can occur at any age. It then tends to persist life-long. It can affect people of all races.
Benign familial pemphigus is an inherited skin disorder, although occasionally sporadic cases arise without a family history. The defect responsible has now been identified on a gene called ATP2C1 found on chromosome 3q21-24. This gene codes for the protein SPCA1 (Secretory Pathway Calcium/manganese-ATPase), a calcium and manganese pump. The skin cells (keratinocytes) stick together via structures called desmosomes and it seems the desmosomes do not assemble properly if there is insufficient calcium.
The genetic defect in benign familial pemphigus causes the skin cells to become unstuck from one another. Normally the cells are packed together tightly in much the same way as bricks and mortar. Patients with Hailey-Hailey disease have defective ´mortar´ and the cells fall apart, like a dilapidated brick wall.
Benign familial pemphigus typically begins as a symmetrical painful erosive and crusted skin rash in the skin folds. Common sites include the armpits, groins, and neck, under the breasts and between the buttocks. The lesions tend to come and go and leave no scars. As the lesions get bigger the centre clears leaving a typical ring shape. If the lesions are present for some time they may become thickened. The skin then tends to macerate leaving quite painful cracks.
Heat, sweating and friction often exacerbate the disease, and most patients have worse symptoms during the summer months.
Rarely, benign familial pemphigus can be unilateral or have a linear arrangement, or it may involve mucous membranes. White bands on the fingernails and pits in the palms can also occur.
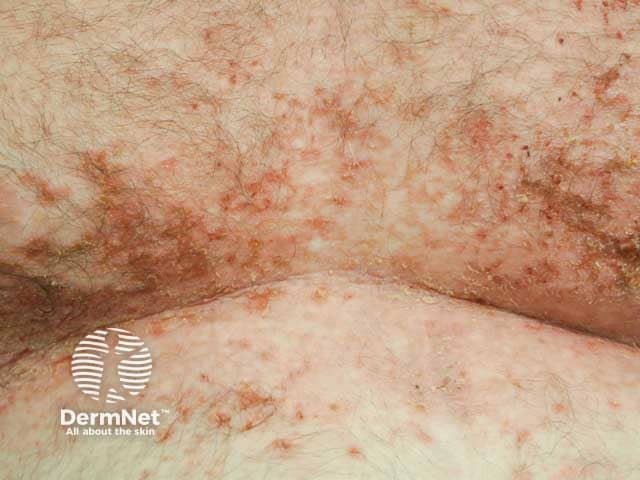
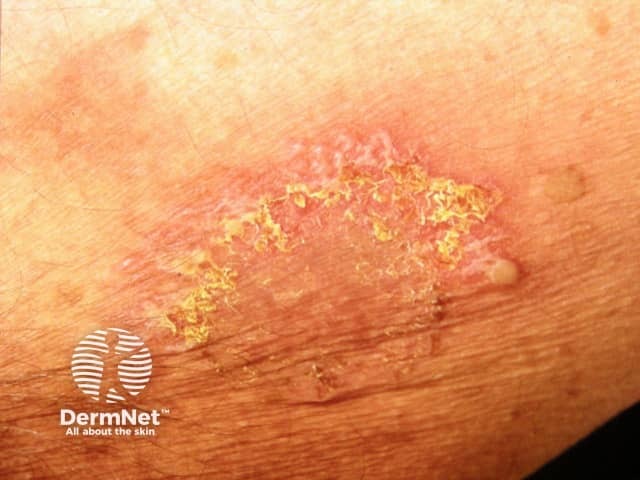
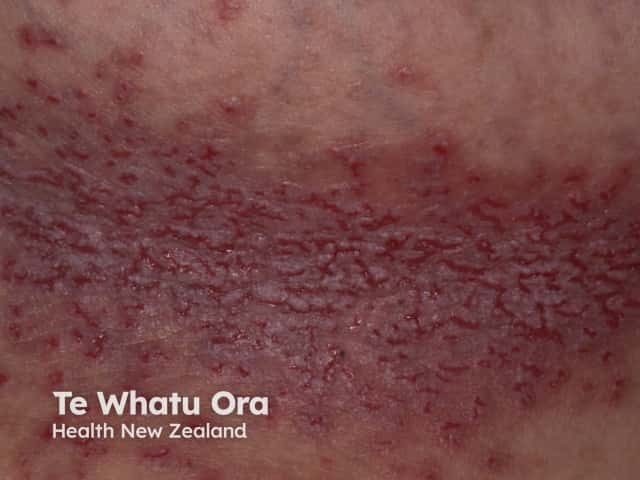
For many patients benign familial pemphigus is a mild condition, but for others, the pain and smell can be serious problems. Secondary bacterial infection, which is not uncommon, can give rise to an unpleasant smell. Herpes simplex can infect blistered sites and may evolve to widespread, painful viral infection (eczema herpeticum).
Usually, benign familial pemphigus is diagnosed by its appearance and family history, but it is often is mistaken for other skin problems. Impetigo, thrush, tinea cruris (jock itch) and other blistering conditions look similar.
Diagnosis may require a skin biopsy. The histology is characteristic, with layers of detached skin cells (‘acantholysis’) lining up like 'a row of tombstones'. Unlike pemphigus vulgaris, the immunofluorescence test for antibodies is negative.
As yet there is no diagnostic test available to family members.
There is no cure for Hailey-Hailey disease. Treatment is aimed at reducing symptoms and preventing flares.
Many patients have long remissions and an improvement with age does occur.