Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Matthew Scorer, Medical Student, Peninsula Medical School, United Kingdom, 2011.
Introduction Anticonvulsant drugs Adverse cutaneous reactions Genetic predisposition
Many drugs can cause cutaneous (skin) side effects. The severity of the symptoms can range from a mild rash to life-threatening conditions causing skin failure and death. Certain groups of drugs are known to cause frequent, specific, or serious skin reactions. The anticonvulsant or antiepileptic drugs are one such group of drugs, some of which have notable side effects on the skin.
Recognising the side effects that involve the skin is important, as prompt withdrawal of the drug can prevent worsening of symptoms caused by the drug. A decision may have to be made in a patient who has suffered a drug eruption whether to continue an important drug that might have caused the reaction or switch to an alternative drug.
When confronted by a new skin rash in a patient, a full drug history is paramount and should include prescribed, over-the-counter, and alternative medicines the patient is taking so that drug eruptions can be considered or ruled out.
Anticonvulsant drugs, also known as antiepileptic or antiseizure drugs, are a diverse group of medications that are commonly used in the treatment of epilepsy and seizures, and less commonly for other conditions such as trigeminal neuralgia and bipolar disorder. They work by reducing the excessive firing of neurons that happens in a seizure.
Types of skin reactions to anticonvulsant drugs |
|
|---|---|
Reaction |
Symptoms |
|
|
|
|
Target (iris) shaped lesions |
|
Usually develops within the first week of taking the drug |
|
Anticonvulsant hypersensitivity syndrome |
Symptoms usually develop 2-6 weeks after starting the drug but may happen at any time |
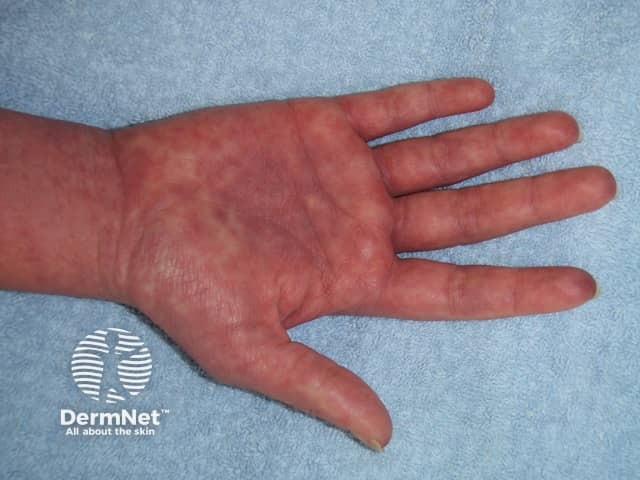
Morbilliform eruption
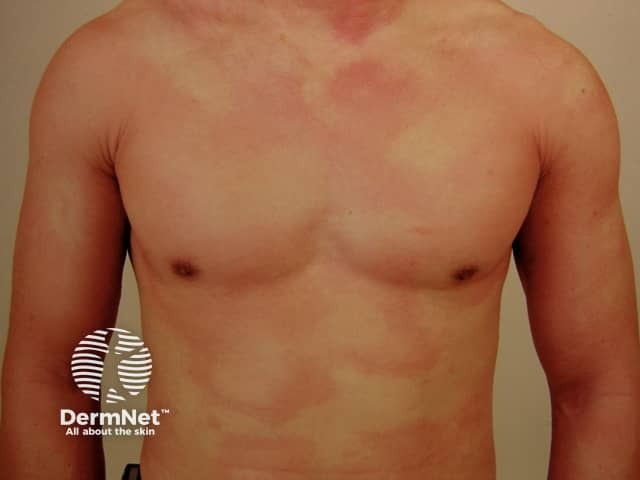
Urticaria
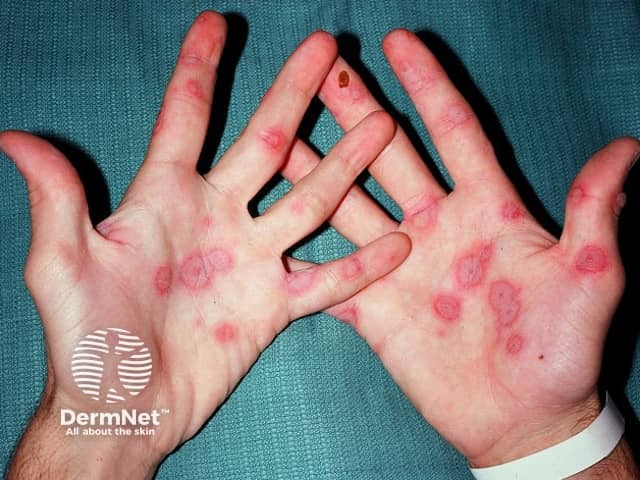
Erythema multiforme
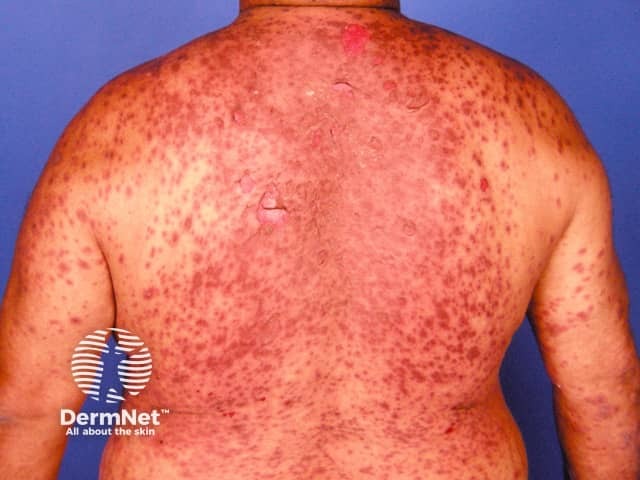
Toxic epidermal necrolysis
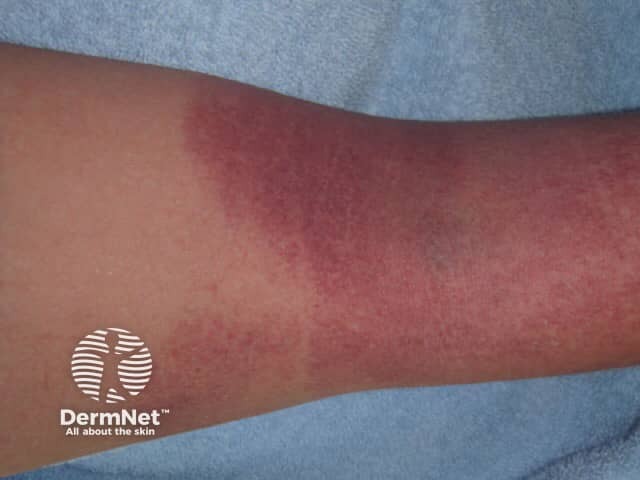
Purpuric eruption
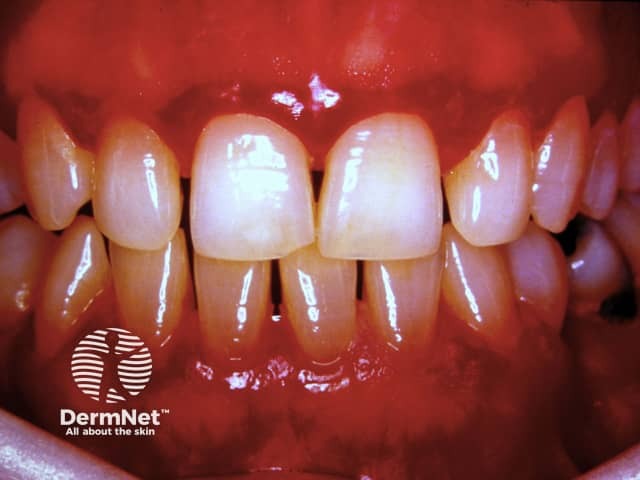
Gingival hyperplasia
Specific reactions to anticonvulsant drugs |
||
|---|---|---|
Drug |
Skin reaction |
Notes |
Carbamazepine |
Cutaneous side effects are the most common side effects causing discontinuation of carbamazepine |
|
Phenytoin |
|
5–10% of patients using phenytoin have a skin reaction |
Fosphenytoin |
|
Pruritus is present in 49% of patients and is dose related |
Phenobarbital |
||
Lamotrigine |
|
Life-threatening skin reactions occur in 1 in 100 children and 1 in 1000 adults treated with lamotrigine |
Valproic acid |
|
Interacts with other anticonvulsants such as lamotrigine, increasing the chance of side effects |
Some racial groups are especially prone to cutaneous adverse reactions with anticonvulsants. Testing for a particular allele prior to the commencement of an anticonvulsant may be useful in identifying patients at risk.