Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Selene Ting, Medical Registrar, Waitakere Hospital, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2020.
Introduction
Causes
Demographics
Hyperhidrosis-inducing drugs
Clinical features
Complications
Diagnosis
Treatment
Outlook
Hyperhidrosis is excessive sweating due to the overstimulation of the eccrine sweat glands by a neurotransmitter, acetylcholine [1]. Hyperhidrosis can be primary, which happens early in life, or secondary, which is caused by systemic or neurological diseases, or as a side effect of medications.

Excessive sweating in armpits
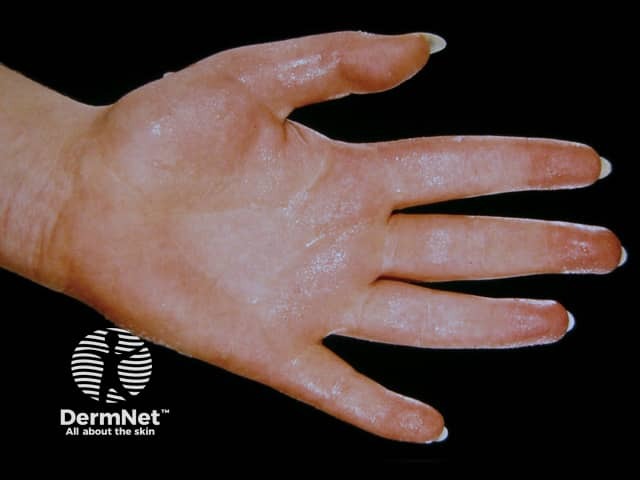
Palmar hyperhidrosis
Drug-induced hyperhidrosis is the most common cause of secondary hyperhidrosis. Drugs can act on the hypothalamus or at spinal thermoregulatory centres, at sympathetic ganglia or at the eccrine-neuroeffector junction [2]. It results from the release of acetylcholine by medications that block the action of acetylcholinesterase, an enzyme that breaks down the neurotransmitter [3].
Acetylcholine exerts its effect via receptors found on sweat glands. Due to impaired negative feedback to the hypothalamus, acetylcholine causes the body to sweat more than is needed for core temperature to reach homeostasis [2].
There are no specific characteristics that increase the risk of a person getting drug-induced hyperhidrosis. It can begin at any age, and affect people of all races [4].
Other factors that can contribute to increased sweating include a family history of increased sweating, and underlying medical conditions such as obesity, diabetes, hyperthyroidism, menopause, or cancer [4,5].
Different classes of medications can influence the sweating response by acting centrally in the brain and the peripheral nervous system [2,5,6].
Medications used to treat psychiatric conditions that can cause hyperhidrosis include:
Medications used to treat dementia or Parkinson disease include:
Pain relief medications that can cause hyperhidrosis include:
Antimicrobial medications and antibiotics that can cause hyperhidrosis include:
Medications that can affect endocrine function and thus cause hyperhidrosis can include:
Withdrawal from non-prescription drugs such as alcohol and caffeine can also cause generalised hyperhidrosis.
Primary hyperhidrosis tends to occur symmetrically at sites where there are concentrated eccrine glands, such as the armpits, palms, soles of feet, and face [1].
In contrast, sweating in drug-induced hyperhidrosis is more likely to be unilateral and asymmetrical, or generalised, affecting any part of the body.
While sweating tends to reduce at night in patients with primary hyperhidrosis, it can occur during sleep in drug-induced hyperhidrosis.
The Hyperhidrosis Disease Severity Scale [7] is a four-point questionnaire to assess the impact of the condition on a patient’s daily life by selecting from the following 4 options [8]:
Untreated hyperhidrosis can lead to skin infections, such as pitted keratolysis [9].
Drug-induced hyperhidrosis may lead to social embarrassment, lowered self-confidence, and emotional stress [1,7].
Drug-induced hyperhidrosis is diagnosed clinically. Other causes of secondary hyperhidrosis should be excluded, such as an underlying infection, malignancy, neurological, or endocrine conditions [5].
A temporal relationship between initiation of a certain medication and onset of symptoms with no other apparent cause of secondary hyperhidrosis is suggestive of drug-induced hyperhidrosis [7].
A physical examination can help exclude other causes. If hyperhidrosis is active on examination, the location and pattern of sweating can help to differentiate between primary or secondary causes.
There is no laboratory test to confirm drug-induced hyperhidrosis. The Minor starch-iodine test and gravimetric analysis can be used to confirm localised sweating, which points towards primary hyperhidrosis [7].
When suspicious of drug-induced hyperhidrosis, the possible culprit medication should be stopped completely as a trial. Other options are to reduce the dose, change to an extended-release formulation, or substitute with another medication less likely to cause sweating.
Treatments to suppress excessive sweating include [10]:
Drug-induced hyperhidrosis resolves when the causative medication is stopped.