Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Cindy Lam, University of Adelaide, South Australia. Copy edited by Gus Mitchell. July 2022.
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
Pitted keratolysis, also known as keratolysis plantare sulcatum or ringed keratolysis, is a superficial bacterial skin infection characterised by crater-like pits and malodour. It typically affects pressure-bearing areas on the soles of the feet, although the palms are rarely affected.
This condition is very treatable with a good prognosis.
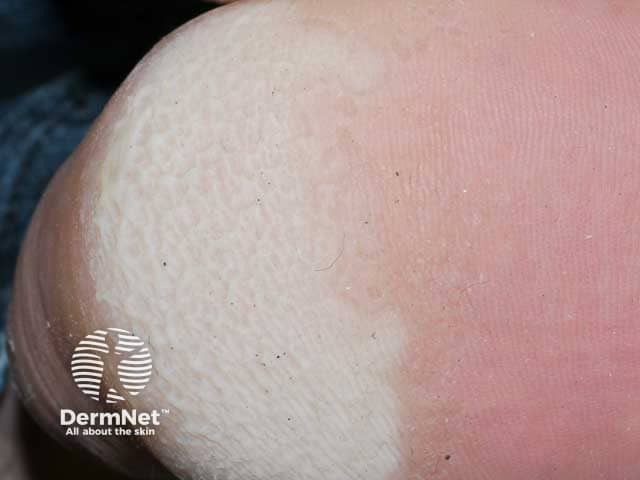
Pits and maceration in pitted keratolysis on the heel (PK-patient1)
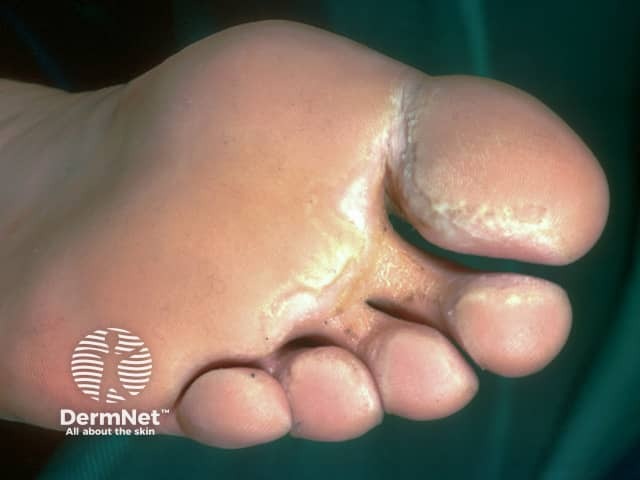
Interdigital and toe pitted keratolysis
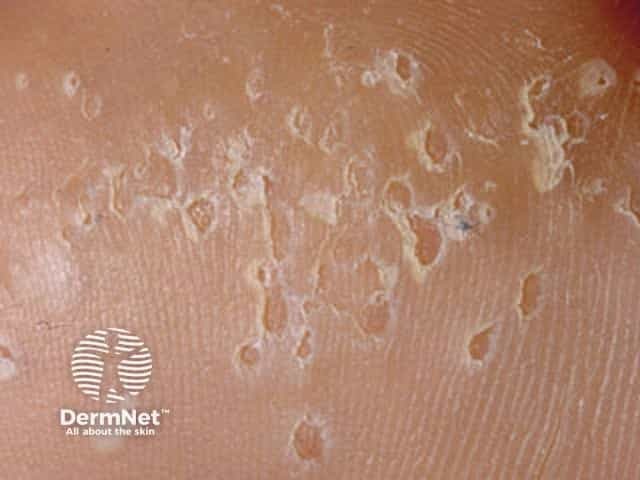
Close up of plantar pits in pitted keratolysis
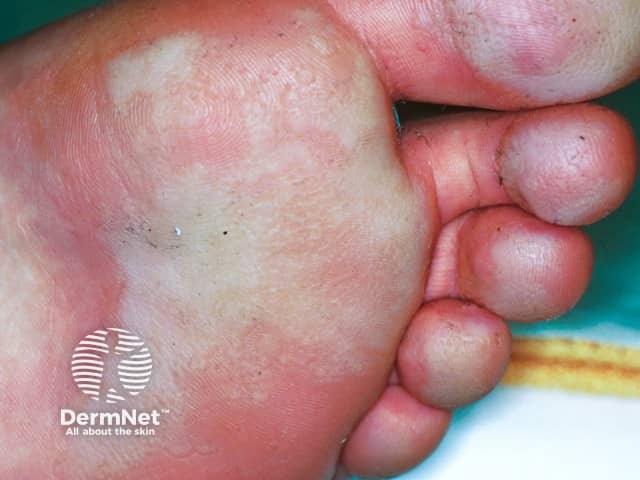
White macerated and pitting plantar skin in pitted keratolysis
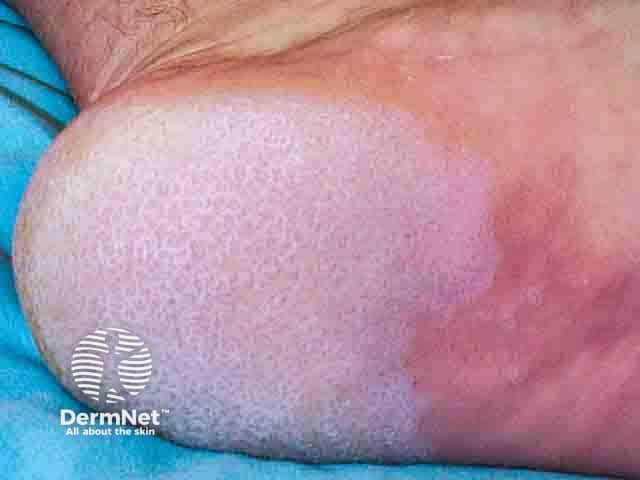
Heel maceration and pits in pitted keratolysis
Pitted keratolysis is more commonly seen in men compared to women and can affect all age groups.
Occupations at risk include:
Factors that increase the risk of developing pitted keratolysis include:
Pitted keratolysis is caused by a range of bacterial species. The most common are Corynebacteria, Dermatophilus congolensis, Kytococcus sedentarius, Actinomyces, or Streptomyces.
Bacteria thrive under moist and warm conditions. They proliferate and produce protease enzymes that cause destruction of the stratum corneum to create pits/craters. The odour is associated with the sulfur compounds (thiols, sulphides, and thioesters) which are produced by the bacteria.
The infection often occurs bilaterally on pressure-bearing areas, most commonly the ball of the foot and heel. Involvement of the palms have been reported in certain professions such as rice paddy farmers.
It is often asymptomatic, however, when symptomatic there may be associated pruritus and pain on walking.
Characteristic features include:
Associated features:
Variants of pitted keratolysis (less common):
Pitted keratolysis has been seen in patients of all skin types. They all present similarly and can present in a range of sizes and colours.
No mortality is associated with pitted keratolysis.
Diagnosis is often clinical given its distinctive appearance and malodour. Consider examination of intertriginous areas (axilla and groin) for co-existing corynebacterial infections, such as erythrasma and trichomycosis axillaris.
Other investigations that can be considered:
Pitted keratolysis can be treated successfully with adequate foot hygiene, topical antibiotics, and antiseptics.
Pitted keratolysis is treatable and has an excellent prognosis.