Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2005; Updated: Meghan Grossmann, Medical Student, Michigan State College of Osteopathic Medicine, Detroit MI, United States of America; Dr Martin Keefe, Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. October 2021.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Basal cell naevus syndrome is a rare genetic cancer syndrome characterised by multiple early onset basal cell carcinomas, odontogenic keratocysts and other tumours, and other abnormalities.
Basal cell naevus syndrome (BCNS) is probably best known as Gorlin syndrome, and is also called naevoid basal cell carcinoma syndrome, amongst many other names.
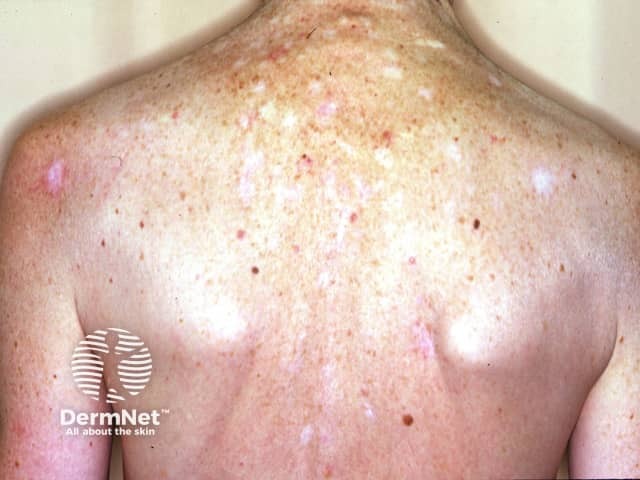
Multiple BCCs and scars

Palmar pits
Genetics of Basal cell naevus syndrome (Image courtesy Genetics 4 Medics)
Basal cell naevus syndrome is an autosomal dominant genetic disorder affecting males and females equally. Although seen in all races, race does influence incidence and penetrance with Gorlin syndrome rarely diagnosed in Black Americans and Asians. The prevalence is difficult to determine as although Gorlin syndrome has high penetrance, expressivity is variable and sporadic mutations are found in 50%. Estimates of prevalence range from 1/57,000 to 1/256,000.
Basal cell naevus syndrome is the result of genetic mutations affecting the sonic hedgehog signalling pathway, a pathway crucial for proper cell differentiation. Genes implicated in Gorlin syndrome include PTCH1, PTCH2, and SUFU.

Multiple BCCs and scars
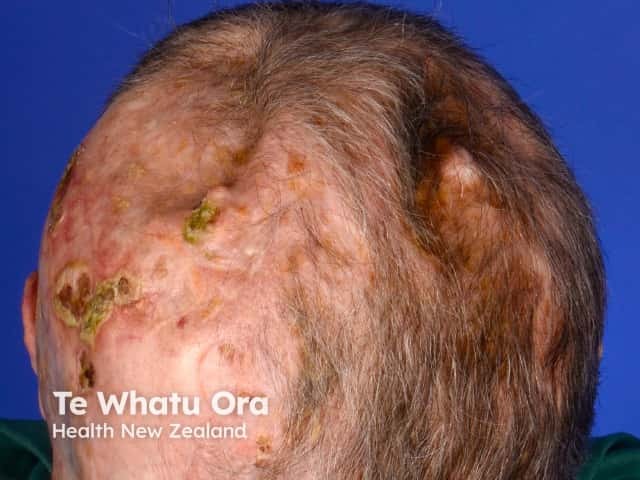
Scarring from surgeries to many basal cell carcinomas in basal cell naevus syndrome
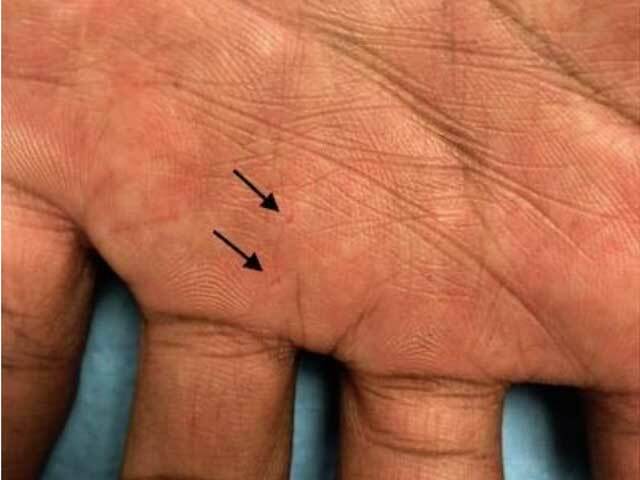
Basal cell naevus syndrome: palmar pits
Image Credit for palmar pits in skin of colour: Poladian K, Difato TC, Anderson KL, Taylor SL. Gorlin syndrome in a patient with skin type VI. Dermatol Online J. 2019;25(11):13030/qt64c4p1sq.
Basal cell carcinomas are seen in 80-90% of pale-skinned patients with Gorlin syndrome. Black patients may have < 2 skin cancers; 20% of dark-skinned Africans with Gorlin syndrome have none.
Basal cell naevus syndrome can be diagnosed on clinical criteria alone but may require investigations to confirm it in some cases, particularly in children. The BCC histology is the same as for sporadic BCC [see Basal cell carcinoma pathology].
The diagnosis is made if there are two major criteria, or one major and two minor criteria.
Basal cell naevus syndrome patients continue to develop new BCC throughout their life, with some patients having over 1000 BCC in their lifetime (median 8). Basal cell carcinomas can be clinically aggressive causing considerable morbidity and can be fatal. Life expectancy is generally believed to not otherwise be affected.