Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, New Zealand, 1997. Updated by: Dr Jacqueline Kim Nguyen, Resident, St Vincent’s Hospital, Australia. Copy edited by Gus Mitchell. August 2022
Introduction
Uses
Contraindications
How it works
Benefits and disadvantages
Side-effects and complications
Post-treatment care
Cryotherapy is a minimally-invasive treatment that freezes skin surface lesions using extremely cold liquid or instruments (cryogen).
Cryotherapy, also known as cryosurgery or cryoablation, can be delivered with various cryogens. Liquid nitrogen is the most common and effective cryogen for clinical use (temperature –196°C).
Other cryogens include:
Cryotherapy is an effective alternative to more invasive treatment options as it is inexpensive, simple, relatively safe, and can be performed quickly in an outpatient setting.
Benign lesions that may be treated by cryotherapy include:
Dermatologists can freeze small skin cancers such as superficial basal cell carcinoma (BCC) and in-situ squamous cell carcinoma (SCC) on the trunks and limbs, but this is not always successful, so careful follow-up is necessary.
Cryotherapy should not be used for:
Cryotherapy works by using a cryogen to cool the targeted lesion to sub-zero temperatures causing direct tissue necrosis. The thawing process induces osmolarity changes which also results in tissue damage.
Cryotherapy using liquid nitrogen involves the use of a cryospray, cryoprobe, or a cotton-tipped applicator. The dose, freeze-time, and delivery method depend on the location, depth, size, and tissue type of the lesion.
Liquid nitrogen spray methods include:
With the timed spot freeze technique, the spray gun is positioned 1 to 1.5cm above the centre of the skin lesion and sprayed until an ice ball encompasses the lesion (and required margin). The ice field is then maintained for 5 to 30 seconds depending on the lesion and depth of freeze. The treatment is repeated in some cases once thawing has completed. This is known as a ‘double freeze-thaw’.

A liquid nitrogen storage vessel - the room is ventilated and has an oxygen monitor. Gloves and goggles are used when filling smaller units for clinic use

Large cotton swabs used for cryotherapy
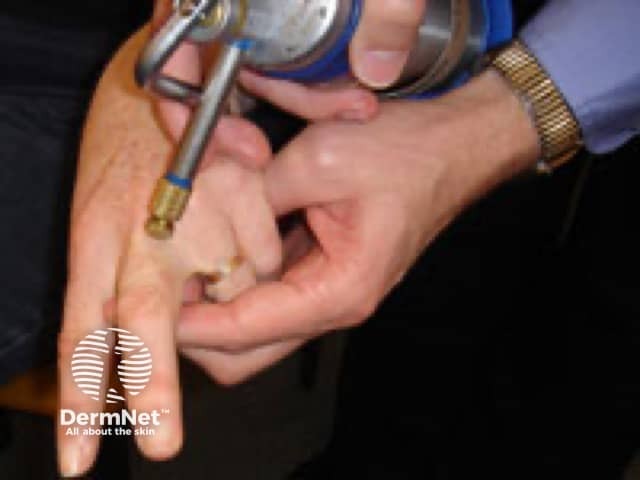
Cryotherapy spray
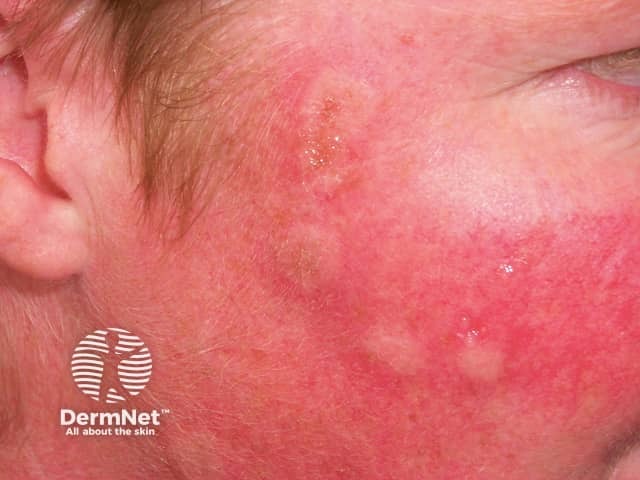
Redness and oedema 4 hrs after cryotherapy
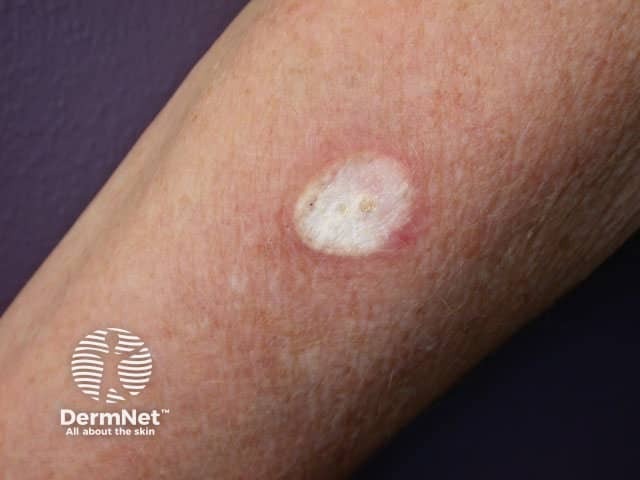
The ice ball just as the cryotherapy is discontinued – it will thaw in 15-30 seconds
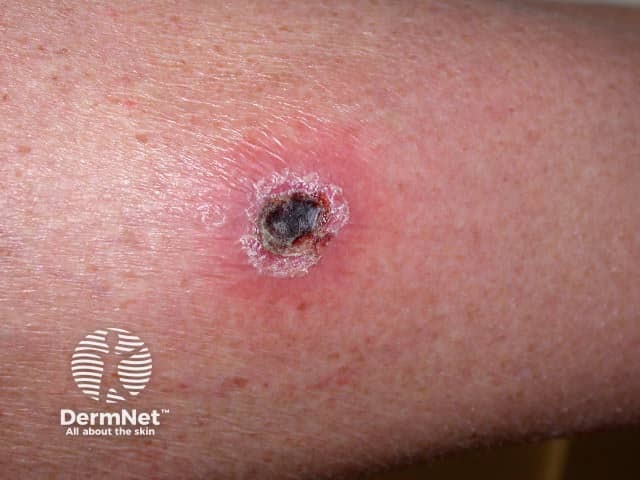
Cryotherapy eschar
Carbon dioxide cryotherapy involves making a cylinder of frozen carbon dioxide snow or a slush combined with acetone. It is applied directly to the skin lesion.
DMEP comes in an aerosol can and is often available over-the-counter. It is used to treat warts using a foam applicator pushed onto the skin lesion for 10–40 seconds, depending on its size and site.
Cryotherapy is a simple and relatively safe procedure, however, it can require several treatments to work. The resultant pain can also hinder compliance.
Benign lesions secondary to sun damage can be highly amenable to cryosurgery.
Clearance rates of verrucous lesions can vary depending on the degree of hyperkeratosis and size of the wart.
Several treatment sessions may be needed and the overall cure rate varies from 39% to 84% at three months.
Favourable response rates have been reported with keratolytic pre-treatment.
Cryosurgery is not a first-line treatment for cancerous lesions such as BCCs and SCCs, but is an option for low-risk lesions.
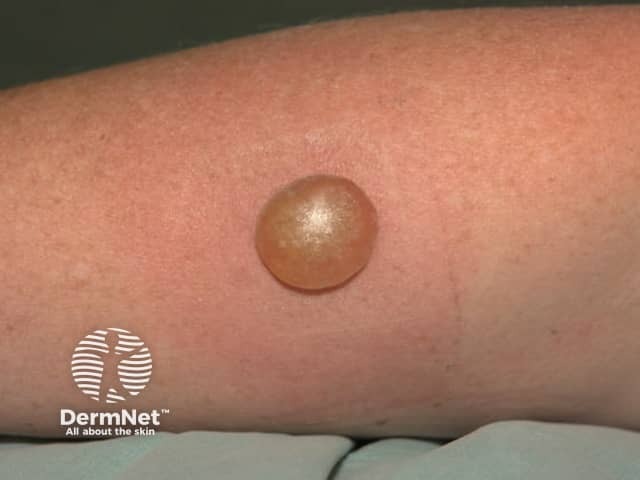
A cryotherapy blister 48 hrs after treatment
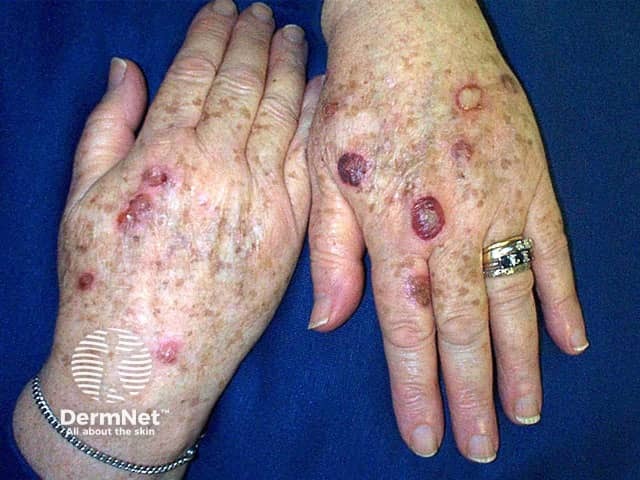
Haemorrhagic blisters 3 days after treatment
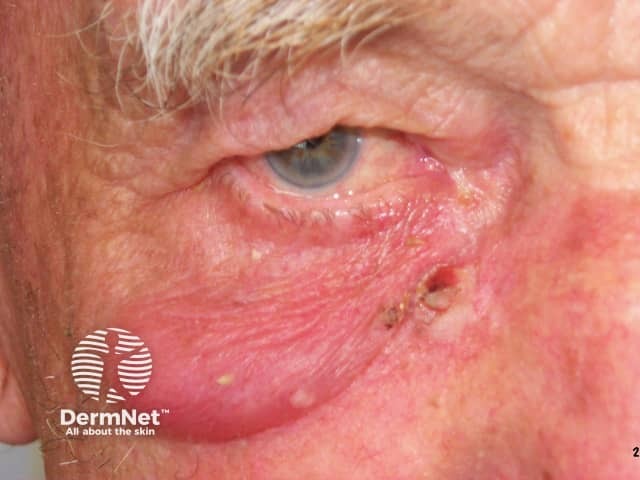
Eyelid oedema 24 hrs after cryotherapy to the lesion adjacent to the nose
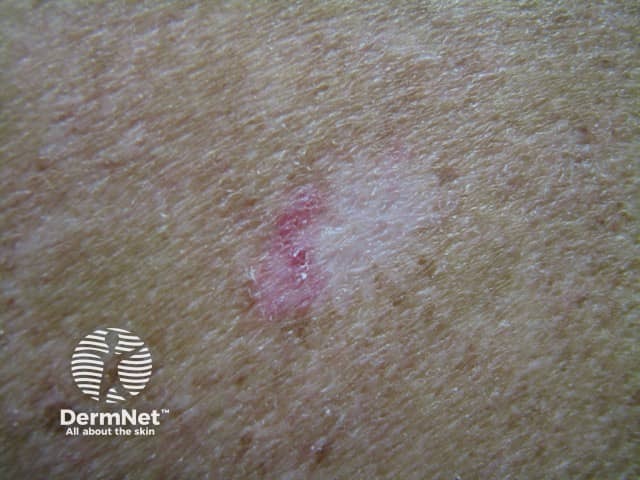
Recurrent BCC post-cryotherapy
It is important to provide patients with postoperative wound care instructions and complications to be aware of.
Usually, no special attention is needed during the healing phase. The treated area may be gently washed once or twice daily with soap and water and should be kept clean. A dressing is optional but is advisable if the affected area is subject to trauma or clothes rub on it.
Immediate swelling and redness may be reduced by:
The treated area is likely to blister within a few hours, depending on the depth and duration of the freeze. It may contain clear fluid or blood (this is harmless).
Treatment near the eye may result in a puffy eyelid, especially the following morning, but the swelling settles within a few days. A scab will then form and the blister gradually dries up.
When the blister dries to a scab, apply petroleum jelly and avoid picking at the scab. The scab peels off after 5–10 days on the face and 3 weeks on the hand. A sore or scab may persist as long as 3 months on the lower leg because healing in this site is often slow.