Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Types Demographics Clinical features Skin manifestations Other manifestations Treatment
Cryoglobulinaemia is a rare disorder characterised by the presence of abnormal immunoglobulin proteins in the blood that can precipitate out into tissues at low temperatures and causing inflammation and damage.
Immunoglobulins are the class of proteins that make antibodies in response to foreign substances (antigens) introduced into the body. In the case of cryoglobulinaemia, the abnormal immunoglobulins form complexes (cryoglobulins) and precipitate (leach) out of the blood at cold temperatures. This causes restricted tissue blood flow and systemic inflammation, which leads to many clinical signs and symptoms including skin lesions, arthralgia (joint pain), arthritis, vascular purpura (purple skin marks), livedo (marbling pattern), and bleeding conditions.
Cryoglobulinaemia often occurs in association with other diseases, particularly autoimmune or infectious diseases (this is known as secondary cryoglobulinaemia). When it occurs without an associated disease it is called idiopathic or essential cryoglobulinaemia.
Cryoglobulinaemia is classified into 3 major types based on the make-up of the cryoglobulin complex. Each type has been found to be associated with certain diseases.
Cryoglobulin type |
Immunoglobulin composition |
Associated diseases |
|---|---|---|
Type I: single monoclonal antibody |
Mainly IgM |
Waldenström's macroglobulinaemia |
Type II: mixed antibody with monoclonal rheumatoid factor (usually IgG or IgM) |
IgM-IgG |
Waldenström macroglobulinaemia |
Type III: mixed antibody with polyclonal rheumatoid factor |
IgM-IgG |
Systemic lupus erythematosus |
Cryoglobulinaemia is thought to be rare. Essential mixed cryoglobulinaemia occurs in about 1 in 100,000 people. Most cases of cryoglobulinaemia have an underlying cause. The type of cryoglobulinaemia found in patients is roughly 25% with type I, 25% with type II and 50% with type III.
It tends to develop between 40-60 years of age and affect females more than males by 3:1.
The clinical features of cryoglobulinaemia differ between the types as shown in the table below.
Features of Type I cryoglobulinaemia |
Features of Type II and III cryoglobulinaemia |
|---|---|
|
|
Skin problems are almost always present in patients with cryoglobulinaemia.
Skin problem |
Type I (%) |
Types II and III (%) |
|
|---|---|---|---|
Ischaemic necrosis (skin and tissue damage due to lack of blood flow) |
40 |
0-20 |
|
15 |
80 |
||
1 |
14 (in type III) |
||
15 |
10 (in type III) |
||
Scarring of the tip of nose, pinnae, fingertips and toes |
|||
Nailfold capillary abnormalities |
|||
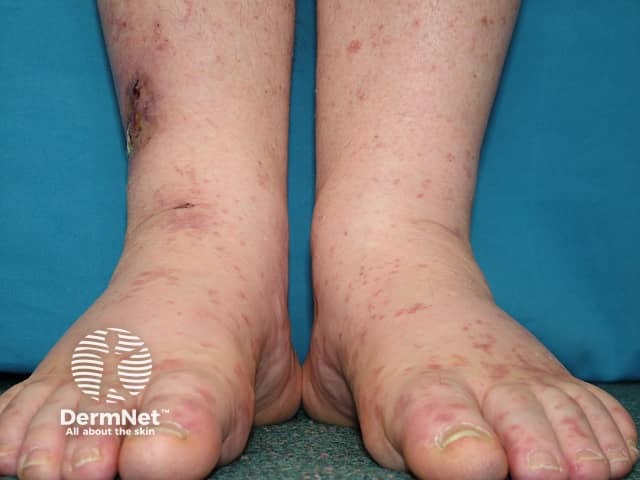
Cryoglobulinaemia
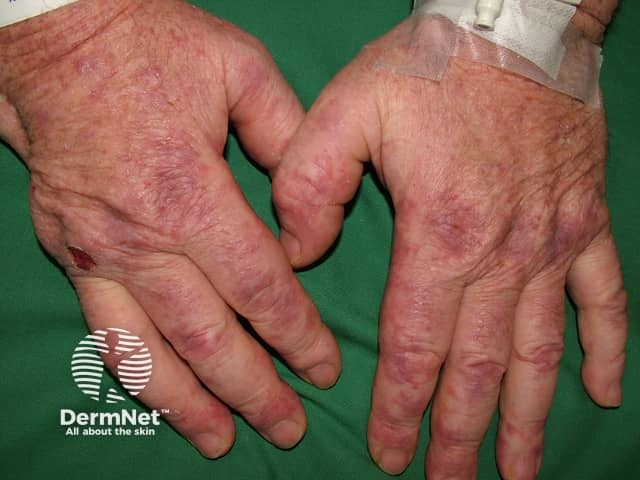
Cryoglobulinaemia
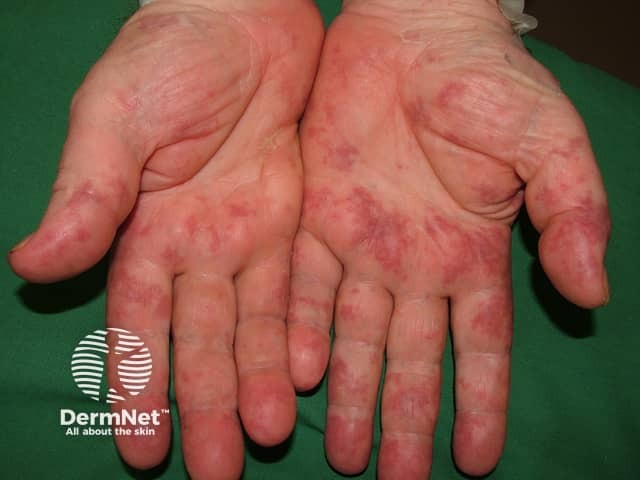
Cryoglobulinaemia
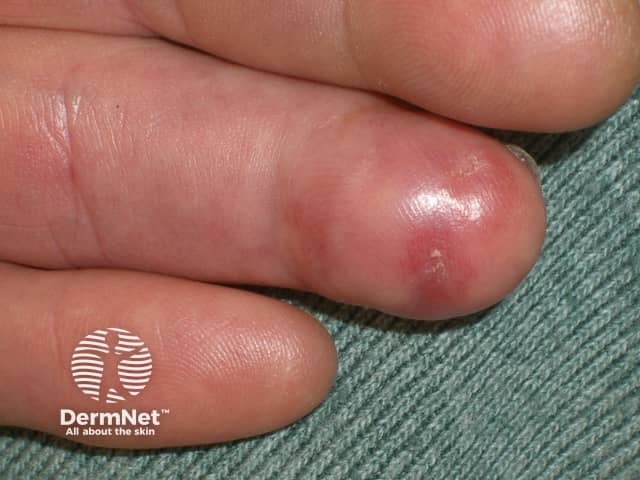
Cryoglobulinaemia
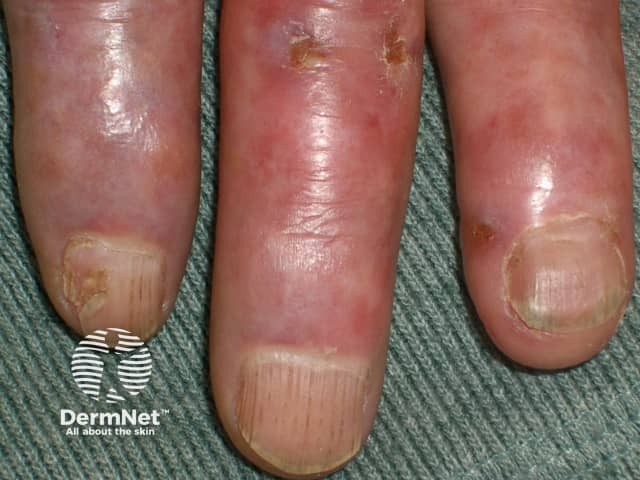
Cryoglobulinaemia
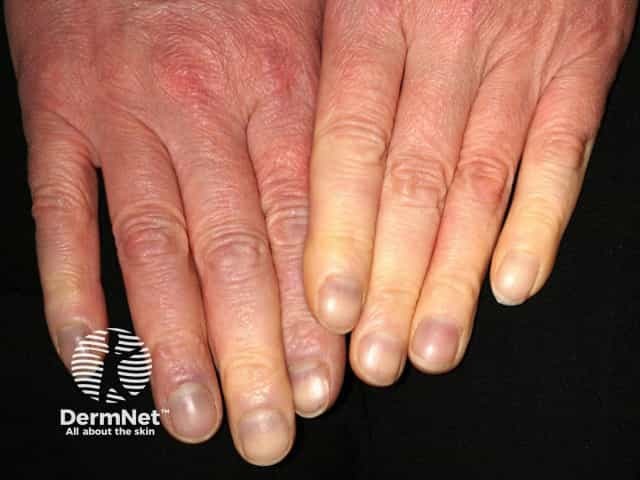
Raynaud phenomenon
Many organs may be affected by cryoglobulinaemia.
Affected organ |
Signs and symptoms |
|
|---|---|---|
Lungs |
A cough, shortness of breath, fluid in the lungs |
|
Gastrointestinal |
Stomach pain, bleeding, enlarged liver and/or spleen |
|
Kidneys |
Hypertension (high blood pressure), glomerulonephritis, nephrotic syndrome |
|
Nervous system |
Visual disturbances, peripheral neuropathy |
|
Fever may also occur.
The main aim of therapy is to find and treat the underlying cause and limit precipitation of cryoglobulins and the inflammation that results. Patients with cryoglobulinaemia should be advised to avoid cold environments to prevent triggering the precipitation of cryoglobulins.
Symptomatic treatment includes:
Identification and treatment of early symptoms such as skin lesions, fatigue or arthralgia, as a result of cryoglobulinaemia, will prevent further organ damage and improve patient outcomes.