Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern/Gus Mitchell. July 2017.
Introduction Uses Contraindications Benefits Drawbacks Side effects
The term plasmapheresis describes a procedure in which blood components (ie, white blood cells, red blood cells, platelets and plasma) are separated through a wide-bore central intravenous line, either via centrifuge or a semipermeable membrane separation technique. It can be repeated every few days on several occasions.
In therapeutic plasmapheresis (also known as plasma exchange) using a centrifuge:
In comparison, plasmapheresis via a membrane separation technique:
Plasma exchange can also involve:
Plasmapheresis removes autoantibodies, immune complexes, complement and non-specific inflammatory mediators. It is primarily used in severe autoimmune or cytotoxic diseases.
It has been used for a variety of haematological, rheumatological, metabolic, dermatological, neurological and renal conditions. Clinical evidence is strongest for the use of plasmapheresis in Guillain–Barrée syndrome, myasthenia gravis, thrombotic thrombocytopenic purpura, Goodpasture syndrome and fulminant Wilson disease.
Plasmapheresis is not often used in dermatology; it is used mainly experimentally for the following disorders:
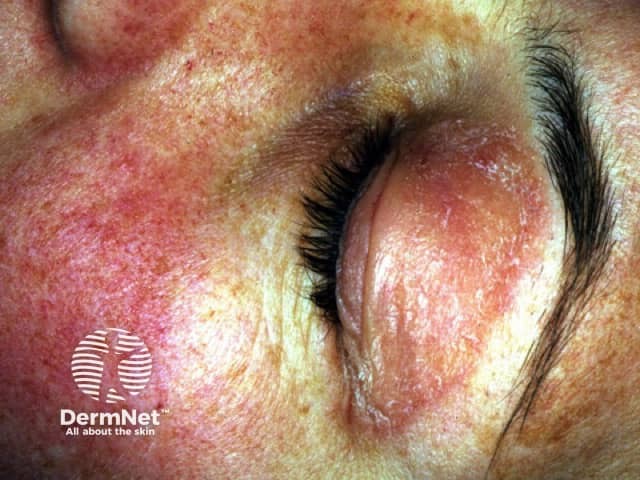
Dermatomyositis
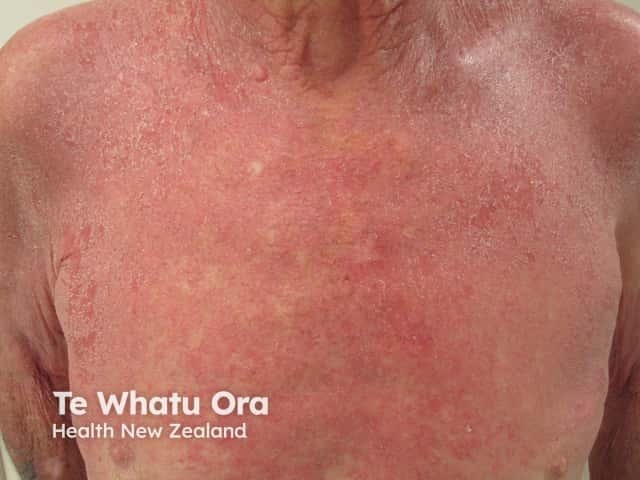
Erythroderma
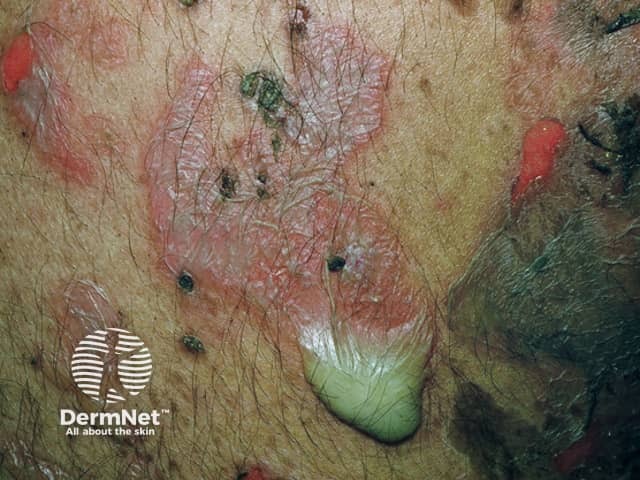
Pemphigus
Plasmapheresis is contraindicated in patients who:
The theoretical benefits of plasmapheresis in treating skin diseases include:
Plasmapheresis is not in common use. It is not widely available as it requires a team of experienced clinicians, and it is thus expensive to perform.
Complications and risks of plasmapheresis can include: