Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Systemic diseases Autoimmune/autoinflammatory
Author: Dr Shilpa Manupati and Dr Farazmand Paymaneh, Speciality Doctors in Dermatology, U.K. (2022)
Previous contributors: Vanessa Ngan (2003)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Prevention Outcome
Paraneoplastic pemphigus (PNP) is a rare, autoimmune, mucocutaneous, blistering disease that is almost always associated with a confirmed or occult neoplasm.
Paraneoplastic autoimmune multiorgan syndrome (PAMS) is another proposed name for PNP due to potential autoimmune reactions also appearing in internal organs, such as bronchiolitis obliterans in the lung.
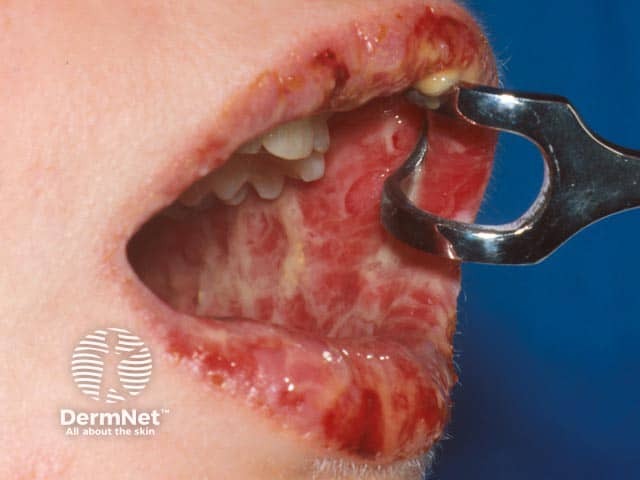
Severe oral paraneoplastic pemphigus due to an underlying Castleman tumour
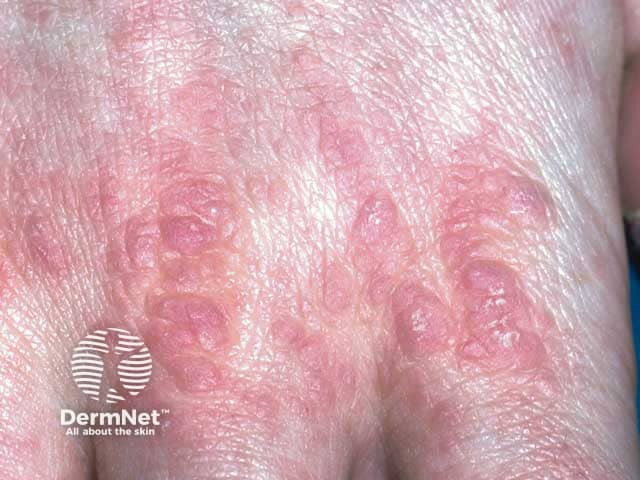
Lichenoid lesions on the hand in paraneoplastic pemphigus associated with Castleman disease
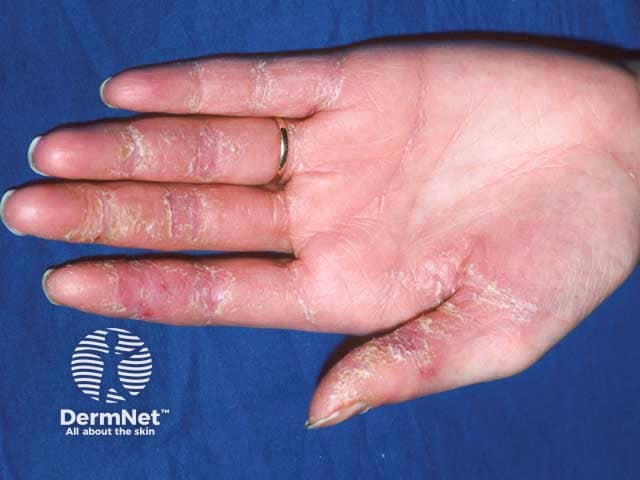
Palmar changes in paraneoplastic pemphigus associated with Castleman disease
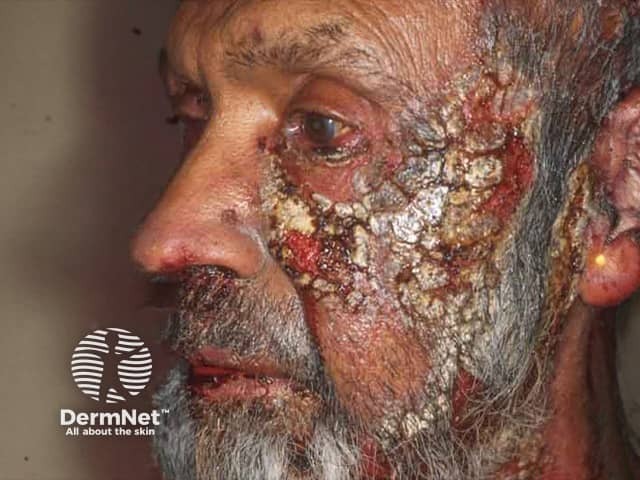
Facial paraneoplastic pemphigus due to tonsil lymphoma
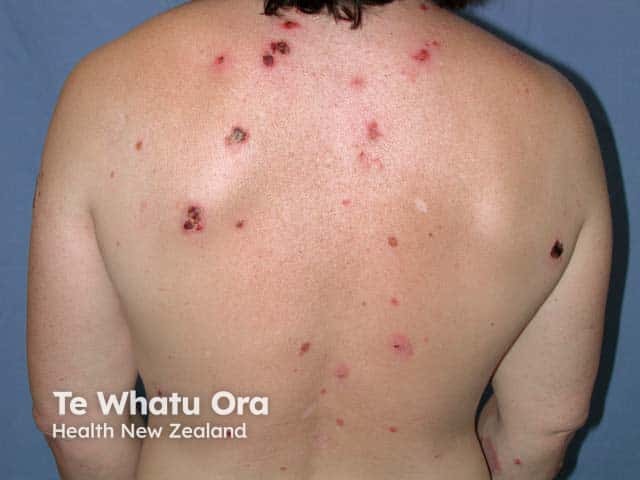
Erosions over the torso in paraneoplastic pemphigus (PNP-patient2)
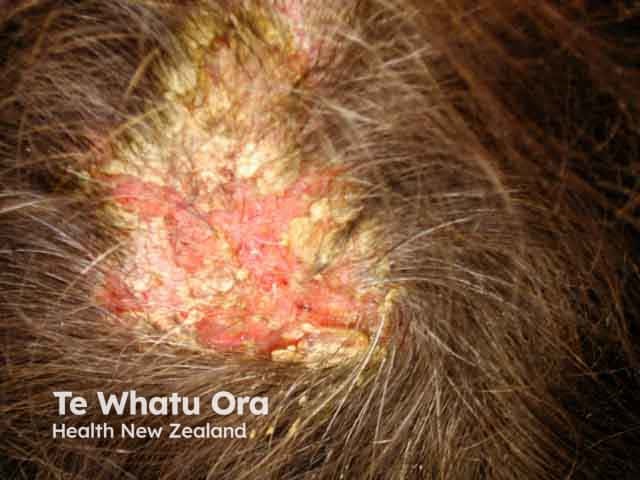
Scalp crusting and erosions in paraneoplastic pemphigus (PNP-patient1)
PNP is a rare autoimmune bullous disease variant; it is the least common but most serious form of pemphigus, accounting for 3–5% of all cases. Though PNP most commonly develops in adults between 45–70 years of age with equal male and female sex predilection, it is also seen in children.
Almost all cases of PNP are associated with an underlying cancerous (malignant) process:
The cause of PNP is not completely understood, but it appears that underlying malignancy (most commonly a lymphoproliferative neoplasm) stimulates an autoimmune response:
Genetic factors also play a role in the autoimmune response:
Clinical features may include:
There are five major clinical subtypes of PNP, likely linked to the range of auto-antibodies:
PNP is diagnosed based on a combination of clinical and histological findings, along with direct and indirect immunofluorescence, and immune serology.
Once PNP is diagnosed, a thorough search for any underlying malignancy is important.
There are two types, which may overlap depending on clinical phenotype.
The optimal treatment for PNP is debated, and response to therapy is variable; treatment options may include:
Management of the underlying malignancy by surgical excision or appropriate chemotherapy, radiotherapy, or immunotherapy will be required.
Because PNP is almost always associated with underlying cancer, particularly haematological cancers such as lymphoma and leukaemia, prevention is not straightforward.
Surgical resection of solid tumours (especially solitary Castleman tumours) with pre- and post-surgery use of high-dose IVIG can lower the risk of bronchiolitis obliterans in patients with PNP.
PNP has a poor prognosis with a mortality rate ranging from 70–90%. The erythema multiforme-like subtype of PNP appears to be associated with a worse prognosis. Causes of death include widespread infections, progression of malignancy, or bronchiolitis obliterans. Treatment with a variety of therapies may improve the prognosis of PNP.