Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Reactions Autoimmune/autoinflammatory
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. June 2017.
Introduction - pemphigus
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outcome
Pemphigus refers to a group of autoimmune diseases that cause blistering. Pemphigus is characterised by the development of antibodies directed against a protein (either desmoglein 1, desmoglein 3 or both) involved in cell-to-cell adherence in the epidermis.
Types of pemphigus include:
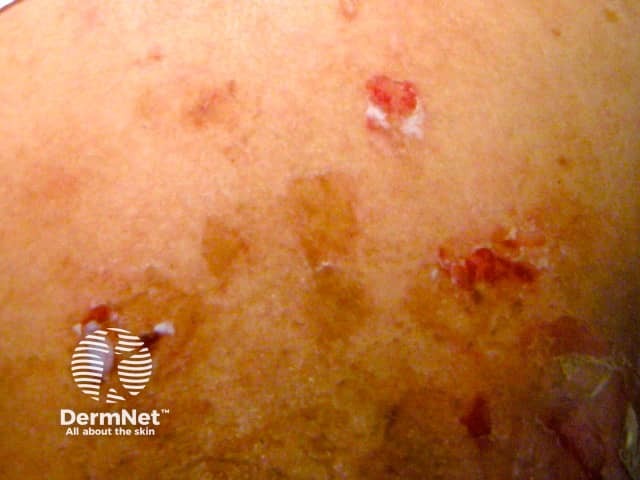
Drug-induced pemphigus foliaceus
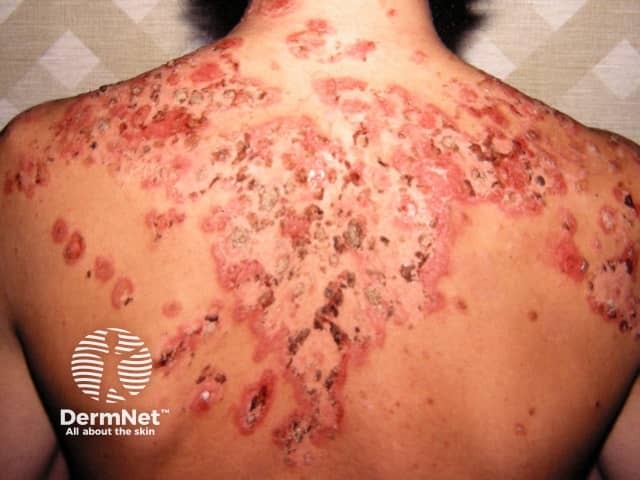
Pemphigus foliaceus
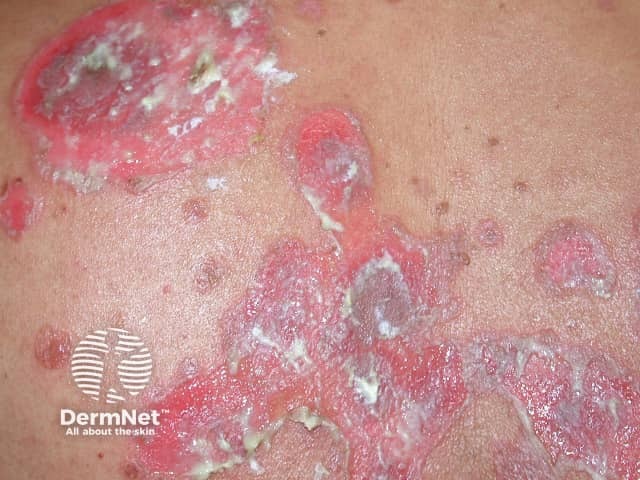
Pemphigus vulgaris
Drug-induced pemphigus is diagnosed when a form of pemphigus has been precipitated by a medication. Pemphigus may occur days, weeks, or as long as 6 months after the drug has been commenced.
Over 200 cases of drug-induced pemphigus have been reported in the medical literature. The reports suggest that patients with drug-induced pemphigus may have similar characteristics to non-drug-induced pemphigus.
In some cases, the drug triggers the re-activation of pre-existing pemphigus in remission.
Drugs that cause pemphigus include:
Pemphigus can also be induced by the topical application of drugs such as imiquimod, ketoprofen, neomycin, and bacitracin. Tincture of benzoin and chromium sulphate have also been reported to cause 'contact pemphigus', defined as pemphigus occurring at the site of contact with a topical agent.
Drug-induced pemphigus is usually caused by the induction of an immune reaction to desmoglein proteins and it is identical to the idiopathic forms of pemphigus. In some cases, when no antibodies to desmoglein have been detected, a biochemical cause for the drug-induced pemphigus has been suspected.
The clinical features depend on whether the drug-induced pemphigus has been induced by thiol or non-thiol drugs.
Thiol drugs cause pemphigus foliaceus.
Non-thiol drugs most commonly cause pemphigus vulgaris.
The diagnosis of drug-induced pemphigus can be challenging, especially in patients on multiple drugs as the period between the ingestion of the causative drug and the onset of symptoms can be prolonged. Careful, thorough history-taking is vital.
The diagnosis of pemphigus is confirmed by its characteristic intraepidermal blistering when seen on histology of a skin biopsy, and the presence of typical antibodies on direct immunofluorescence. Circulating pemphigus antibodies against desmoglein 1 and/or desmoglein 3 may be detected on serology.
The outcome for drug-induced pemphigus depends on whether the patient has developed antibodies and whether the cause of the condition is a thiol or non-thiol drug.