Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated: Dr Amy Stanway, Dermatologist, Tauranga, New Zealand. Copy edited by Gus Mitchell. September 2021.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Pemphigoid gestationis is a rare pregnancy-associated autoimmune blistering skin condition.
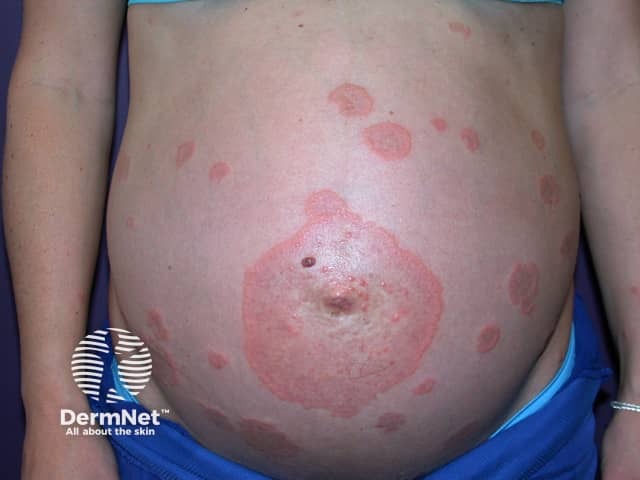

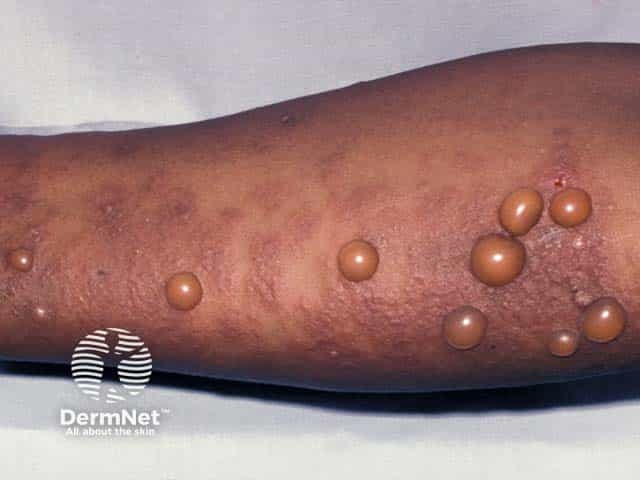
Pemphigoid gestationis affects women of all races during pregnancy or shortly after delivery. The median age of onset is 26–32 years (range 17–41 years). It may develop during the first pregnancy or appear for the first time in a multiparous woman.
Pemphigoid gestationis occurs in approximately 1 in 50000 pregnancies. It may rarely present in association with trophoblastic tumours such as choriocarcinoma or hydatidiform mole.
Pemphigoid gestationis usually develops during the second and third trimesters of pregnancy or the immediate postpartum period. Onset may be earlier in subsequent pregnancies.
Pemphigoid gestationis is an autoimmune disease, which means a woman’s immune system is attacking a normal component of her own skin.
In pemphigoid gestationis, PG factor, a specific immunoglobulin type G (IgG) in the blood, binds to the BP-180 protein located in the basement membrane of the skin leading to tissue damage and blistering. The usual function of BP-180 is to help stick the epidermis and dermis together, so the blister split is in the basement membrane [see Structure of normal skin].
BP-180 protein is also found in the placenta. It appears it is the placenta, not the skin, that triggers the autoimmune response in pemphigoid gestationis, which explains why this condition starts in pregnancy.
Pemphigoid gestationis is strongly associated with maternal MHC class II antigens haplotypes HLA-DR3 and HLA-DR4. As in other autoimmune conditions, pemphigoid gestationis is associated with an increased risk of other organ-specific autoimmune diseases, in particular Graves disease [see Pretibial myxoedema].
Pemphigoid gestationis typically presents as an intensely itchy urticaria-like rash during mid to late pregnancy (13–40 weeks gestation).

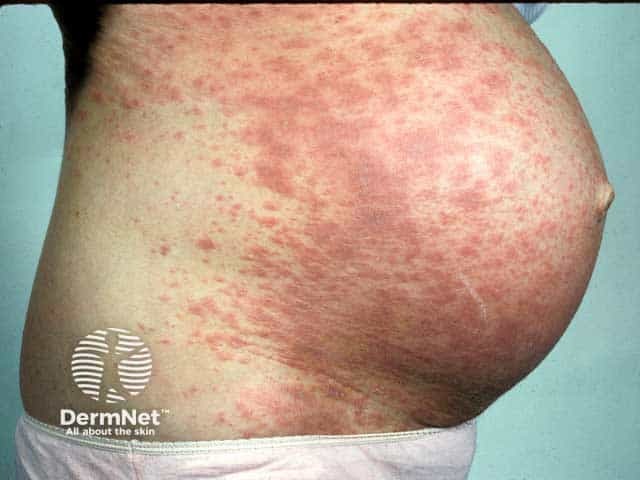



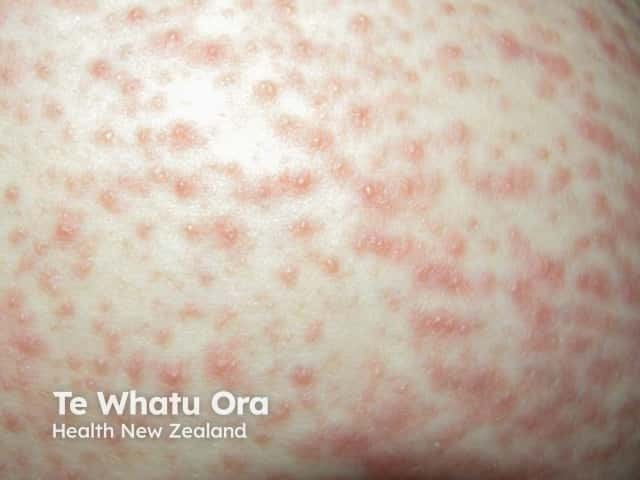



Pemphigoid gestationis is usually a clinical diagnosis when the features are typical, but in the early stages it can be indistinguishable from other pregnancy eruptions. Blood tests and skin biopsy may be required.
The aim of treatment in pemphigoid gestationis is to relieve itch, prevent blister formation, and treat secondary infection.
Pemphigoid gestationis follows a fluctuating course of exacerbations and remissions during pregnancy. It frequently improves in late pregnancy followed by a flare at the time of delivery in 75% of patients. After delivery, the lesions usually resolve within weeks or months. Rarely, pemphigoid gestationis can persist for several years. A systematic review found 80% of women were in complete remission 9 months post-partum, but half were still requiring treatment.
Pemphigoid gestationis usually recurs with subsequent pregnancies, although there may be unaffected pregnancies in between. Skin changes may recur with menstruation and hormonal contraception.