Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Chloe Jiang, 5th Year Medical Student, University of Auckland, New Zealand; Chief Editor: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2016.
Demographics Skin problems treated by oral contraceptives How they work Skin problems caused by oral contraceptives Contraindications
An oral contraceptive, or birth control pill, is a medication that prevents pregnancy. They contain either two hormones combined (oestrogen and progestin) or a single hormone (progestin).
OCPs suppress ovulation and thicken cervical mucus (which stops sperm getting into the womb).
Oral contraceptives are mainly used by women of childbearing age for birth control. They also have non-contraceptive health benefits.
Oral contraceptives are used to treat signs of hyperandrogenism in women. The associated skin problems are
Hyperandrogenism refers to an excess of male hormone either in the circulation or due to increased sensitivity of individual pilosebaceous cells (hair follicle and sebaceous gland).
Women with signs of hyperandrogenism should be evaluated for underlying disorders such as polycystic ovarian syndrome, congenital adrenal hyperplasia, adrenal or ovarian tumours.
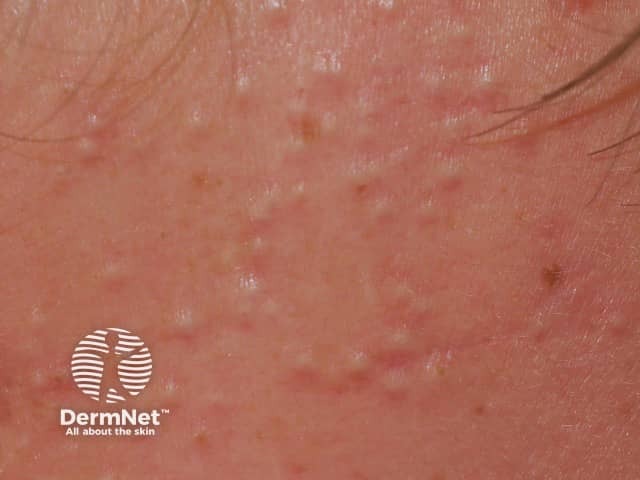
Comedonal acne
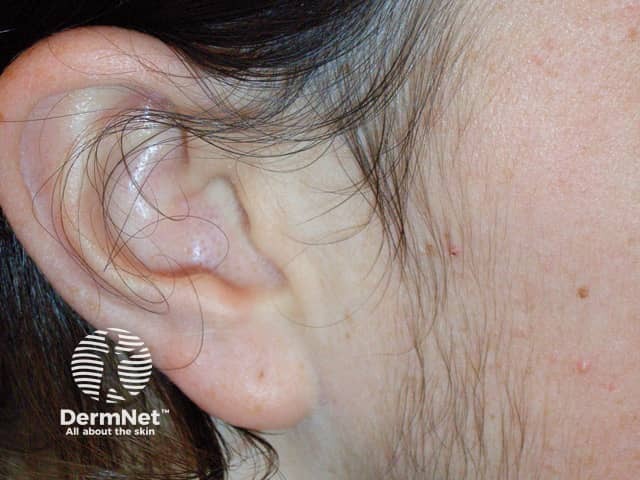
Hirsutism
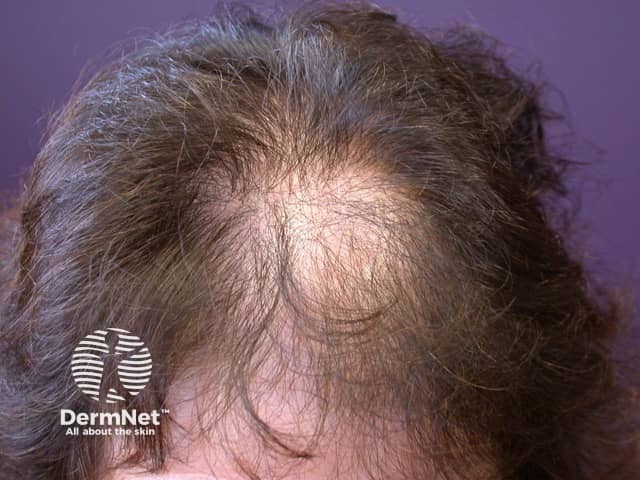
Female pattern alopecia
Combined oral contraceptives suppress luteinising hormone (LH)-driven androgen production and increase sex hormone binding globulin. The result is a decrease in the levels of free androgen leading to improvement in acne and reduction in excess hair growth
The action of combined oral contraceptives depends on their oestrogen-progestin balance. Progestins are weak androgens.
In a combined oral contraceptive, the effects of the oestrogen outweigh the effects of the progestin, so androgen levels decrease overall.
Progesterone-only oral contraceptives (the minipill) are not effective in the management of androgen-mediated skin conditions and can make acne worse.
Skin problems sometimes caused by oral contraceptives include:
Before starting oral contraceptives, especially oestrogen-containing OCPs, patients should be questioned regarding any possible contraindications, due to the risk of adverse effects. These include thromboembolism (blood clots) and liver disease.