Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Signs and symptoms Diagnosis Treatment
Polycystic ovary syndrome (PCOS) is characterised by menstrual irregularities/abnormalities, hirsutism (male-like hairiness in women), obesity and metabolic syndrome, resulting from abnormalities in the metabolism of androgens and oestrogen and in the control of androgen production. It was once thought to be mainly due to an ovarian defect as it was often associated with enlarged polycystic ovaries, hence its name polycystic ovary syndrome. However, it is now known that PCOS may occur in women with normal sized ovaries and polycystic ovarian changes can be found in women with normal menstrual cycles.
PCOS occurs in women only and generally starts at around puberty. It is estimated to affect 3-10% of women. Although the signs and symptoms are similar in most patients, different races can be affected differently. For example, in the US, 70% of patients have hirsutism compared to 10-20% in Japan.
The exact cause of PCOS is not yet known but is thought to develop when the ovaries overproduce androgen hormones (e.g. testosterone). This is caused by the overproduction of luteinizing hormone (LH), which is produced by the pituitary gland. People with PCOS also have an inability to process insulin effectively. This is known as peripheral insulin resistance. It is more of a problem in obese patients. Elevated insulin levels also have an effect on ovarian function.
There are many signs and symptoms associated with PCOS.
The diagnostic criteria for PCOS include two out of three of:
If the doctor is suspicious of PCOS, blood tests may be ordered. These may include:
A pelvic ultrasound examination and/or CT scan or magnetic resonance imaging (MRI) may be useful to detect ovarian or adrenal tmours if levels of testosterone are very high.
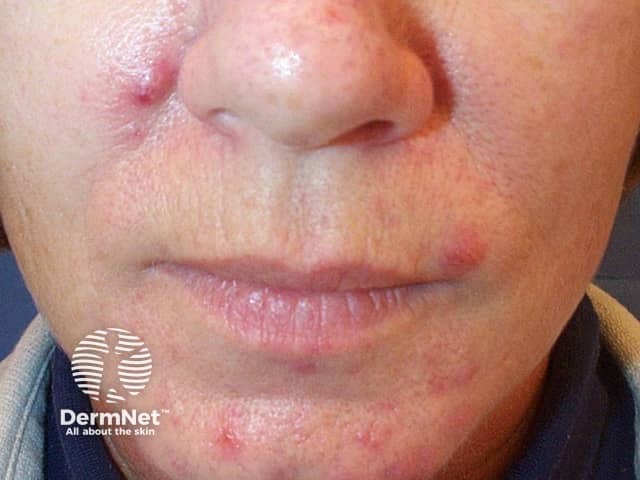
Polycystic ovarian syndrome
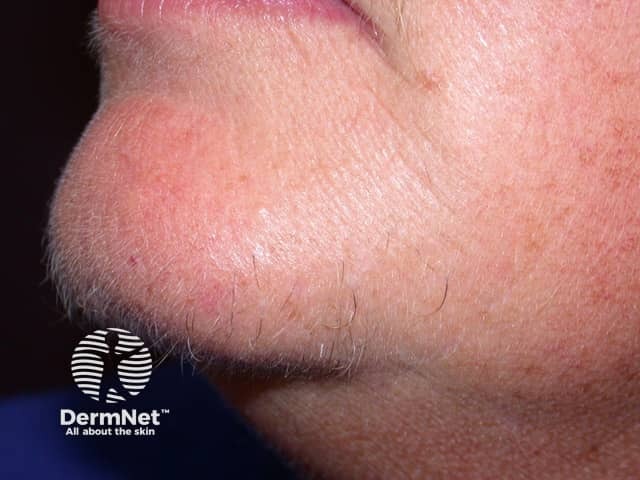
Hirsutism
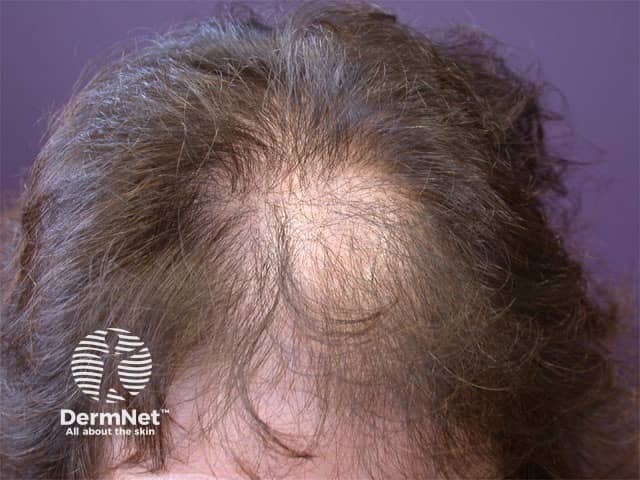
Polycystic ovaries
In the past, management of the condition was directed at treating individual symptoms of PCOS, such as hirsutism, acne or fertility. More recently with the understanding that insulin resistance has a large part to play in the development of PCOS, treatment has shifted towards correcting insulin resistance, which in turn improves many other symptoms of the condition.
In addition to the above treatments, specific treatments are used to gain overall control of symptoms.
Book: Textbook of Dermatology. Ed Rook A, Wilkinson DS, Ebling FJB, Champion RH, Burton JL. Fourth edition. Blackwell Scientific Publications