Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2017. Revised September 2020.
Introduction - angioma
Introduction - cherry angioma
Demographics
Causes
Clinical features
Differential diagnoses
Investigations
Treatment
Angioma or haemangioma (American spelling ‘hemangioma’) describes a benign vascular skin lesion. An angioma is due to proliferating endothelial cells; these are the cells that line the inside of a blood vessel.
Angiomas can arise in early life (infantile haemangioma) or later in life; the most common type of angioma is a cherry angioma.
A cherry angioma is a small papular angioma. It is a true capillary haemangioma. Cherry angioma has many synonyms, the most commonly used being Campbell de Morgan spots.
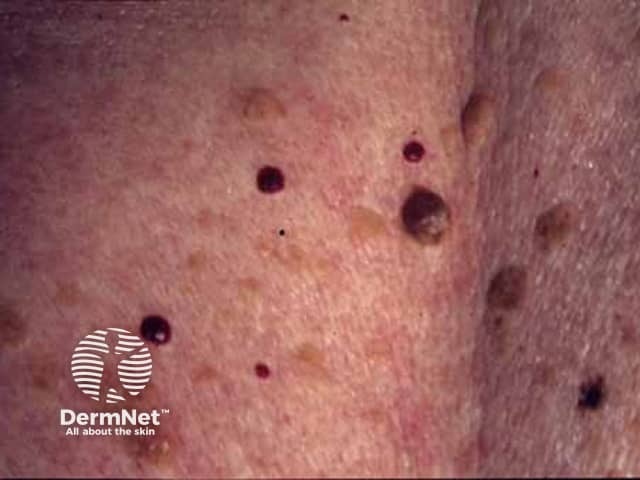
Cherry angiomas
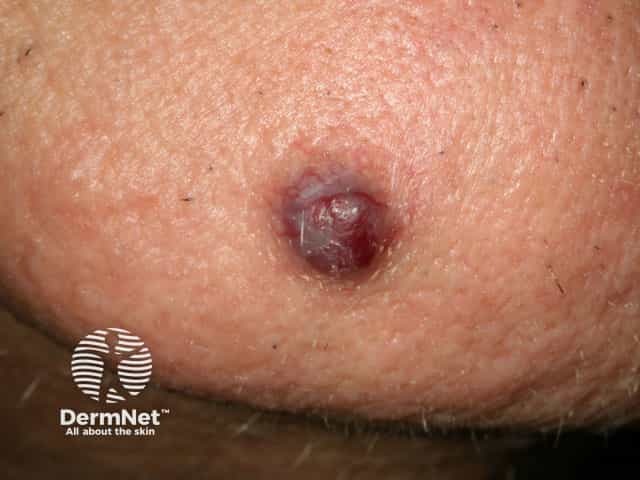
Cherry angioma
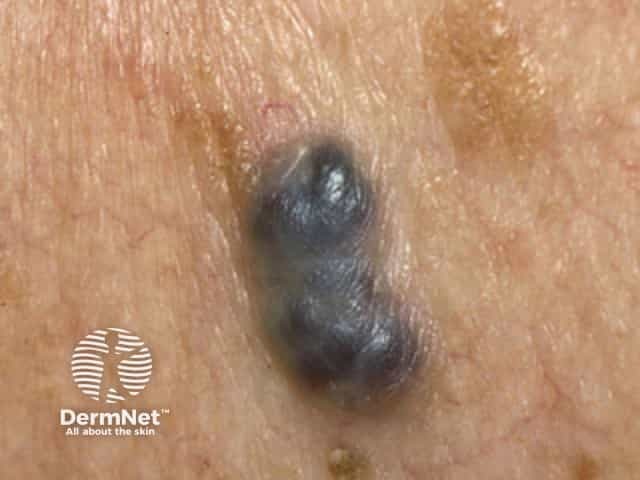
Cherry angioma
See more images of cherry angioma.
Cherry angiomas markedly increase in number from about the age of 40, so it has been estimated that 75% of people over 75 years of age have them. Although they also called senile angiomas, they can occur in young people too - 5% of adolescents have been found to have them. Cherry angiomas are very common in males and females of any age or race, with no difference in sexes or races affected. They are however more noticeable in white skin than in skin of colour. There may be a family history of similar lesions. Eruptive cherry angiomas have been rarely reported to be associated with internal malignancy and pregnancy.
The cause of cherry angiomas is unknown. Genetic analysis has found cherry angiomas frequently carry specific somatic missense mutations in the GNAQ and GNA11 (Q209H) genes, which are also involved in other vascular and melanocytic proliferations.
Cherry angioma is an asymptomatic firm red, blue, or purple papule, 0.1–1 cm in diameter. When thrombosed, it can appear black in colour until examined with a dermatoscope when the red or purple colour is more easily seen. Cherry angiomas are usually multiple. They are usually scattered over any part of the body surface, but are rarely found on the hands and feet or mucous membranes.
Cherry angioma is usually easy to diagnose, but occasionally it may be confused with:
Spider telangiectasis, also known as spider naevus, is sometimes (incorrectly) called a spider angioma but this is a vascular dilatation and not a proliferation of endothelial cells.
Cherry angioma is usually diagnosed clinically and investigation is not necessary for the majority of lesions. It has a characteristic red-clod or lobular pattern on dermoscopy (called lacunar pattern using conventional pattern analysis).
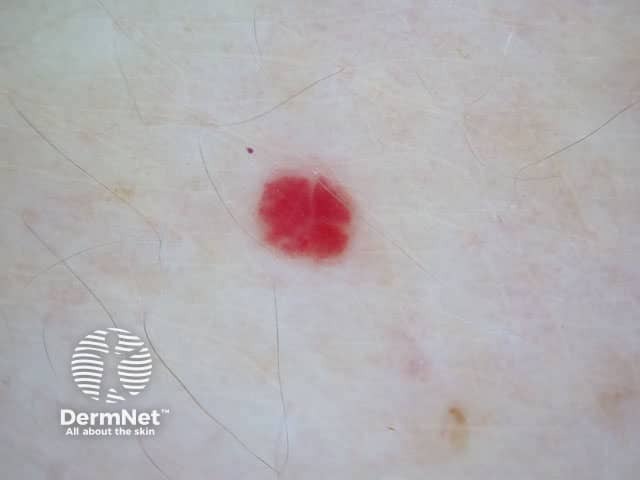
Cherry angioma
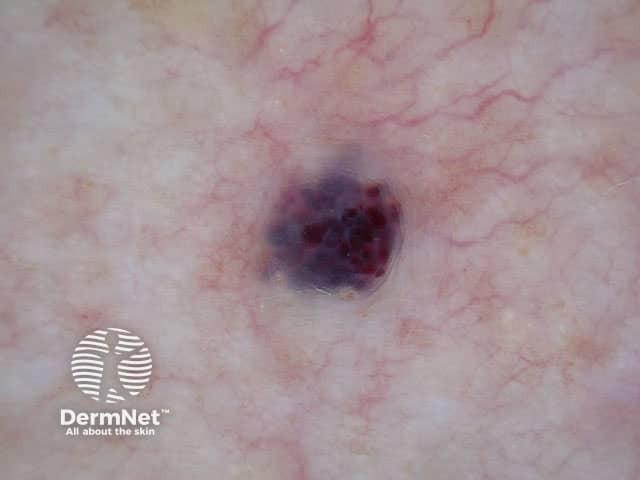
Cherry angioma
When there is uncertainty about the diagnosis, a biopsy may be performed. The angioma is composed of venules in a thickened papillary dermis. Collagen bundles may be prominent between the lobules. See cherry angioma pathology.
Cherry angiomas are harmless, so do not have to be treated. Occasionally, they are removed to exclude a malignant skin lesion such as nodular melanoma.
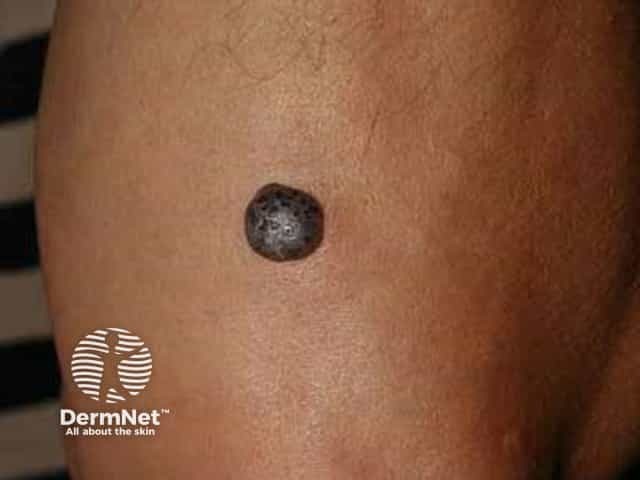
Cherry angioma resembling nodular melanoma
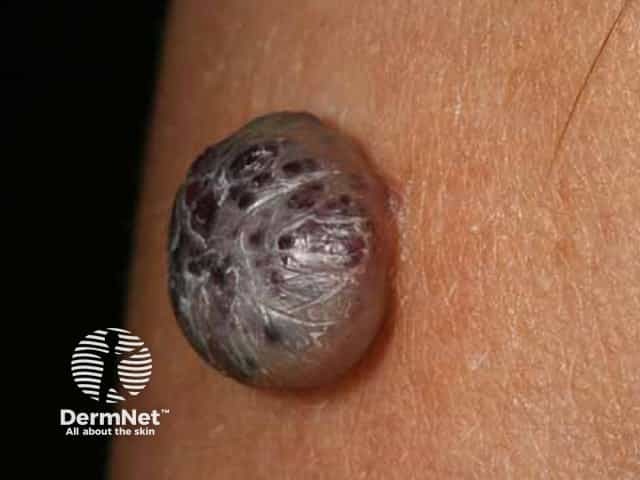
Cherry angioma resembling nodular melanoma
If desired for cosmetic reasons, a cherry angioma can be simply removed by one of the following methods: