Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Chin-Yun Lin, Dermatology Registrar; Dr Amanda Oakley, Dermatologist, Waikato Hospital, Hamilton, New Zealand, 2011.
Introduction
Terminology used in electrosurgery
Waveforms in electrosurgery
Electrofulguration and electrodessiccation
Electrocoagulation
Electrosection
Thermocautery
Risks of electrosurgery
Electrosurgery is used in dermatological procedures to stop bleeding (haemostasis) or to destroy abnormal skin growths.
In electrosurgery, high-frequency, alternating electric current at various voltages (200 to 10,000 V) is passed through the skin to generate heat. It requires a power supply and a handpiece with one or more electrodes. The device is controlled using a switch on the handpiece or a foot switch.
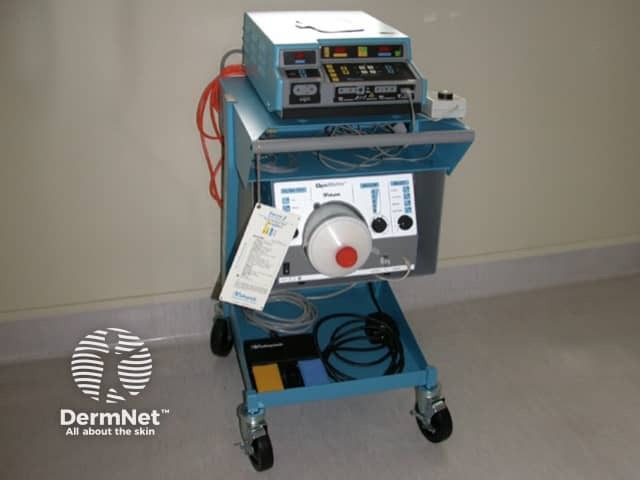
Electrosurgery

Electrocautery

Tips used for electrocautery
Some of the terminology used to describe electrosurgery is confusing. The aim of the procedure is to perform cauterisation. The word cautery originates from the latin, meaning to brand. It relates to the coagulation or destruction of tissue by heat or a caustic substance.
Electrosurgery (particularly electrocoagulation) is sometimes incorrectly called diathermy, which means ‘dielectrical heat’. Diathermy is produced by rotation of molecular dipoles in high frequency alternating electric field – the effect produced by a microwave oven.
The term electrocautery is most often used in reference to a device in which a direct current is used to heat the cautery probe. As no current flows through the patient, this is not a true form of electrosurgery. It is therefore preferable to use the term thermocautery for these devices.
Electrosurgery includes:
Electrosurgery may be monoterminal, monopolar or bipolar.
Different waveforms may be generated by the electrosurgery machine for different procedures.
Electrofulguration and electrodesiccation are used to destroy superficial lesions that are unlikely to bleed profusely when disturbed, such as viral warts and seborrhoeic keratoses.
Electrofulguration and electrodesiccation use a single electrode to produce high voltage and low amperage current. The current accumulates in the patient but there is minimal tissue damage.
Unless bipolar output is used, the patient must be on an insulated table, as burns may result from current passing between patient and the earth-ground. Electrofulguration and electrodesiccation should only be performed on conscious patients who would feel the burn from an unwanted earth-ground path.
The Conmed Hyfrecator® is a brand name for a low-powered electrosurgical device used for electrofulguration, electrodessication and electrocoagulation. The term ‘hyfrecation’ is often used generically to describe similar devices made by other manufacturers. The power output is adjustable, and the pencil handpiece may be equipped with different stainless steel tips, including the following types.
Electrocoagulation is used to cause deeper tissue destruction and to stop bleeding with minimal carbonisation. The haemostatic and destructive capacity of electrocoagulation makes it ideal for the treatment of skin cancers and vascular skin conditions such as pyogenic granuloma. It can also be used to stop small blood vessels from bleeding during skin surgery.
Electrocoagulation uses monopolar or bipolar electrodes to produce low voltage and high-amperage current at relatively low power. An indifferent electrode prevents accumulation of current in the patient, hence low voltage is sufficient to establish current flow. High amperage causes deep tissue destruction and haemostasis by fusion of blood vessel collagen and elastic fibres.
The electrode is applied across the lesion until slightly pink to pale coagulation occurs. Coagulated tissue has greater resistance to electrical current than normal skin, and limits the amount of damage.
Electrocoagulation may result in permanent scarring and white marks (hypopigmentation).
Electrosection is used to simultaneously cut skin and seal bleeding vessels by blending damped and undamped wavetrains. It is suited for excision of large, relatively vascular lesions, such as benign dermal naevi (moles), skin tags, or for shaving off seborrhoeic keratoses, folliculitis keloidalis nuchae and rhinophyma (see rosacea). Electrosection requires almost no manual pressure from the operator as the electrode glides through tissue with minimal resistance.
Electrosection uses an monopolar electrode to produce low-voltage and high-amperage current at higher power than is used for electrocoagulation. The current is highly focused to vaporise tissue with minimal peripheral heat damage. The electrode is usually a fine tungsten wire or loop.
The destruction of chemical bonds or decomposition of tissue arises through thermolysis (heat-induced) and electrolysis (via DC electric-current). The main component of tissue is water, which is broken down into its components, hydrogen and oxygen.
Radiofrequency devices are often used for electrosection, e.g. Ellman Surgitron®. They produce little heat so cause little collateral tissue damage.
An assortment of single use or disposable electrodes are available for the Surgitron.
Thermocautery is used for pinpoint haemostasis during surgical procedures or to get rid of small blood vessels (telangiectasias).
Direct electric current is used to heat the surgical element, which then causes thermal injury by direct heat transference to the tissue. In contrast, in electrosurgery, the treating electrode remains cold.
Portable and disposable thermocautery devices are available powered by penlight batteries. The Shaw Hemostatix® Scalpel is a form of thermocautery in which a heated disposable copper alloy blade is used to cut tissue with reduced bleeding in highly vascular areas.
Thermocautery is suitable for patients with an implanted pacemaker or defibrillator.
The risks of electrosurgery include electric shock and electrical burns, thermal burns, transmission of infection and production of toxic gases.
Electric shock can be minimised by:
Electric/thermal burns can be minimised by:
Electrosurgery may be used to treat viral warts. Thermolysis will generate smoke/fumes which may contain human papillomavirus (HPV) particles that may be transmitted to the operator who breaths in or comes into contact with the fume. When working with HPV-related lesions, minimise the risk of transmission.
Other viral DNA, bacteria, carcinogens, and irritants are also known to be present in electrosurgical smoke. NIOSH (the National Institute of Occupational Safety and Health) a division of CDC (Center for Disease Control, USA) have also studied electrosurgical smoke at length. They state: “Research studies have confirmed that this smoke plume can contain toxic gases and vapors such as benzene, hydrogen cyanide, and formaldehyde, bioaerosols, dead and live cellular material (including blood fragments), and viruses.”
Smoke can be removed using hand held suction. Newer smoke evacuation devices can be attached directly to a standard electrosurgical pencil reducing the work of an assistant during surgery.
Electric currents from electrosurgery electrodes pass through the patient's body to the indifferent electrode. This may sometimes cause malfunction of implanted cardiac devices.
This risk may be mitigated in the following ways.
Pre and postoperative input from a cardiologist may be required in complex patients.