Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Blood vessel problems Diagnosis and testing
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated 2012. Revised and updated Dr Arun Gangakhedkar, Paediatrician, Waitemata DHB, Auckland, New Zealand. Copy edited by Gus Mitchell. January 2021.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses
Infantile haemangioma, also known as a strawberry naevus, is the most common benign vascular skin tumour in children. It is noticed in the first few weeks of life.
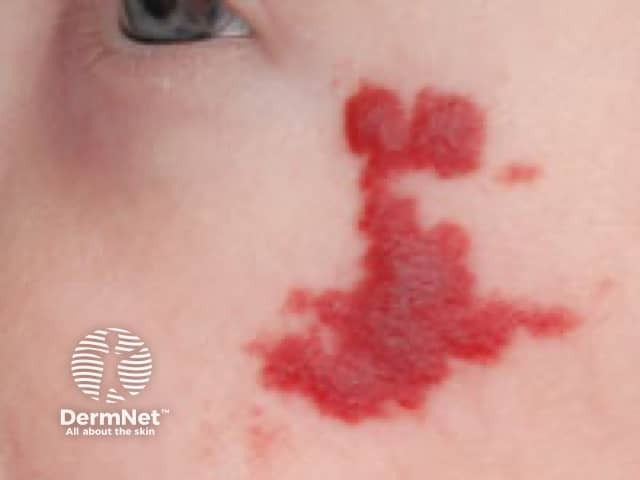
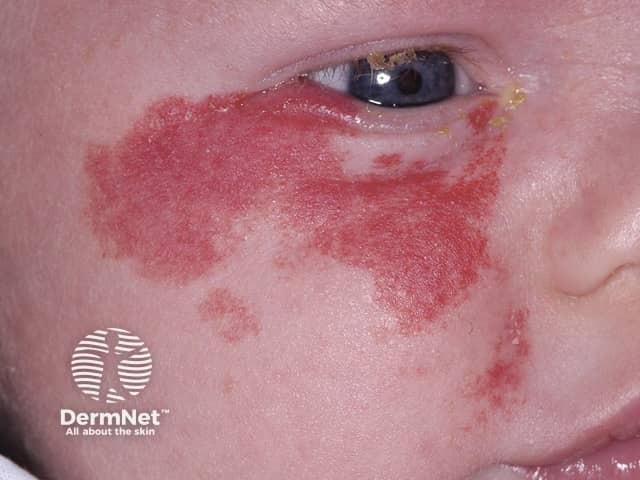
Infantile haemangioma, face
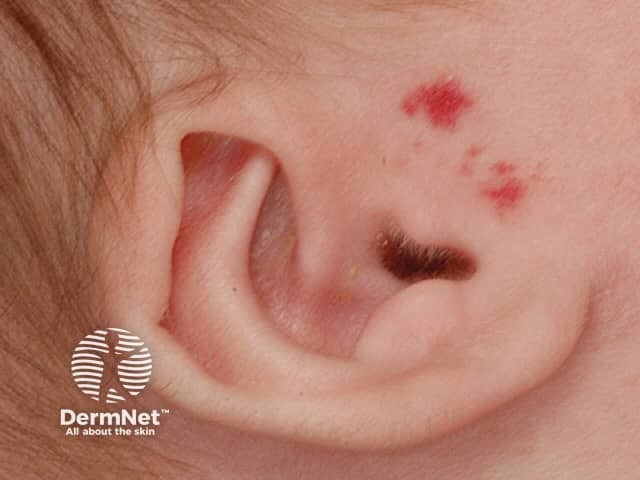
Infantile haemangioma
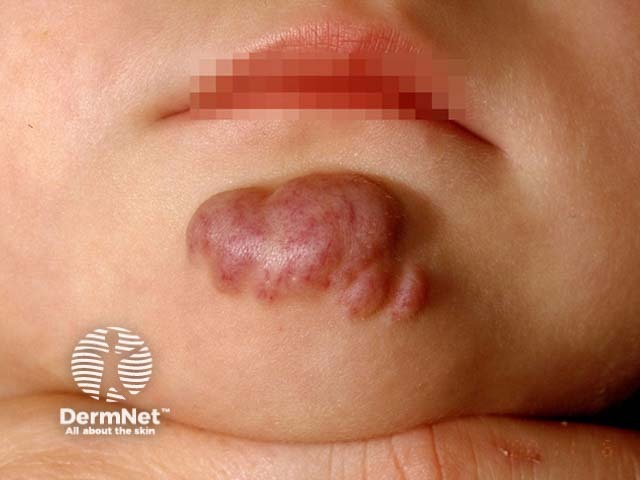
Infantile haemangioma is found in 1–2% of newborns, and up to 10–12% at 1 year of age in Caucasian infants. It is less frequent in non-Caucasian populations. Girls are more commonly affected than boys (3:1).
Risk factors for developing infantile haemangioma include:
A placental origin for infantile haemangioma is suggested due to GLUT1 protein expression. Fetal vascular origins are proposed due to the presence of primitive marker CD133 from the fetal cardinal vein.
Defective vascular stem cell regulation involving endothelial progenitor cells (EPC), or extrinsic factors such as hypoxia and developmental vascular field disturbances can influence the development of vascular anomalies.
Infantile haemangiomas are typically solitary and most are located on the head and neck region (60%). Involvement of internal organs is usually indicated by multiple cutaneous lesions. The clinical features are determined by the depth of the lesion, distribution pattern, and phase of growth.
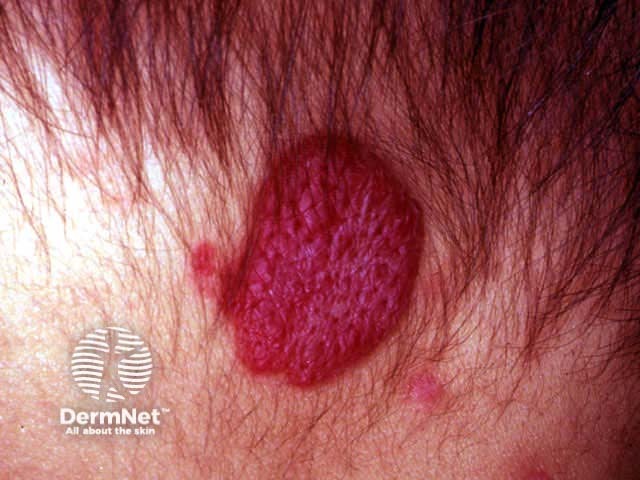
Superficial infantile haemangioma
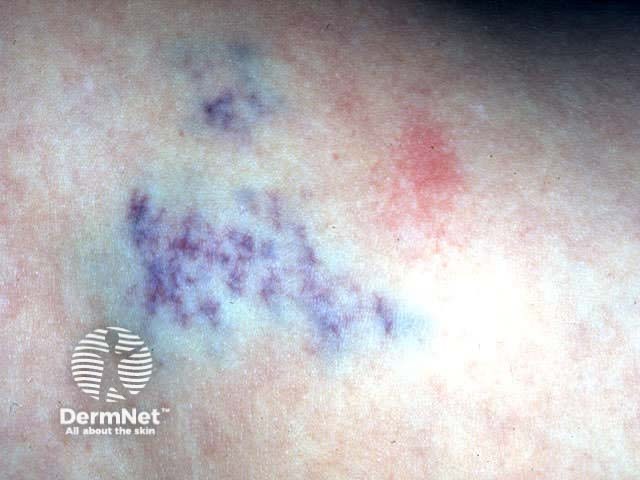
Deep infantile haemangioma
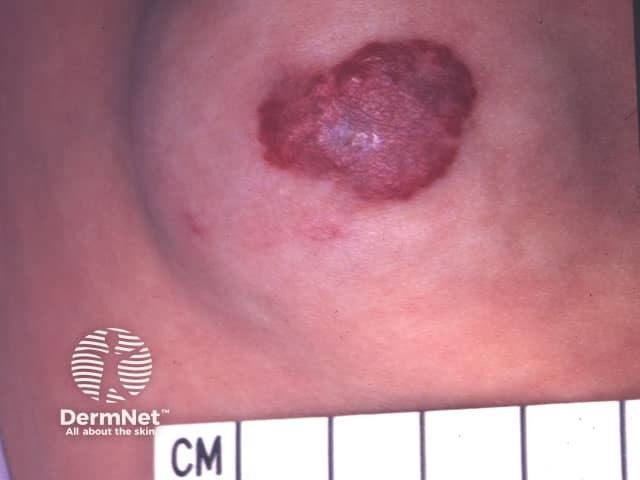
Mixed infantile haemangioma
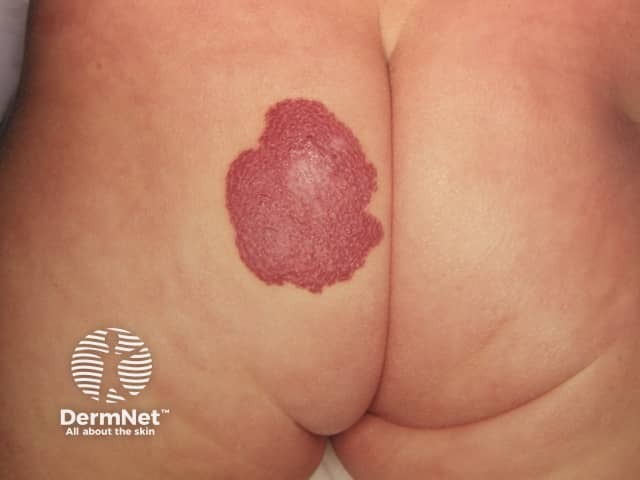
Focal infantile haemangioma
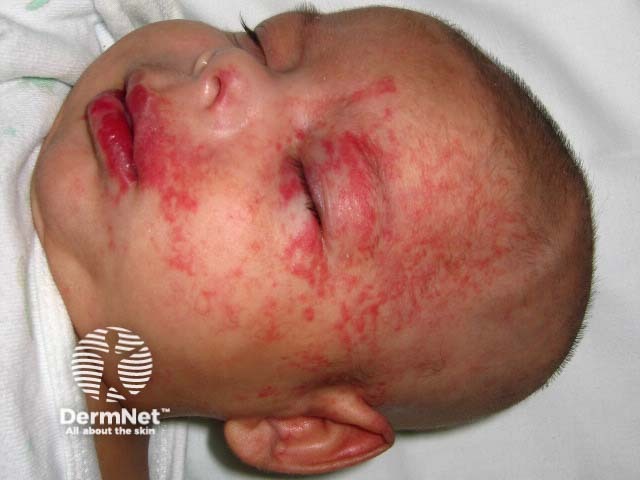
Segmental infantile haemangioma
Most infantile haemangiomas show rapid growth in the first 3 months with a growth arrest by about 5 months of age, receding subsequently over several years. The progression may be described in different morphological phases.
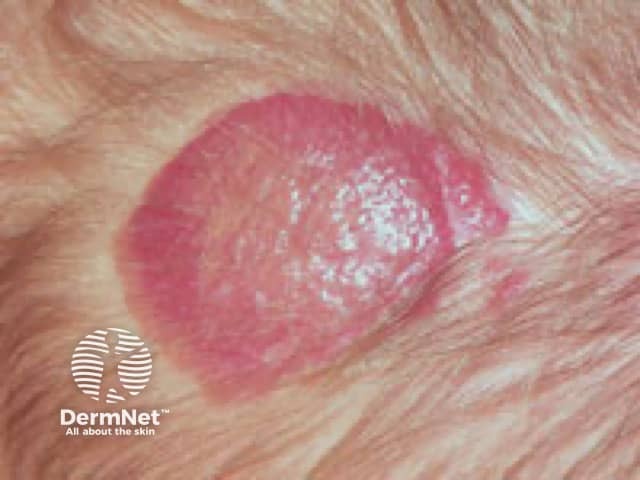
Superficial infantile haemangioma on the scalp
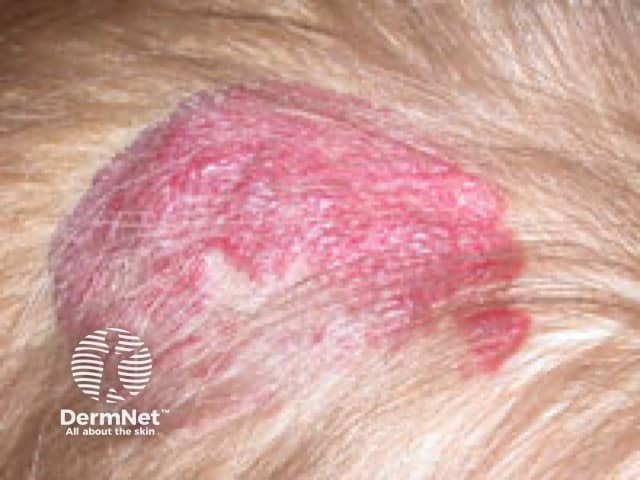
Superficial infantile haemangioma starting to regress
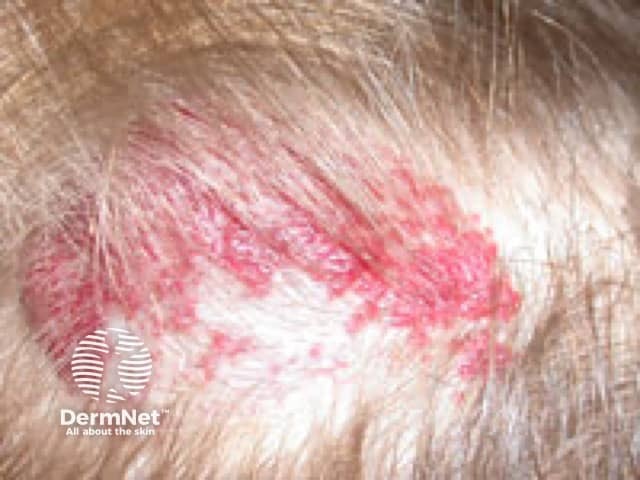
Superficial infantile haemangioma, further regression
Infantile haemangioma with minimal or arrested growth (IH-MAG) has an abortive or minimal growth in 25% of the lesion’s surface area, appearing as telangiectatic patches with or without papules, lacking a significant proliferative phase. This may be mistaken for a port-wine stain [see Capillary vascular malformation]. Occasionally these can be segmental with syndromic associations. Two-thirds of these lesions are seen over lower limbs.
Infantile haemangioma is usually a clinical diagnosis and investigations are not routinely indicated. Investigations may be considered if the diagnosis is uncertain, to define extent and associations, or monitor response to therapy.
Tests may include:

Kaposi sarcoma
Vascular malformation
Angiosarcoma
[see also Infantile haemangioma: Complications and treatment]