Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Jane Morgan, sexual health physician, Waikato Hospital, Hamilton, New Zealand, 2003. Editor-in-Chief: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Updated by Jannet Gomez; Dr Amanda Oakley, February 2017. Copy editor: Gus Mitchell. Minor update November 2025.
Kaposi sarcoma (KS) is a disease of the endothelial cells of blood vessels and the lymphatic system. Despite its name, it is no longer classified as a sarcoma (which is a malignant tumour of mesenchymal origin) as it is due to multicentric vascular hyperplasia.
There are four types of Kaposi sarcoma.
In the United States, Kaposi sarcoma was particularly common in the 1980s. It remains prevalent amongst HIV-positive men who have had sex with men (MSM), in which it has a very aggressive course. It occurs less frequently in intravenous drug users and is rare in women, haemophiliacs, or their sexual partners. HIV–associated Kaposi sarcoma is more common in women than in men in some parts of Africa. It has become less common in the US and Europe because of effective highly active antiretroviral treatment (HAART) for HIV.
Iatrogenic Kaposi sarcoma is a particular concern for organ transplant patients, especially in geographic areas associated with high levels of infection with Kaposi sarcoma herpesvirus (KSHV). Most have the virus before transplantation, but the drugs cause it to reactivate. Use of corticosteroids and biologics like rituximab, infliximab, and abatacept, prescribed for chronic inflammatory and autoimmune conditions, are also prone to develop Kaposi sarcoma.
Kaposi sarcoma has several causes.
KSHV may lie dormant, or replicate and cause disease. KSHV may also cause some forms of non-Hodgkin lymphoma and Castleman disease.
Kaposi sarcoma presents as red to purplish macules, papules and nodules anywhere on the skin or mucous membranes lining the mouth, nose, and throat; lymph nodes; or other organs. Initially, the lesions are small and painless, but they can ulcerate and become painful.
There are various forms:
Kaposi sarcoma often starts as flat patches on one or both lower legs, often in association with lymphoedema. The patches evolve into plaques, nodules or scaly tumours.
Kaposi sarcoma in association with HIV infection may develop at any time during the illness. Generally, the greater the immunosuppression (eg, with CD4 cell counts less than 200/mm3), the more extensive and aggressive the Kaposi sarcoma will be.
Kaposi sarcoma lesions can also occur internally; in the gut, lungs, genitals, lymphatic system and elsewhere. These internal lesions may cause symptoms such as:
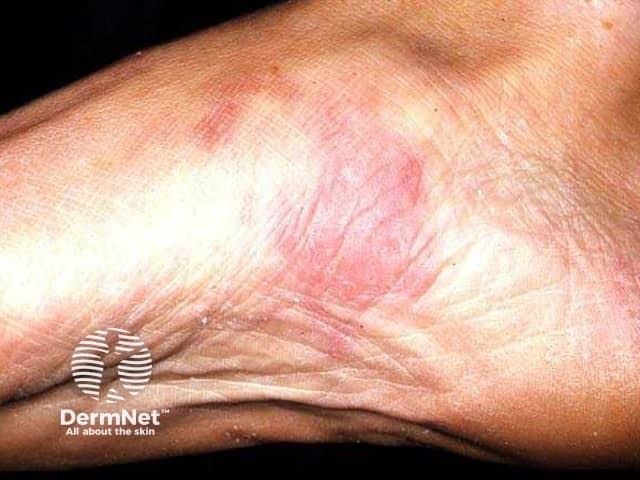
Patch stage KS
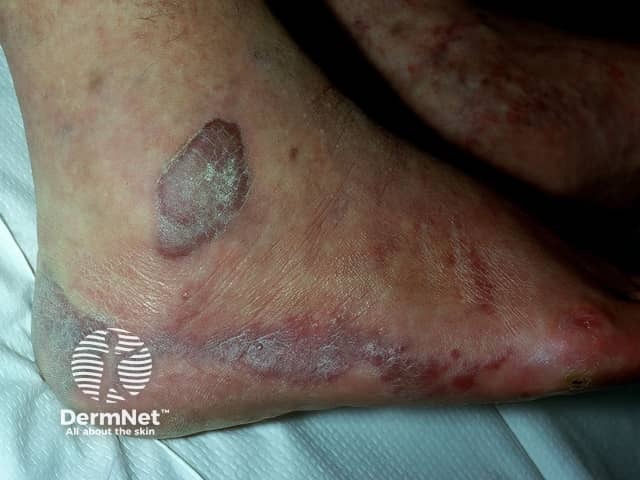
Plaque stage KS
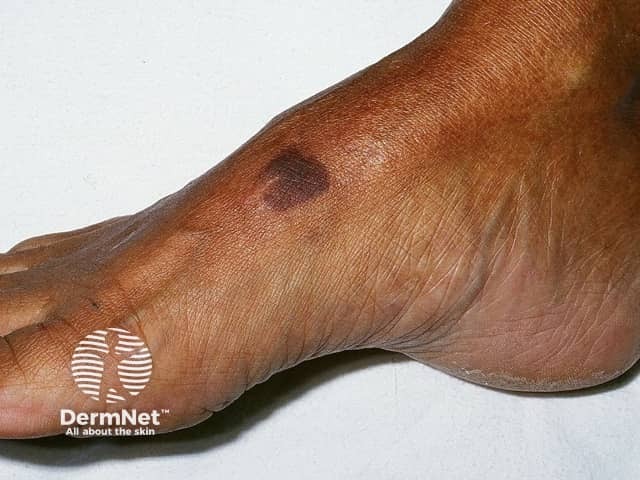
Classic KS
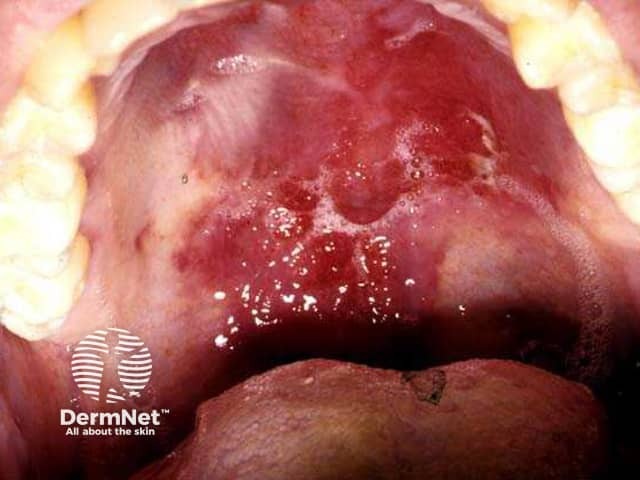
Palatal KS
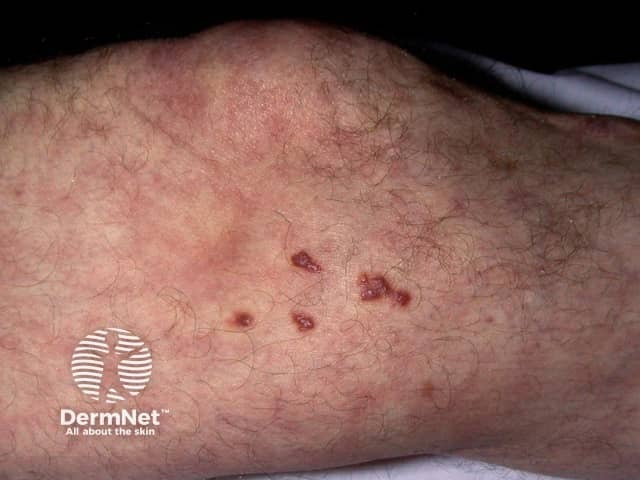
Plaque stage KS
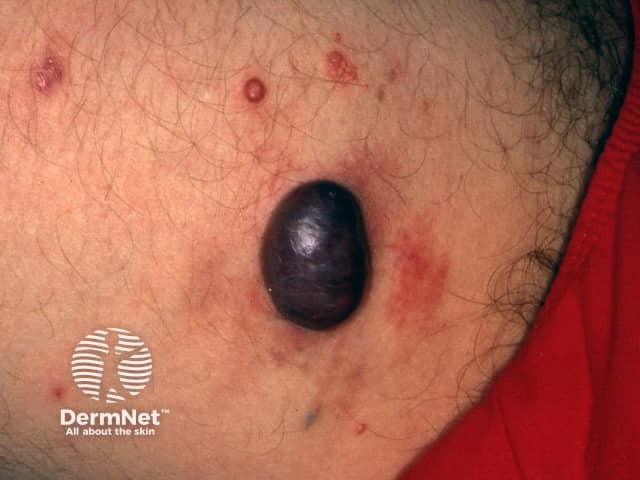
Tumour stage KS
See more images of Kaposi sarcoma.
Blood tests may show no abnormality, depending on whether there are associated disorders such as AIDS. Anaemia may arise if there is bleeding. KSHV assays or antibody titres to KSHV are challenging to interpret. CD4 lymphocyte counts and plasma HIV load studies are performed in patients with HIV infection.
The appearance of Kaposi sarcoma lesions is often typical, but a skin biopsy of a lesion allows a definite diagnosis, as other conditions such as melanoma, fungal infections, and mycetoma mimic Kaposi sarcoma in appearance and location. The histopathology of Kaposi sarcoma shows red cells in slit-like spaces formed by atypical spindle cell proliferation of endothelial cells and associated with inflammatory cells.
There have been various attempts to classify Kaposi sarcoma, depending on whether it is localised or disseminated in the skin, and if there is a lymph node or internal organ involvement. The degree of immunosuppression present may also be used in staging systems.
Kaposi sarcoma has a variable course. Some patients develop only a few minor skin lesions while others have extensive external and internal disease. The latter lesions may result in fatal complications from bleeding, obstruction or perforation of an organ. Kaposi sarcoma is not curable, but it can be treated and its symptoms controlled.
In HIV disease, if the lesions are not widespread or troublesome, often the best approach is to treat the underlying HIV infection with highly active antiretroviral drug combinations that suppress HIV replication (HAART).
Iatrogenic Kaposi sarcoma may improve or clear if it is possible to stop the immune suppressive medication.
The choice of a more specific treatment depends mainly on the extent of the disease.
Small, localised lesions are generally only treated if they are painful or they are causing cosmetic problems. It should be noted that lesions tend to recur after local treatments. Treatments include:
A combination of anti-cancer drugs are given, but at lower than usual dosages if there is immunosuppression.
Other chemotherapy treatments that are used in some international centres include bleomycin, etoposide, paclitaxel, docetaxel and liposomal forms of the conventional anti-cancer drugs, doxorubicin or daunorubicin. Liposomal means that the drugs are coated in small fat bubbles, or liposomes, which allows better absorption, resulting in less cardiac toxicity and myelotoxicity. Paclitaxel is approved for use in Kaposi sarcoma in advanced stages or as a second-line option.
Immunotherapy includes the use of interferon-alpha and imiquimod, sirolimus and thalidomide.
Kaposi sarcoma may arise in organ transplant patients. Switching from ciclosporin to sirolimus (rapamycin) has resulted in resolution of the sarcoma. This is primarily attributed to the anti-proliferative and anti-angiogenic effects of sirolimus (mTOR inhibitor).
Clinical trials into a wide range of other therapies are ongoing.