Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Introduction - the lymphatic system Demographics Causes Clinical features Complications Diagnosis Treatment
Lymphoedema (American spelling ‘lymphedema’) is a swelling of part or parts of the body that occurs when the lymphatic system is not working properly. Lymphoedema can be localised to a small area, or diffuse over a large area such as one or both upper or lower limbs.
To understand how lymphoedema occurs we need to know a bit about what the lymphatic system is and how it works.
The lymphatic system forms part of the immune system and part of the vascular system.
The lymphatic system is made up of many tiny vessels that run throughout the body and gradually join together to form bigger vessels. In the skin, small lymphatic vessels are found in the dermis but not in subcutaneous tissue. Running through these vessels is a clear fluid called lymph. Lymph contains the excess protein, water, bacteria and waste products that the body doesn’t require and travels along the lymphatic system until it reaches the lymph nodes (glands).
The lymph nodes, which are situated in the neck, armpits, groins and deep inside the chest and abdomen, filter and cleanse the lymph to remove any foreign matter (e.g. bacteria) and start any necessary immune reactions. Once passed through the lymph nodes, lymph finally drains into large veins located in the lower neck. Movement of adjacent muscles helps to keep the lymph moving along the lymphatic system. In addition the walls of the lymphatic vessels contract and valves inside the vessels keep things pumping.
Lymphoedema:
Oedema (swelling) occurs when excess fluid and protein from damaged blood vessels (e.g. after a burn or ankle sprain) enters into the lymphatic system at a rate too fast for the lymph to be carried away. This produces a temporary swelling which gradually resolves on its own as the damaged tissue heals, blood vessels no longer leak excessively and the lymphatic system can keep pace with the normal flow of lymph.
Lymphoedema is the name given to the swelling that occurs because of a damaged or blocked lymphatic system. Protein, water and waste products are released into tissue in the normal way but a damaged lymphatic system prevents the drainage away and swelling of the affected area results (lymphostasis). In addition, the limb may become inflamed.
Examples of localised or circumscribed lymphoedema include:
There are basically two types of diffuse lymphoedema based on the underlying causes.
Initially the symptoms and signs of lymphoedema may be very slight and almost unnoticeable. If left untreated, the swelling may get bigger and eventually become permanent. Some or all of the following symptoms may be experienced in diffuse lymphoedema.
At first the swollen area will pit if pressed with a thumb. However, as it becomes bigger and harder it will no longer pit. If lymphoedema is left untreated and the swelling gets worse, skin changes may occur. The skin may get very thick with folds and bulges and cannot be lifted up or pinched. Dry warty spots appear on the ankles, feet and toes (elephantiasis nostras verruciformis, or lymphatic papillomatosis).
Lymphoedema of the legs is often worse than that of the arms as lymphatic drainage from the legs is more difficult. Walking becomes difficult as the patient carries the excess weight.
Complications are common in severe diffuse lymphoedema.
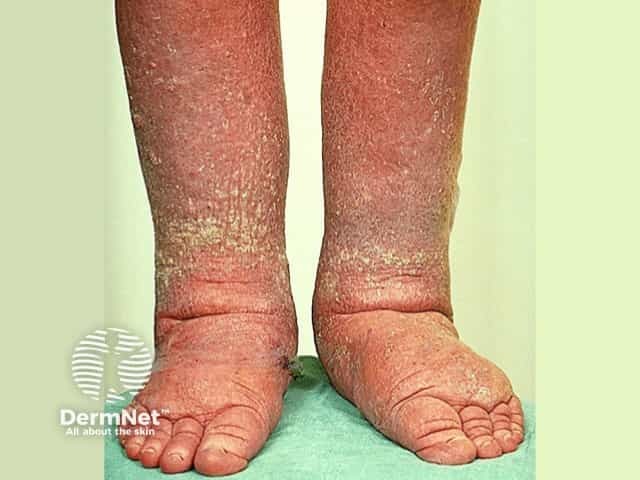
Elephantiasis nostras verruciformis
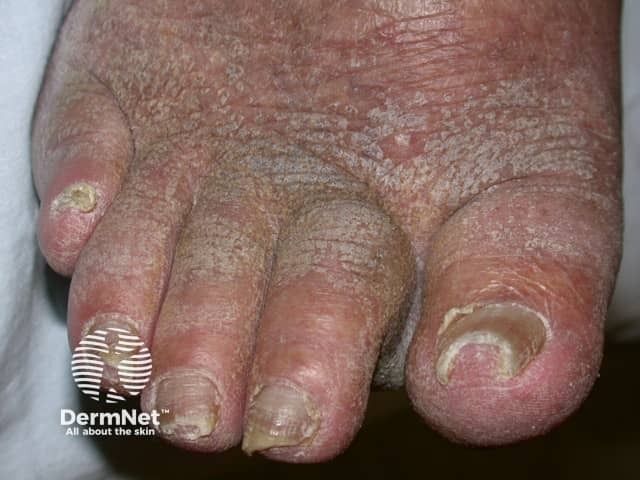
Lymphoedematous toes with overlying warty changes - Kaposi-Stemmer sign was positive (ENV-patient3)
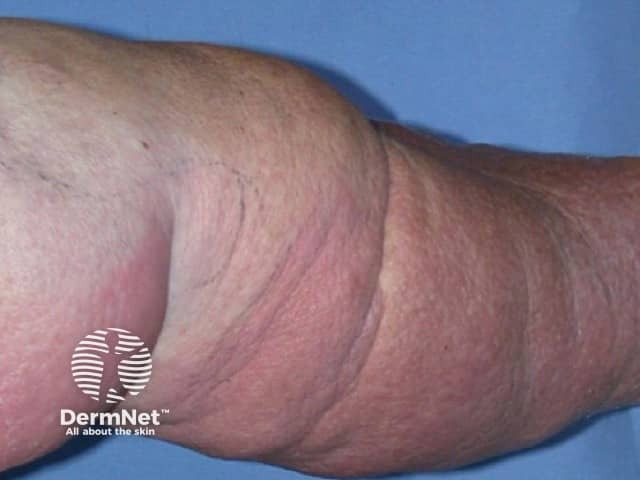
Cellulitis
Diagnosis of lymphoedema is made from a patient's history and observation. The possibility of cancer should be investigated if a cause cannot be found for swelling. In some difficult cases a radiographic test called lymphoscintigraphy may be performed. This measures lymphatic function and gives a fair image of the lymphatic system.
Lymphoedema should be distinguished from lipoedema, in which swelling of both thighs and lower legs is due to the accumulation of fat under the skin.
Lymphoedema is an ongoing condition that has no known cure. The main goal of treatment is to reduce the swelling and keep it to a minimum. It is very important to treat lymphoedema in its early stages to prevent further swelling and complications such as infection. If a cause is found then the cause needs to be treated, e.g. cancer.
For patients with mild to moderate swelling of their limbs a treatment regimen called Complex Physical (Lymphatic/Lymphoedema) Therapy (C.P.T./C.L.T.) is recommended. This regimen consists of 4 main parts.
For people with more severe swelling, additional treatments are usually recommended. These include: