Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Honorary Associate Professor Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated December 2015.
Introduction
Demographics
Causes
Clinical features
Types
Classification by risk
Staging
Diagnosis
Treatment
Advanced and metastatic treatment
Prevention
Outlook
Cutaneous squamous cell carcinoma (SCC) is a common type of keratinocyte cancer, or non-melanoma skin cancer. It is derived from cells within the epidermis that make keratin — the horny protein that makes up skin, hair and nails.
Cutaneous SCC is an invasive disease, referring to cancer cells that have grown beyond the epidermis. SCC can sometimes metastasise and may prove fatal.
Intraepidermal carcinoma (cutaneous SCC in situ) and mucosal SCC are considered elsewhere.
Risk factors for cutaneous SCC include:
More than 90% of cases of SCC are associated with numerous DNA mutations in multiple somatic genes. Mutations in the p53 tumour suppressor gene are caused by exposure to ultraviolet radiation (UV), especially UVB (known as signature 7). Other signature mutations relate to cigarette smoking, ageing and immune suppression (eg, to drugs such as azathioprine). Mutations in signalling pathways affect the epidermal growth factor receptor, RAS, Fyn, and p16INK4a signalling.
Beta-genus human papillomaviruses (wart virus) are thought to play a role in SCC arising in immune-suppressed populations. β-HPV and HPV subtypes 5, 8, 17, 20, 24, and 38 have also been associated with an increased risk of cutaneous SCC in immunocompetent individuals.
Cutaneous SCCs present as enlarging scaly or crusted lumps. They usually arise within pre-existing actinic keratosis or intraepidermal carcinoma.
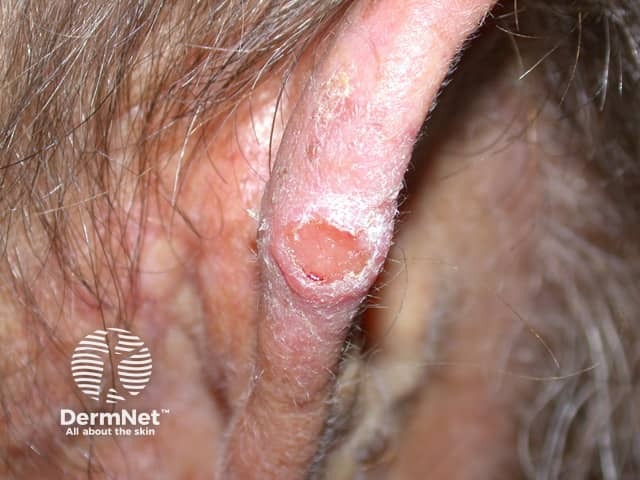
Squamous cell carcinoma
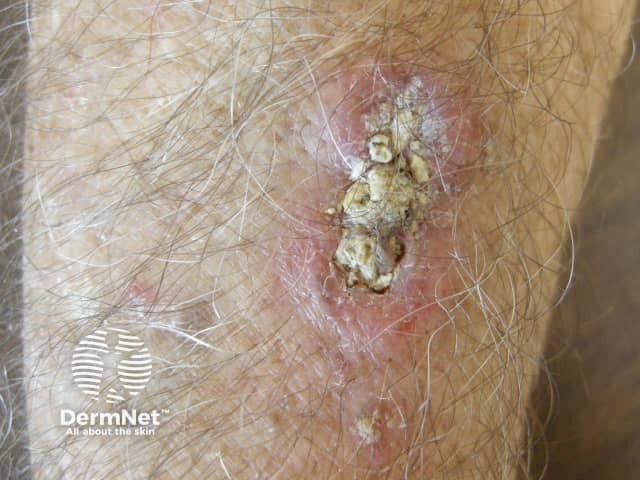
Squamous cell carcinoma
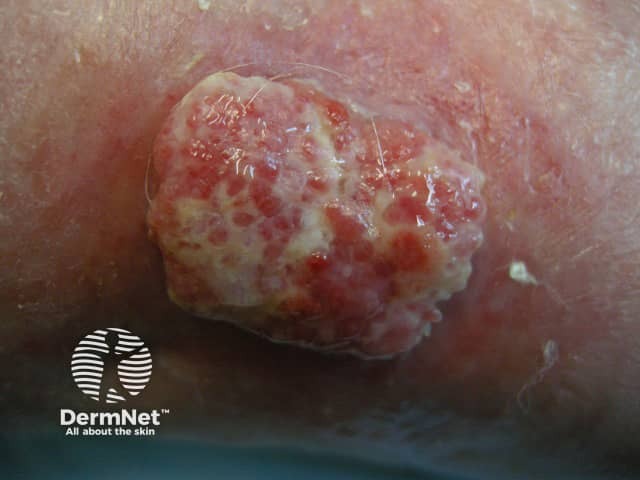
Squamous cell carcinoma
See more images of squamous cell carcinoma:
Cutaneous squamous cell carcinoma images
Distinct clinical types of invasive cutaneous SCC include:
The pathologist may classify a tumour as well differentiated, moderately well differentiated, poorly differentiated or anaplastic cutaneous SCC. There are other variants.
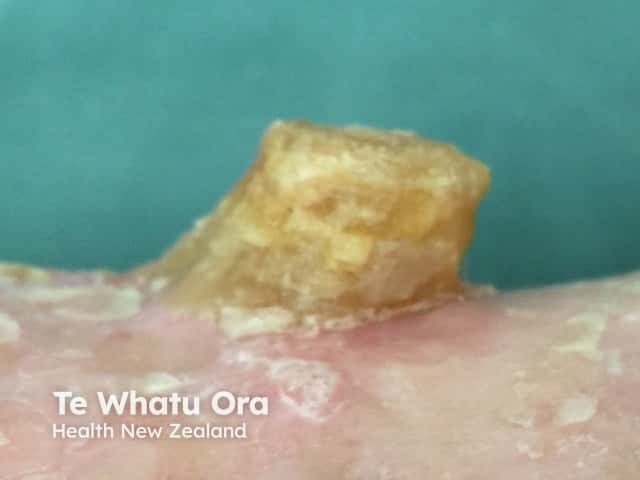
Cutaneous horn
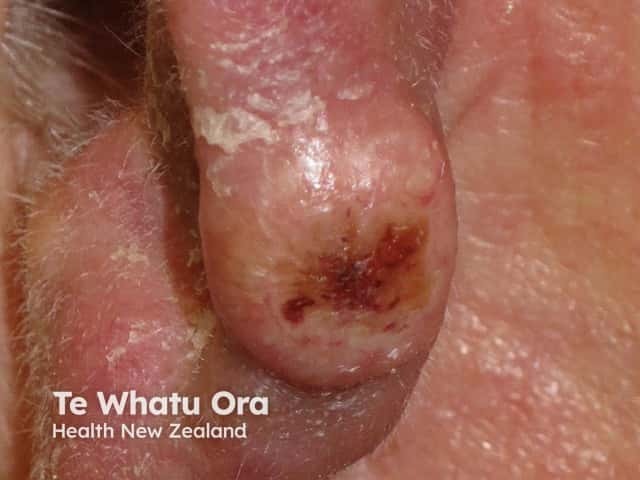
Keratoacanthoma
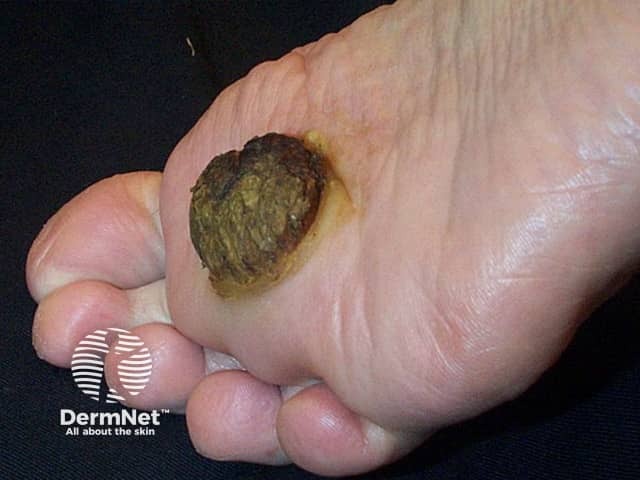
Carcinoma cuniculatum
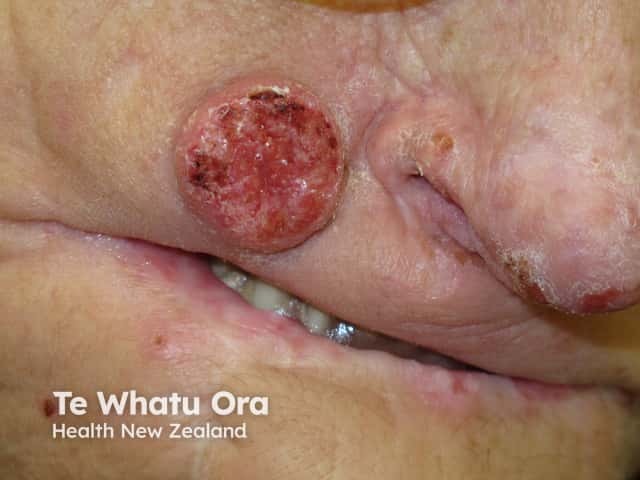
Squamous epithelioma of Ferguson-Smith
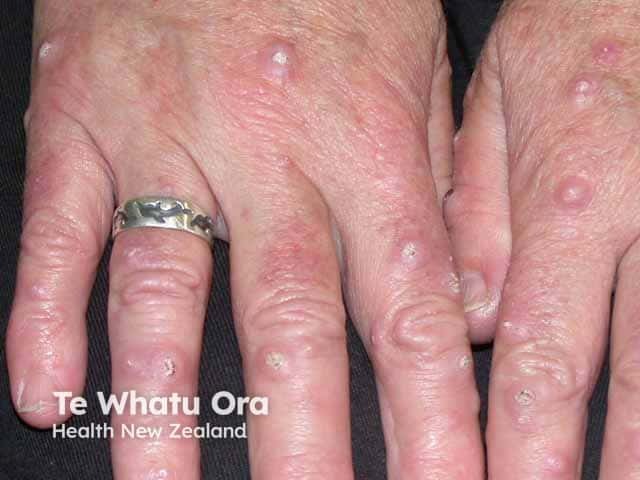
Grzybowski syndrome (GEKA-patient1)
Cutaneous SCC is classified as low-risk or high-risk, depending on the chance of tumour recurrence and metastasis. Characteristics of high-risk SCC include:
High-risk cutaneous squamous cell carcinoma has the following characteristics:
Metastatic SCC is found in regional lymph nodes (80%), lungs, liver, brain, bones and skin.
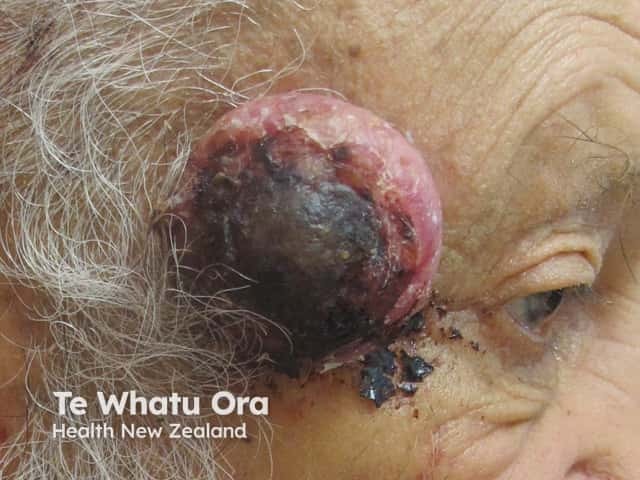
High-risk cutaneous squamous cell carcinoma
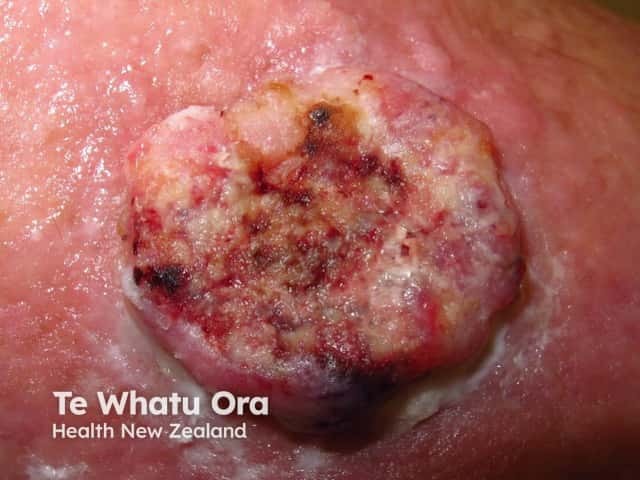
High-risk cutaneous squamous cell carcinoma
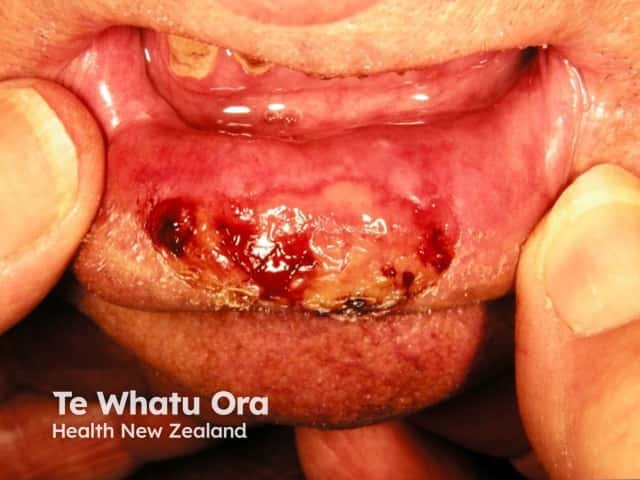
High-risk cutaneous squamous cell carcinoma
In 2011, the American Joint Committee on Cancer (AJCC) published a new staging systemic for cutaneous SCC for the 7th Edition of the AJCC manual. This evaluates the dimensions of the original primary tumour (T) and its metastases to lymph nodes (N).
TX: Th Primary tumour cannot be assessed
T0: No evidence of a primary tumour
Tis: Carcinoma in situ
T1: Tumour ≤ 2cm without high-risk features
T2: Tumour ≥ 2cm; or; Tumour ≤ 2 cm with high-risk features
T3: Tumour with the invasion of maxilla, mandible, orbit or temporal bone
T4: Tumour with the invasion of axial or appendicular skeleton or perineural invasion of skull base
NX: Regional lymph nodes cannot be assessed
N0: No regional lymph node metastasis
N1: Metastasis in one local lymph node ≤ 3cm
N2: Metastasis in one local lymph node ≥ 3cm; or; Metastasis in >1 local lymph node ≤ 6cm
N3: Metastasis in lymph node ≥ 6cm
Diagnosis of cutaneous SCC is based on clinical features. The diagnosis and histological subtype are confirmed pathologically by diagnostic biopsy or following excision. See squamous cell carcinoma – pathology.
Patients with high-risk SCC may also undergo staging investigations to determine whether it has spread to lymph nodes or elsewhere. These may include:
Cutaneous SCC is nearly always treated surgically. Most cases are excised with a 3–10 mm margin of normal tissue around a visible tumour. A flap or skin graft may be needed to repair the defect.
Other methods of removal include:
Locally advanced primary, recurrent or metastatic SCC requires multidisciplinary consultation. Often a combination of treatments is used.
Many thousands of New Zealanders are treated for cutaneous SCC each year, and more than 100 die from their disease.
There is a great deal of evidence to show that very careful sun protection at any time of life reduces the number of SCCs. This is particularly important in ageing, sun-damaged, fair skin; in patients that are immune suppressed; and in those who already have actinic keratoses or previous SCC.
Oral nicotinamide (vitamin B3) in a dose of 500 mg twice daily may reduce the number and severity of SCCs in people at high risk.
Patients with multiple squamous cell carcinomas may be prescribed an oral retinoid (acitretin or isotretinoin). These reduce the number of tumours but have some nuisance side effects.
Most SCCs are cured by treatment. A cure is most likely if treatment is undertaken when the lesion is small. The risk of recurrence or disease-associated death is greater for tumours that are > 20 mm in diameter and/or > 2 mm in thickness at the time of surgical excision.
About 50% of people at high risk of SCC develop a second one within 5 years of the first. They are also at increased risk of other skin cancers, especially melanoma. Regular self-skin examinations and long-term annual skin checks by an experienced health professional are recommended.