Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Treatments Lesions (cancerous)
Author: Tom Middelburg, MD PhD, dermatologist and Mohs surgeon, Christchurch, New Zealand, May 2017.
Introduction
Comparison to standard excision
How it works
Skin cancers best treated by Mohs surgery
Mohs for other types of skin cancer
Efficacy and cost effectiveness
Mohs micrographic surgery, or Mohs surgery, is a precise surgical technique in which the complete excision of skin cancer is checked by microscopic margin control. It offers the highest cure rates while maximizing preservation of healthy tissue. The principles behind it were developed by Dr Frederic Mohs in the 1930s.
Mohs surgery is recognised as the treatment of choice for high risk basal cell carcinoma and squamous cell carcinoma. The skin cancer is progressively removed in stages. After each stage, the excision margins are microscopically examined for remaining cancer cells and this process is repeated until all cancer has been removed.
Mohs is a form of complete circumferential peripheral and deep margin assessment (CCPDMA).
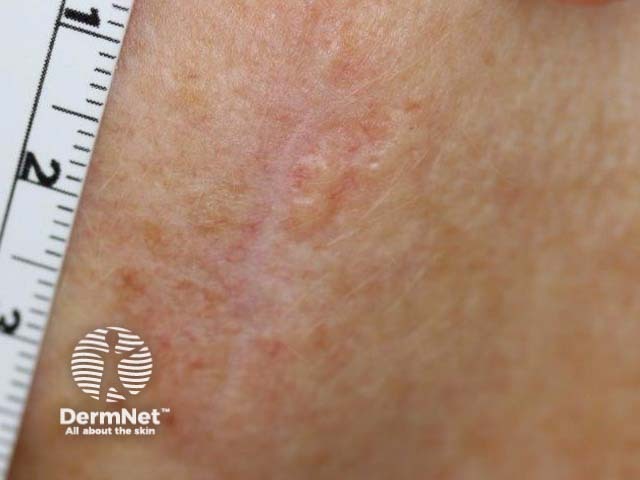
Recurrent basal cell carcinoma

Microscopic slide examination
In standard excision, the tissue sample is sent off for histological processing while the wound is closed. The processing takes a number of days during which cross sections (or vertical sections) are created at various distances through the sample and are microscopically assessed by a pathologist. The pathologist looks for skin cancer at the margins of each section, but these are only a fraction of the actual excision margin.
In Mohs surgery, the histological processing takes place on the day of surgery and the wound is only closed after it has been confirmed that the entire cancer has been removed. The excision margin is examined by an embedding technique that allows horizontal sections to be cut involving all the deep and radial excision margins. If any tumour is visible in these sections, it means that the excision is incomplete and the patient requires a further Mohs stage.
A mapping process and colour coding system is used during Mohs surgery to precisely localise any remaining cancer, and tissue is only removed if it contains cancer. This process preserves healthy tissue.
Mohs surgery yields higher clearance rates than standard excision, and smaller wounds — therefore better cosmetic results.
Mohs surgery is usually undertaken as a single day procedure under local anaesthesia. It involves the following steps:
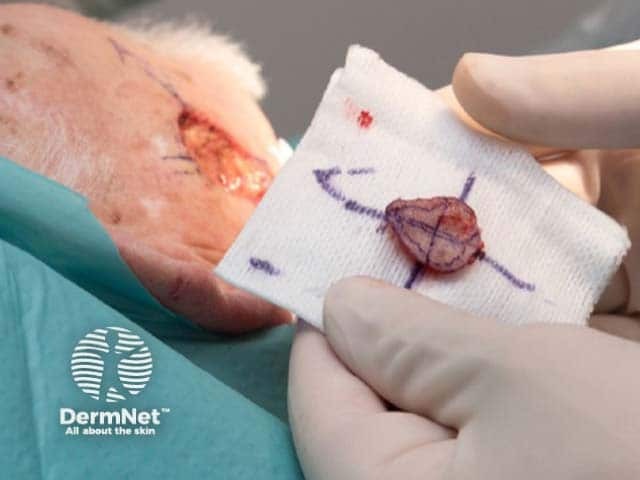
Excision of visible tumour while maintaining orientation
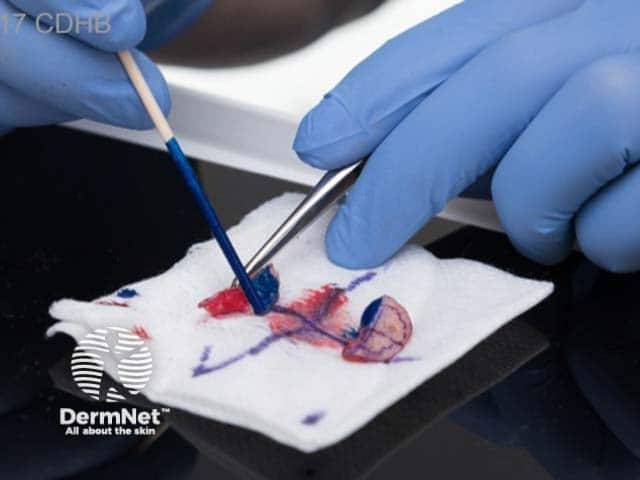
Colour coding the specimens

Cutting frozen sections in cryostat

Staining sections with haematoxylin and eosin

Mohs sections ready for examination
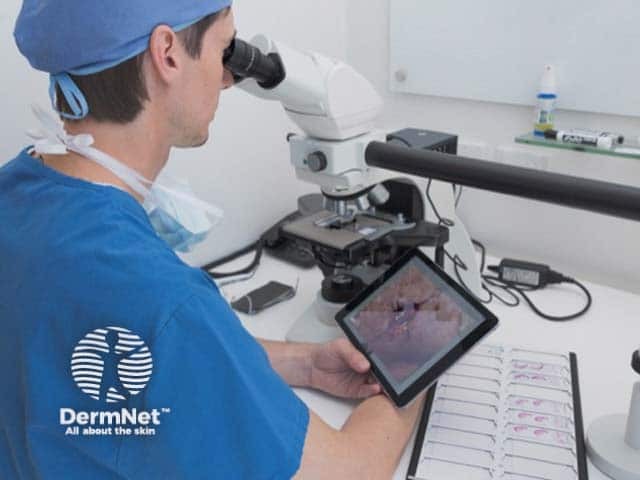
Microscopic examination and marking remaining cancer on image
See clinical images of Mohs surgery ...
Mohs surgery is widely accepted as treatment of first choice for high risk basal cell carcinoma and squamous cell carcinoma. Although different criteria are used across the globe, the main reason to perform Mohs is to minimise the risk of incomplete excision. This reduces burden to the patient and may avoid large and costly re-excisions later.
Mohs surgery has greatest benefit for a tumour at high risk of incomplete excision, such as a:
Mohs may also be appropriate when a large reconstruction is needed to close the defect or when the tumour is located in a cosmetically sensitive area.
In 2012, a joint effort by various medical organisations in the USA led to the development of appropriate use criteria for Mohs surgery. These criteria may be used as guidance when considering Mohs surgery although they may not apply in all jurisdictions [1].
There is plenty of evidence that Mohs is the best form of surgery for high risk basal cell carcinoma and squamous cell carcinoma. Large trials comparing Mohs to standard excision for other types of skin cancer are lacking.
In Mohs surgery, tumour cells must be accurately identified on microscopic examination of frozen sections. This can be challenging in some skin cancers, such as:
For these tumours, variations of Mohs surgery may be applied that follow the basic principles of Mohs surgery (microscopic margin control, horizontal embedding, and mapping and colour coding of tissue) but use paraffin embedded sections instead of frozen sections. This allows the use of immunohistochemical markers to help identify tumour cells.
Such techniques are sometimes collectively referred to as slow Mohs. They include the 'Tuebingen Cake', and 'Muffin' techniques [2].
Mohs surgery leads to fewer tumour recurrences than standard excision of basal cell carcinoma and squamous cell carcinoma. Recurrence rates for Mohs are typically reported to be 1–5%, depending on type of tumour and length of follow-up.
In a randomised clinical trial with 10-year follow-up, recurrence rates were:
Several studies have also found that Mohs is more cost effective than standard excision. The main reason for this is that there are fewer costly operations for recurrent tumours compared to standard excision [4-5].