Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Jenny Caesar, Dermatology Registrar, Singleton Hospital, Swansee, UK. November 2020; Updated: Dr Ian Coulson, Consultant Dermatologist, East Lancashire NHS Trust, UK. Copy edited by Gus Mitchell. August 2021
What is venous insufficiency?
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Venous insufficiency occurs when the normal flow of blood from the superficial veins to the heart via the perforating deep veins in the lower limbs is impaired, resulting in chronic venous congestion. It can be classified as superficial vein insufficiency, perforating, or deep vein insufficiency.
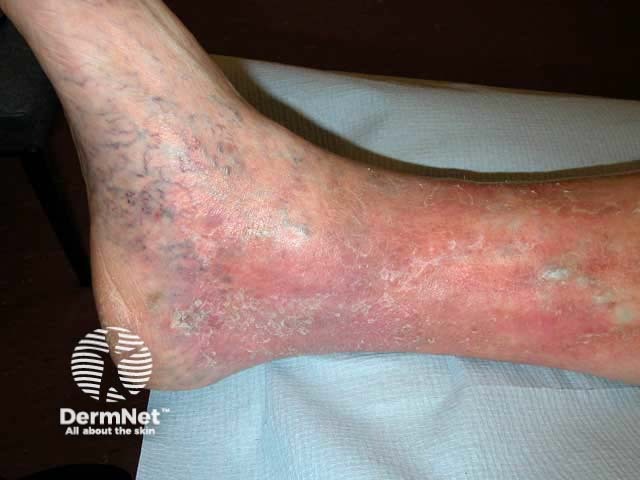
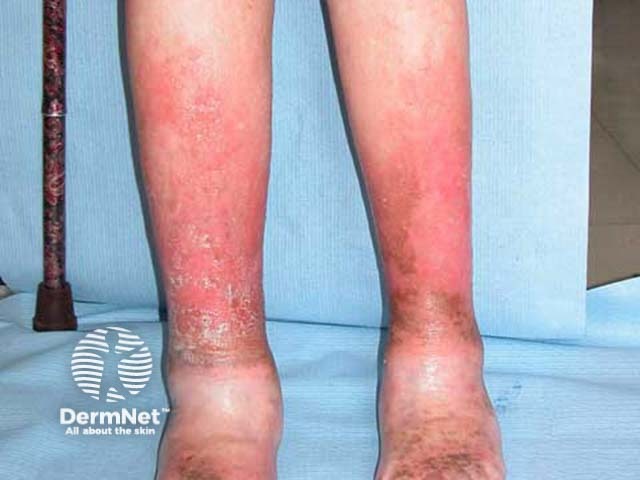
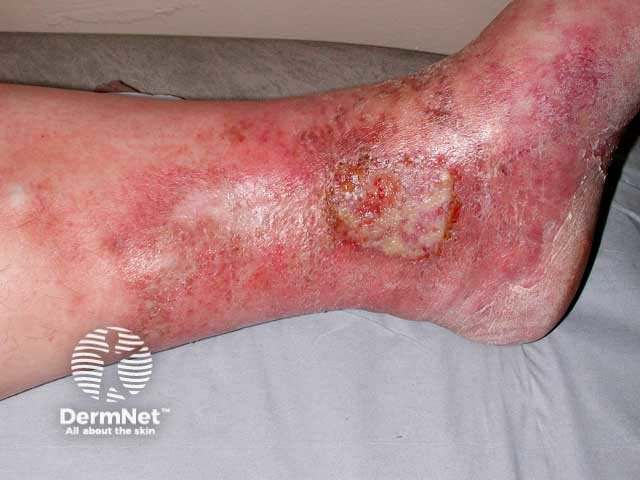
Venous insufficiency is common, affecting all races and both sexes. Estimates suggest rates as high as 50% in some populations. A US study found ethnic whites had a higher rate of venous insufficiency compared to Hispanics, African Americans, and Asians. The Edinburgh Vein Study reported the incidence of chronic venous insufficiency was similar in men and women. Prevalence increases with age, obesity, a family history of varicose veins, and multiple pregnancies.
The venous system in the lower legs consists of a low-pressure superficial network connected by perforating veins to a high-pressure deep network. Venous blood flows from the superficial to deep veins by the action of the calf muscle pump. Retrograde flow is prevented by competent valves.
Chronic venous insufficiency can be caused by:
Once venous hypertension is established, the cutaneous features of chronic venous insufficiency are caused by:
Superficial venous insufficiency can be asymptomatic but may cause aching, cramping, throbbing, burning, or heaviness in the leg. Pain is typical of deep venous insufficiency. Symptoms improve with leg elevation.
Clinical signs of chronic venous insufficiency include:
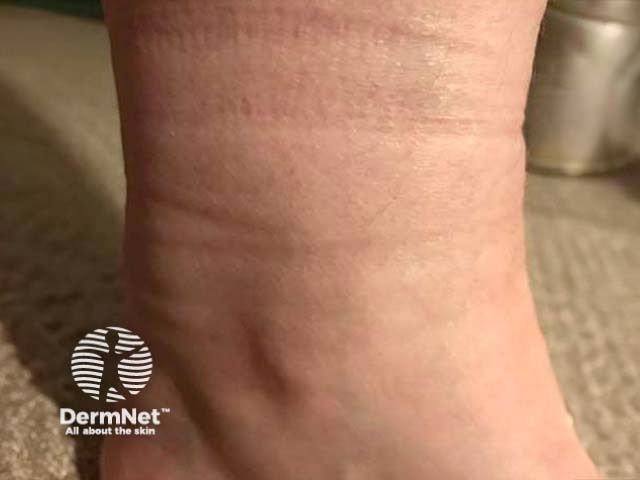
End-of-day ankle oedema
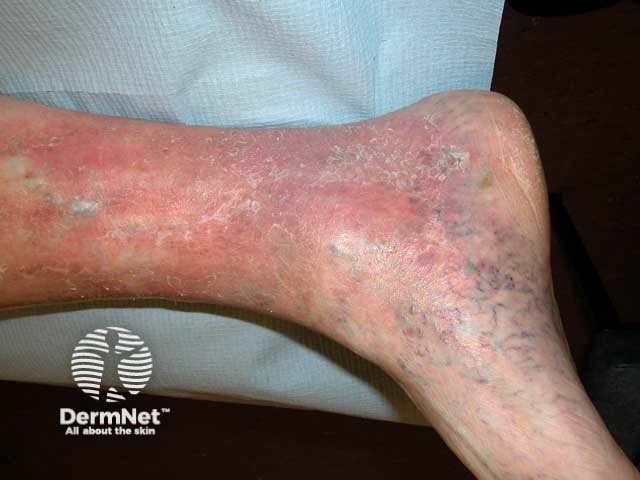
Corona phlebectatica and venous eczema
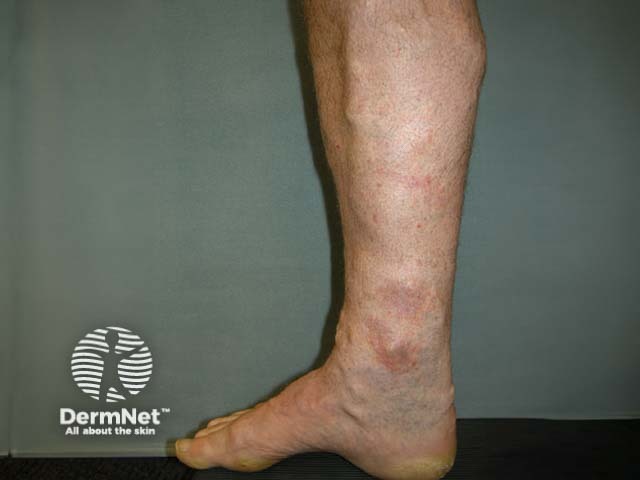
Varicosities and venous eczema
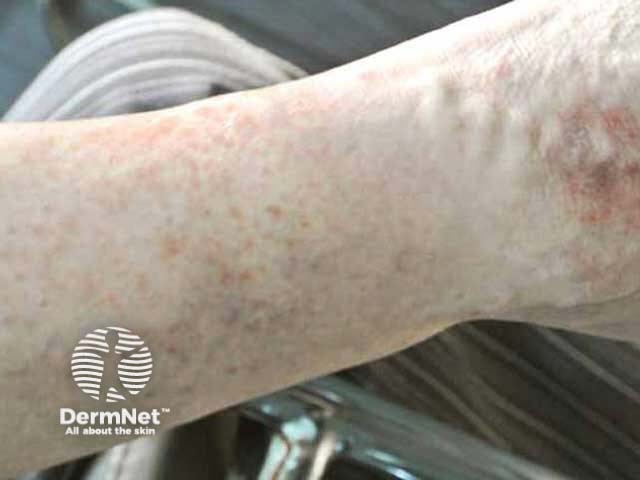
Pinpoint pigmentation
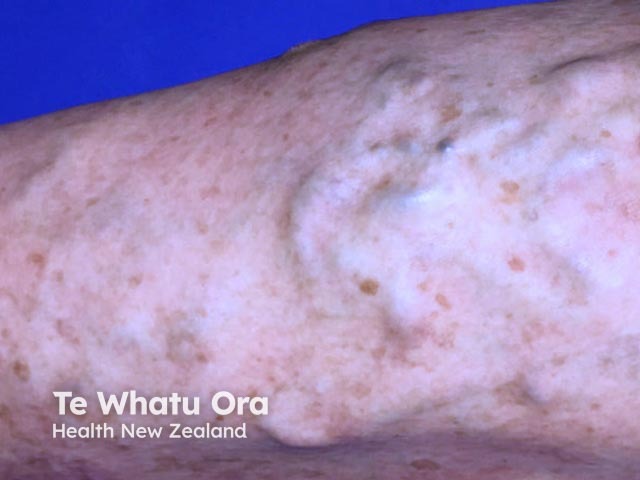
Varicosities and pigmentation
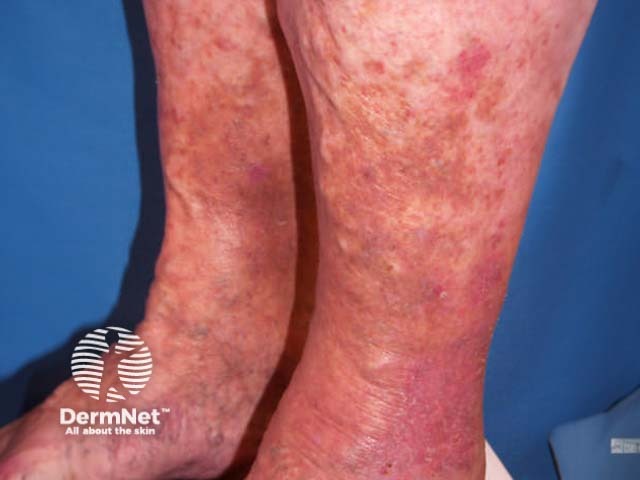
Patchy rusty-red pigmentation
Venous insufficiency in Thai patients has been reported to be less likely to be associated with pain, oedema, inflammation, and visible varicose veins compared to ethnic whites.
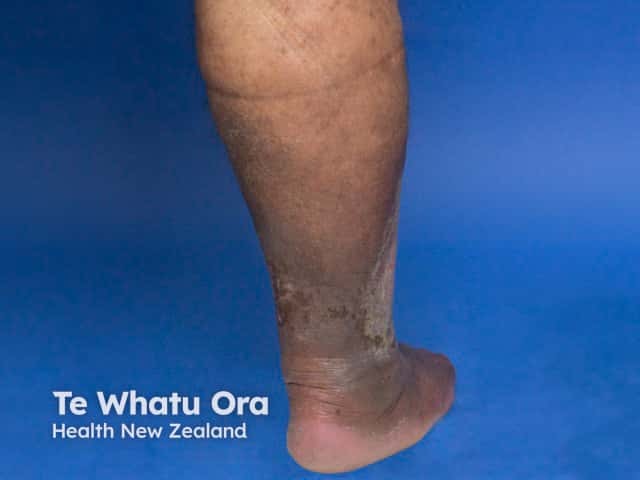
Venous eczema
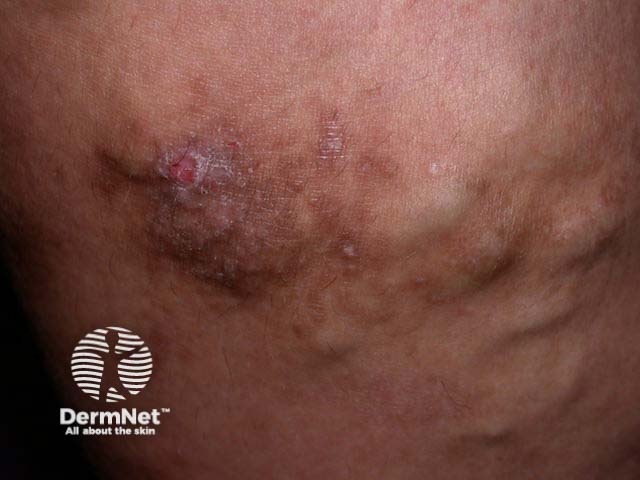
Varicose eczema
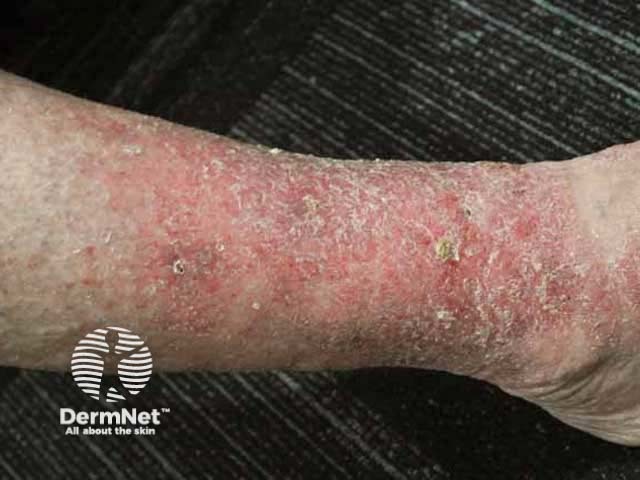
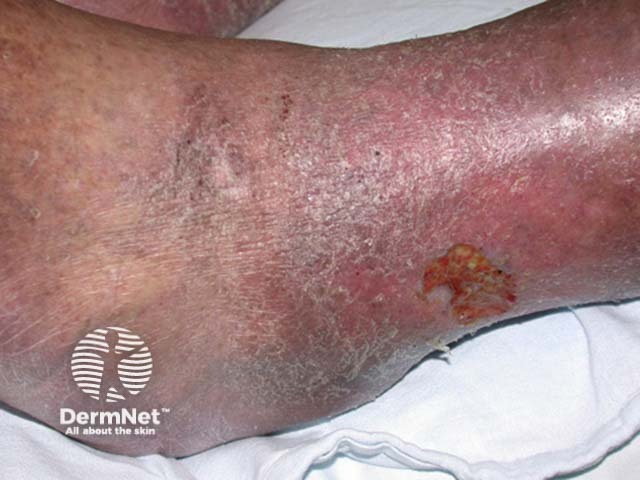
Leg ulcer
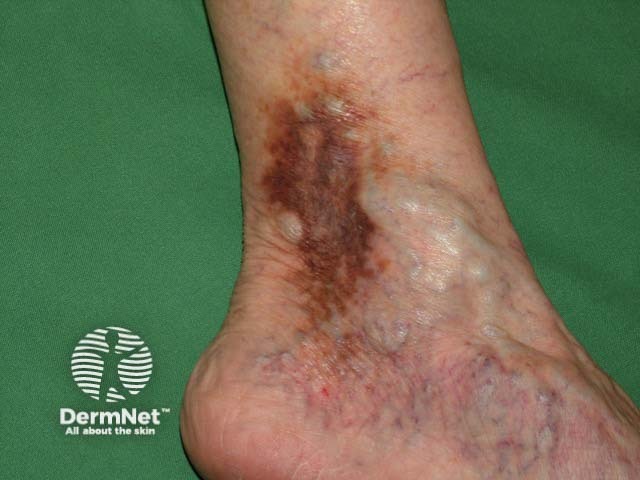
Leg ulcer
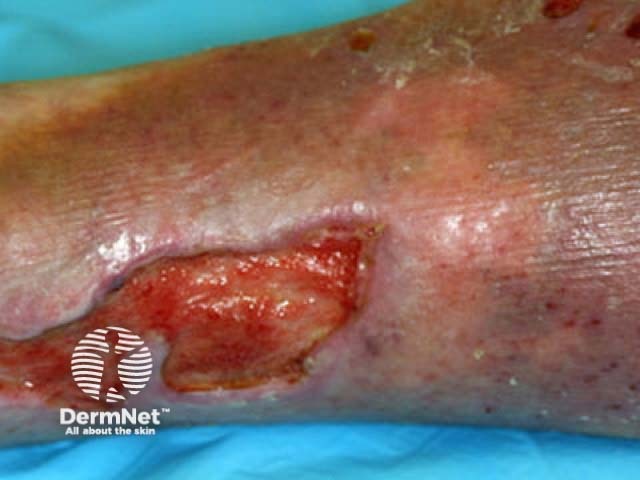
Venous ulcer
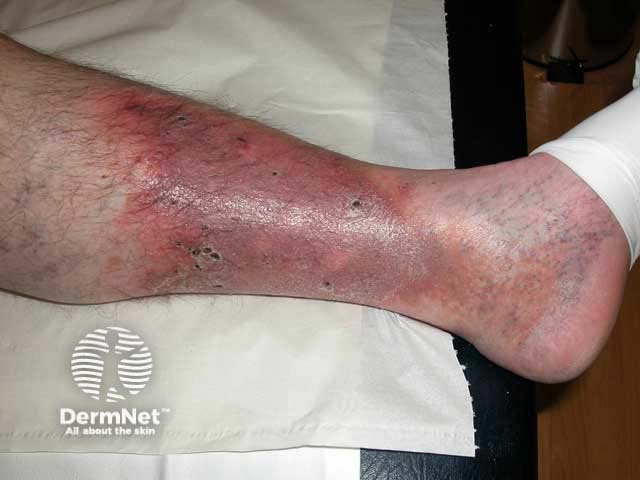
Lipodermatosclerosis and erosions
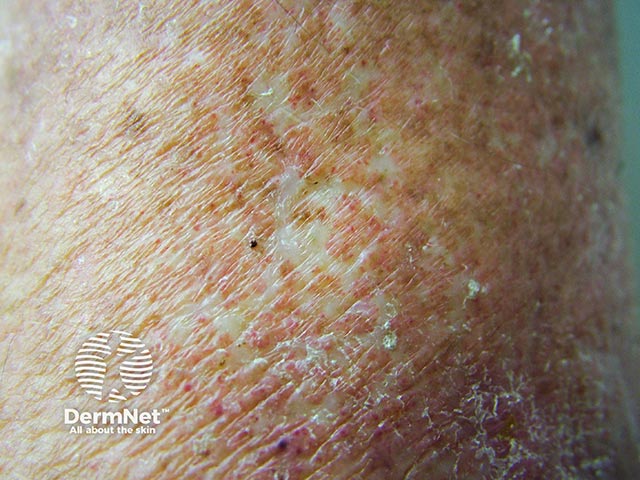
Atrophie blanche
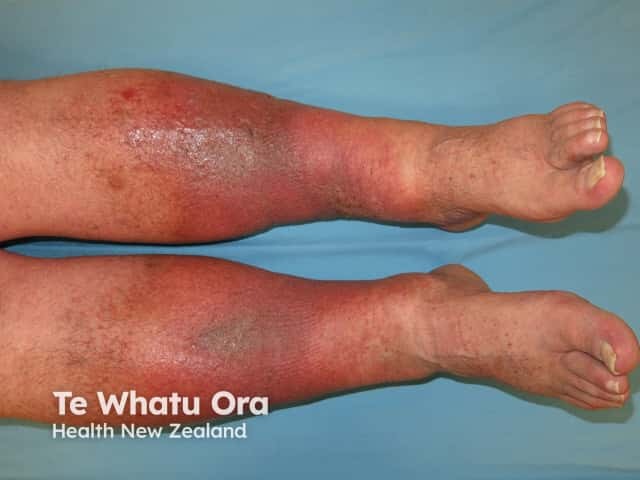
Venous eczema and lipodermatosclerosis
Venous insufficiency is usually diagnosed on history and examination. Varicose veins may require the patient to be standing to appreciate. Duplex ultrasonography is the preferred investigation to demonstrate reflux and communications between the deep and superficial venous networks.
The CEAP (Clinical, Etiologic, Anatomic, Pathologic) system is used categorise and classify venous insufficiency but is unhelpful as a severity score. [see details Varicose veins]
The corona phlebectatica paraplantaris is a clinical sign of severe venous stasis. Specifically, blue telangiectases and capillary stasis spots may be the most useful correlates with the severity of chronic venous insufficiency.
Venous insufficiency is inexorably progressive. The rate of complication development is not known.
Most patients with chronic venous insufficiency will experience at least intermittent episodes of venous eczema.
Leg ulceration is the most important complication and is a major burden for health systems throughout the world. Estimates suggest 4% of patients with varicose veins will develop venous leg ulcers in their lifetime.