Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Ramez Barsoum, Resident Medical Officer, Princess Alexandra Hospital, Brisbane, QLD, Australia. DermNet Editor in Chief: Adjunct A/Prof Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. April 2019.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Varicose veins are engorged, tortuous, green, blue, or purple veins that are often found on the lower legs and feet.
Varicose veins are also called varices or varicosities.
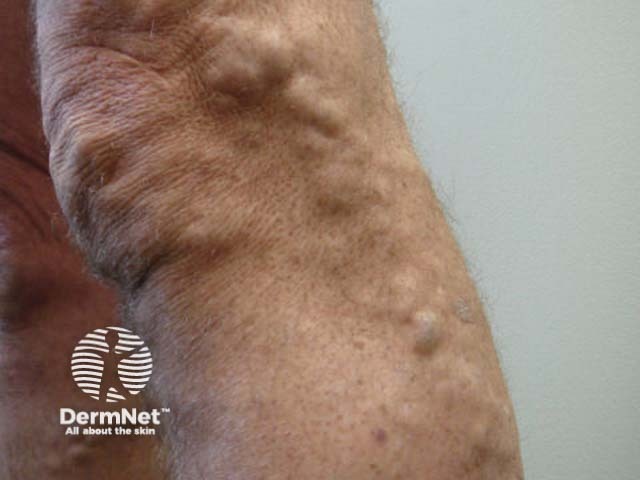
Varicose veins
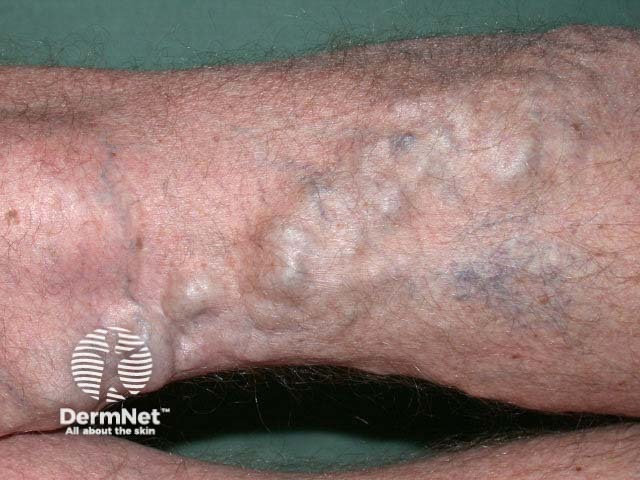
Varicose veins
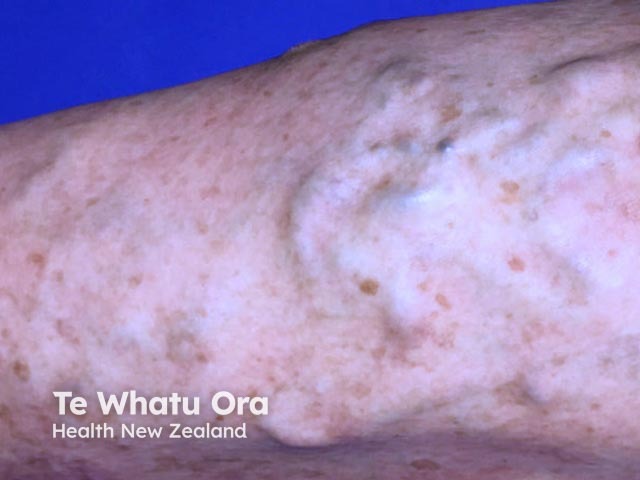
Varicose veins
Approximately one-third of men and women aged 18–64 years have varicose veins [1]. They are more common in women and those with a family history of venous disease.
In normal leg veins, one-way valves direct the flow of venous blood from superficial venules to larger superficial veins, then to the deep veins, and eventually to the heart. Muscle contractions create a pumping action to help the flow of blood to the heart (known as the venous return). In the legs, varicose veins are a manifestation of venous insufficiency.
Risk factors for varicose veins include:
Patients with varicose veins present because they are unsightly and because of a feeling of discomfort, heaviness, itching, or a dull ache. Patients can also present with complications such as bleeding, ulceration, and thrombophlebitis.
Superficial veins are prone to trauma and can bleed, which can be potentially life-threatening [6,7].
The increased pressure in varicose veins allows proteins, hormones, and circulating proinflammatory molecules to leak out of the vein and into the extravascular space, which leads to localised inflammation and the formation of a chronic venous leg ulcer.
Phlebitis is inflammation of a vein with erythema and painful hardening. It is often associated with a blood clot (thrombosis) that arises as a result of the sluggish circulation and factors that increase coagulation. Phlebitis may be superficial (ie, superficial thrombophlebitis) or deep (ie, deep venous thrombosis) [6].
Venous stasis dermatitis is associated with increased venous pressure and pro-inflammatory molecules. Patients present with brown discolouration, pruritus, and discoid or circumferential, acute or chronic eczema on the distal lower limbs [7].
Lipodermatosclerosis is an inflammatory and thickened form of panniculitis resulting from the presence of pro-inflammatory molecules, poor venous outflow, and hypertension. The lower leg becomes reddened in acute lipodermatosclerosis and indurated in chronic lipodermatosclerosis.
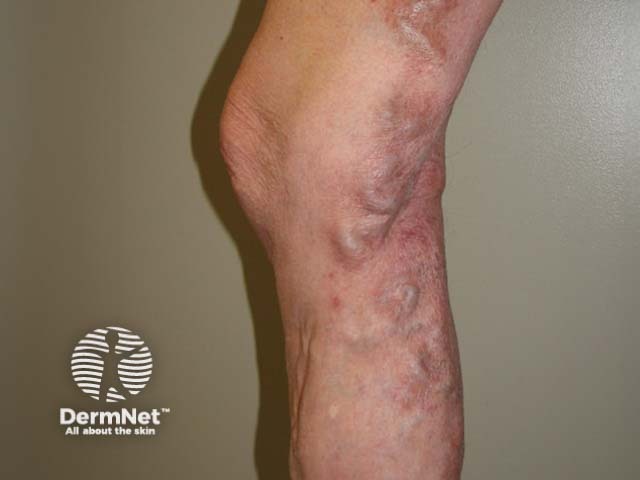
Haemosiderin deposition
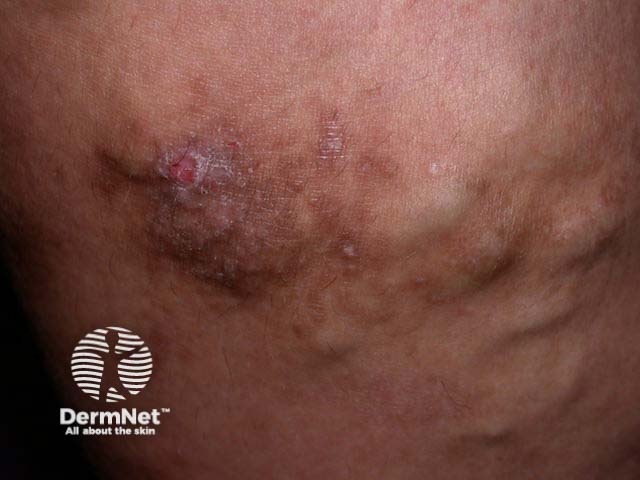
Varicose eczema
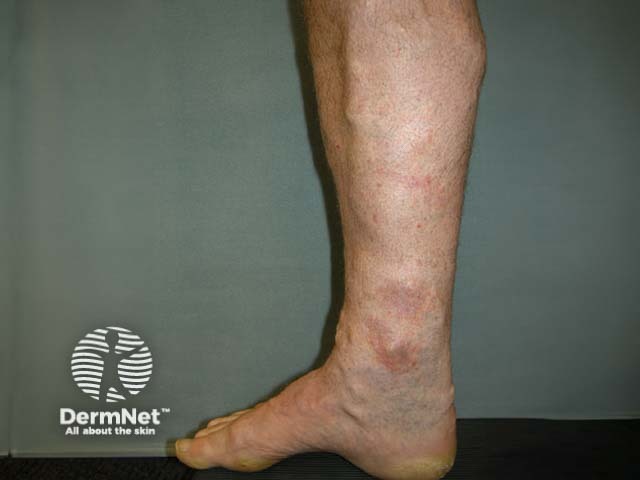
Stasis eczema
Varicose veins are diagnosed clinically. A physical examination should include the entire venous system and it is usually conducted with the patient both lying down and standing up.
The UK's National Institute for Health and Care Excellence (NICE) uses the Clinical–Etiological–Anatomical–Pathophysiological (CEAP) classification of varicose veins.
The CEAP classification categories are as follows:
A Duplex Doppler ultrasound assessment should be performed to determine the extent of disease and the level of truncal reflux (the failure of one of three of the main trunk veins) and to plan treatment options [8].
Varicose veins are larger than telangiectasia (small red 'thread' veins, < 1 mm in diameter) and venulectasia (blue reticular vessels, 1–3 mm in diameter). These are not detected on duplex ultrasound.
Weight loss (if overweight) and moderate physical activity should be encouraged in patients with varicose veins to reduce the risk of complications. Compression hosiery should be used to relieve discomfort and swelling, especially when travelling.
Treatment for varicose veins is available from a vascular service. Options for treatment are listed below.
Endovenous thermal ablation, using either a laser or radiofrequency device, causes an irreversible thermal injury in the vein wall, which leads to scarring and the absorption of the tissue over several months. The success rate for both methods of ablation is 95% [9,10].
Sclerotherapy involves the injection of a sclerosant solution into the veins under ultrasound guidance to cause inflammation in the vessels and the eventual collapse of the varicose network. Smaller surface veins can be injected by microsclerotherapy, involving smaller gauge needles with smaller amounts of sclerosant [11].
Endovenous adhesive ablation, or 'vein glue' technique, involves the injection of a medical-grade adhesive cyanoacrylate glue through a catheter. Long-term safety and efficacy data are lacking for this procedure [12].
ClariVein is a rotating occlusion catheter that mechanically agitates the vein lining while also spraying a liquid sclerosant. It can induce endothelial damage but lacks long-term data about its use [13].
Surgeries such as high-ligation (tying of veins), vein-stripping and avulsion (the tearing out of veins surgically) are less often used to treat varicose veins than in the past due to the post-operative morbidity, recurrence rates, and risks associated with anaesthesia and hospitalisation [10].
Telangiectasia and venulectasia can be treated with long-wavelength vascular lasers, but such lasers are unsuitable for larger varicose veins [14].
Whichever treatment option is used, varicose veins may recur and can usually be treated again. [14].