Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Treatments Blood vessel problems
Author: Author: Dr Amanda Oakley, Dermatologist, Waikato Hospital, 2003.
Sclerotherapy is an injection technique used to get rid of veins. Most often it is used to treat leg veins, but it may also be used for venous malformation, or blue vessels on the sides of the nose and elsewhere.
No anaesthetic is required. A strong solution (the sclerosant) is injected directly into the blood vessel causing inflammation of the walls of the vessel. The vessel disappears over a few weeks to months.
Microsclerotherapy, using a tiny needle, is the best way to treat venulectasia (blue veins) on the legs.
Larger varicose veins may also be treated by sclerotherapy especially if they are tortuous or recurrent (endovenous laser treatment may be preferred for straight veins or on the first occasion). First, a Duplex ultrasound scan should be performed to map out the path of superficial, perforator and deep veins. Those greater than 5 mm in width and demonstrating reflux are the most suitable for treatment. Sclerotherapy of larger superficial veins and perforator vessels is usually performed with ultrasound (echo) guidance. Best results are achieved using a foam sclerosant, where the sclerosant solution is mixed with air in a ratio of 1:4 to form minute bubbles. This provides a greater volume to push the blood away so the sclerosant may adhere more effectively to the blood vessel wall.
Arteries are not treated by sclerotherapy.
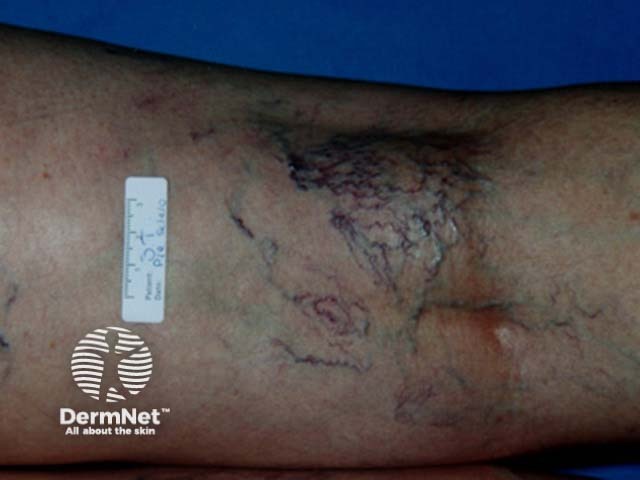
Before treatment
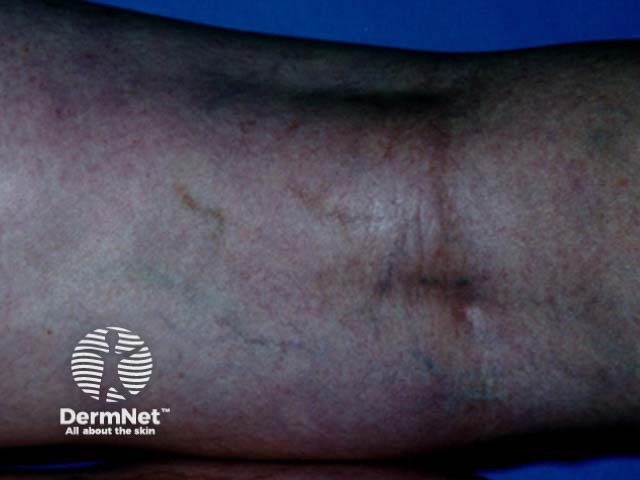
After sclerotherapy
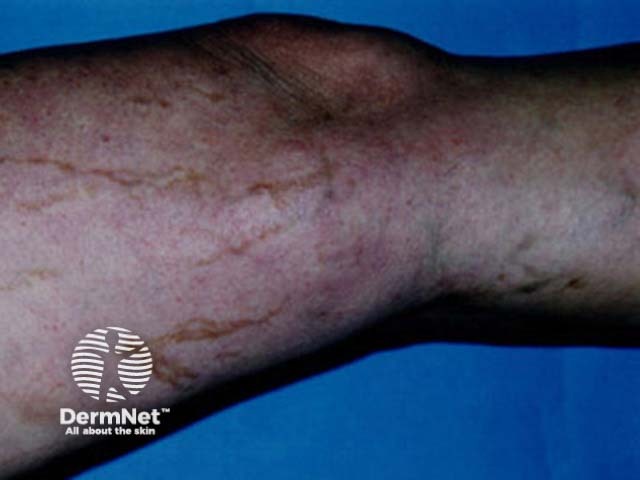
Staining
Sclerosant chemicals include:
Repeated treatments may be necessary at six- to twelve-weekly intervals to achieve up to 85% success at three years.
Although each session may involve a large number of injections, the needle used is very fine so that pain is not generally a problem. There may be some stinging as the solution travels through the smaller vessels. These become red and slightly swollen, sometimes itchy for a few hours.
Often cotton wool pads under adhesive plasters are applied to the injection sites. Pressure is applied to the treated vessels using Grade 2 graduated compression hosiery (support stockings) and/or bandages. These are usually worn for between seven days and three weeks following each treatment. They come in different sizes and colours.
Patients are usually able to return to normal daytime activities immediately after sclerotherapy. They should walk for at least thirty minutes a day, especially for the first few days following the procedure. Vigorous physical activities such as weight lifting or aerobics classes are not advised during this time.
In most cases, the pain, discomfort and swelling associated with the veins disappear within days, and the vessels slowly resolve over several months. Serious complications following sclerotherapy are rare.
The following side effects occur more frequently.
Very fine vessels may be too small to inject, in which case a vascular laser or intense pulsed light treatment may be worth trying.