Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2009. Updated September 2014.
Introduction
Generalised hyperpigmentation
Localised hyperpigmentation
Treatment of hyperpigmentation
Generalised hypopigmentation
Localised hypopigmentation
Leukoderma
Treatment of hypopigmentation
Pigmentation of the skin normally varies according to racial origin (see Fitzpatrick phototypes) and the amount of sun exposure. Pigmentation disorders are often more troublesome in skin of colour.
The melanocytes (pigment cells) are located at the base of the epidermis and produce the protein melanin. Melanin is carried by keratinocytes to the skin surface. The melanocytes of dark-skinned people produce more melanin than those of people with light skin. More melanin is produced when the skin is injured, for example following exposure to ultraviolet radiation. The melanisation process in dark skin is protective against sun damage, but melanisation in white skin (for example after sunburn) is much less protective.
Hormonal effects of oestrogen during pregnancy or due to medication can cause pigmentation of nipples, vulva and abdomen (linea nigra).
Some skin diseases and conditions result in generalised or localised hyperpigmentation (increased skin colour, hypermelanosis), hypopigmentation (reduced skin colour, hypomelanosis), or depigmentation (absent skin colour, leukoderma).
A Wood lamp may be used to assess pigmentation during the examination of the skin, as pigmentary changes are often easier to identify while exposing the affected skin to long-wavelength ultraviolet rays (UVA).
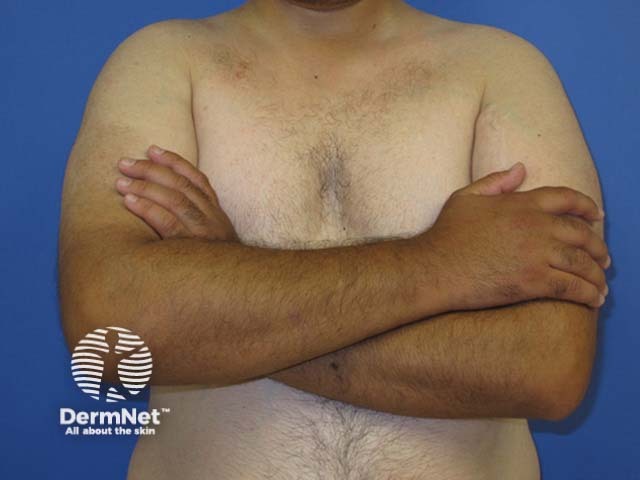
Suntan in dark skin
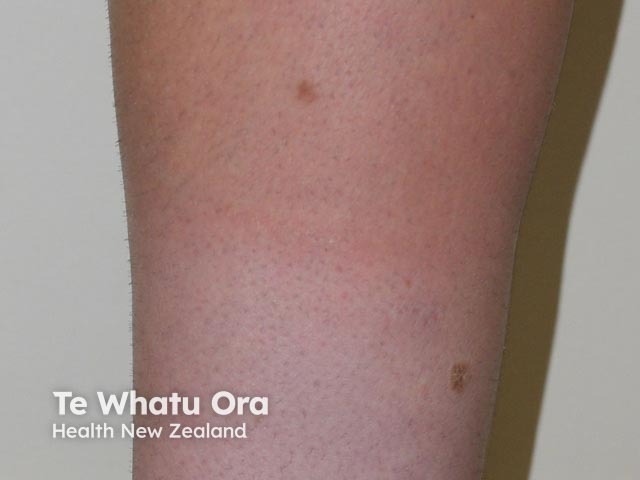
Suntan in fair skin
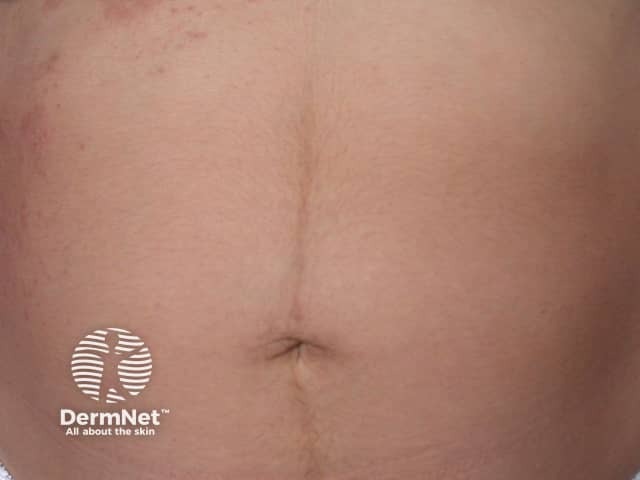
Hormonal pigmentation
Generalised hyperpigmentation or hypermelanosis may rarely arise from excessive circulating melanocyte-stimulating hormone (MSH) when it often has a bronze hue. It occurs:
A differential diagnosis is carotenoderma, in which the skin colour takes on a yellow-orange hue due to ingestion of coloured fruit and vegetables.
Localised pigmentation may be due to melanin, haemosiderin, or externally-derived pigment.
If dark patches are observed, the main diagnoses to consider are:
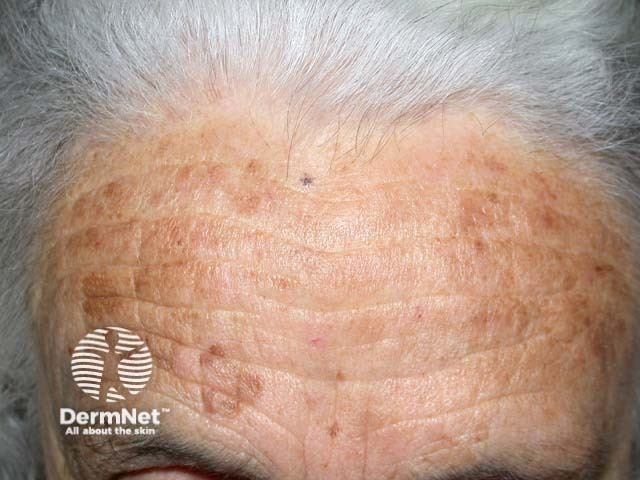
Diffuse lentiginosis
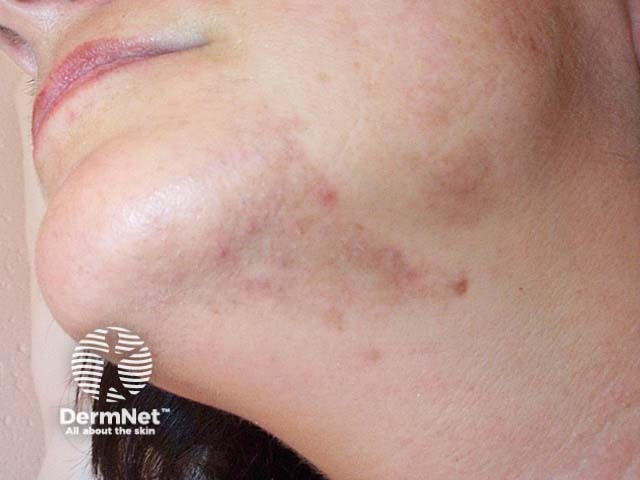
Postinflammatory pigmentation
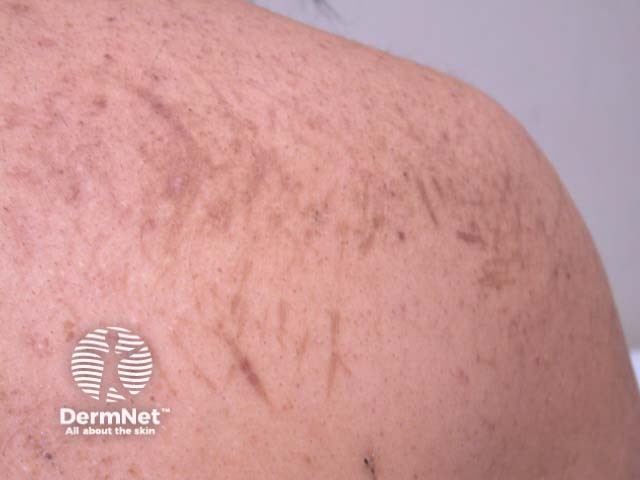
“Flagellate” pigmentation
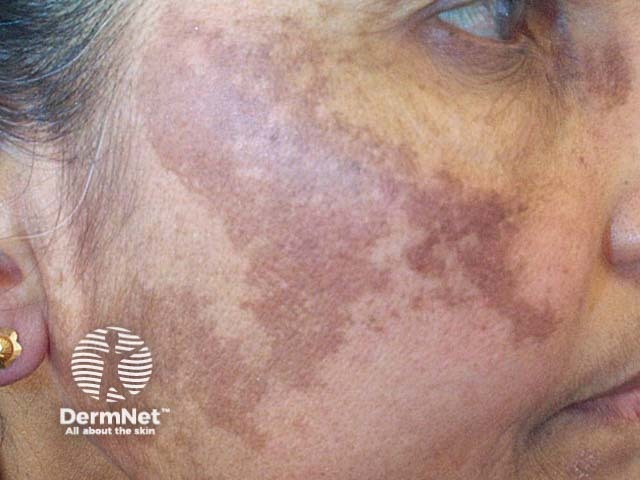
Melasma
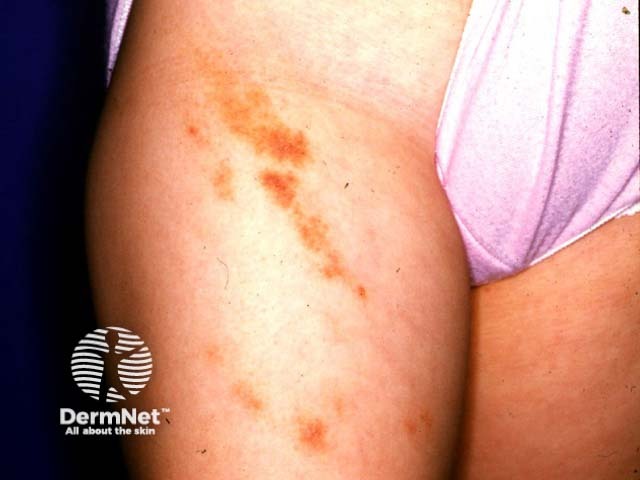
Capillaritis
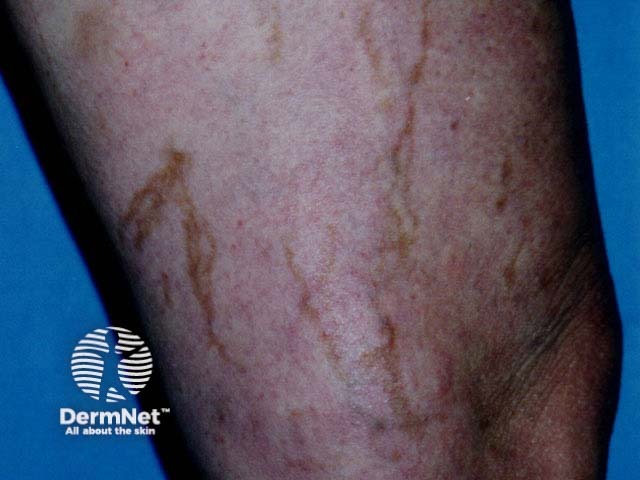
Post-sclerotherapy staining
If pigmentation due to melanin affects an exposed site, daily application of broad-spectrum SPF 50+ sunscreen is important to minimise darkening caused by UVR. This is not effective for melanin located in the dermis or to reduce pigmentation caused by carotene, drugs, or tattoos.
Cosmetic camouflage can be used.
The following agents can be used to lighten epidermal melanosis alone or, more effectively, in combination:
Resurfacing using chemical peels, laser (especially picosecond laser), intense pulsed light (IPL) or dermabrasion may be effective but unfortunately risks further damage to the epidermis and formation of more pigment. Cautious cryotherapy to small areas of postinflammatory pigmentation can be effective but risks causing permanent hypopigmentation.
Cosmetic camouflage using make-up is sometimes the best advice.
Generalised reduction in melanin pigmentation at birth (congenital) may be racial in origin or due to albinism. Pituitary failure resulting in lack of MSH rarely results in acquired generalised hypomelanosis.
Pallor is much more frequently due to blood loss or anaemia.
Localised hypopigmentation may be due to vascular changes or partial loss of melanin. It can be congenital or acquired.
If single or multiple pale patches are observed, diagnoses to consider include:
White depigmented patches (leukoderma) may be due to:
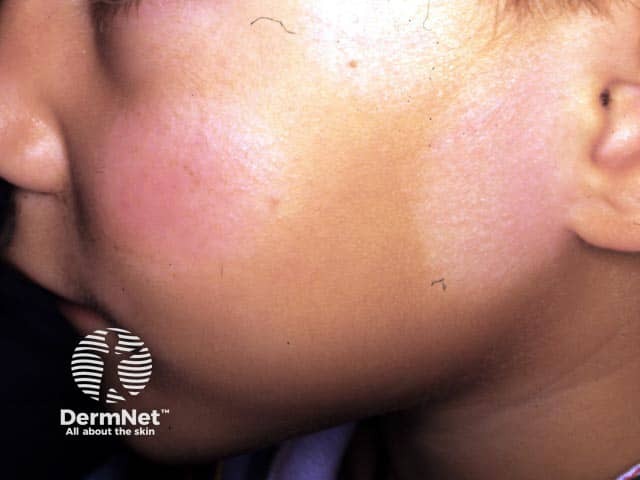
Pityriasis alba on the cheeks
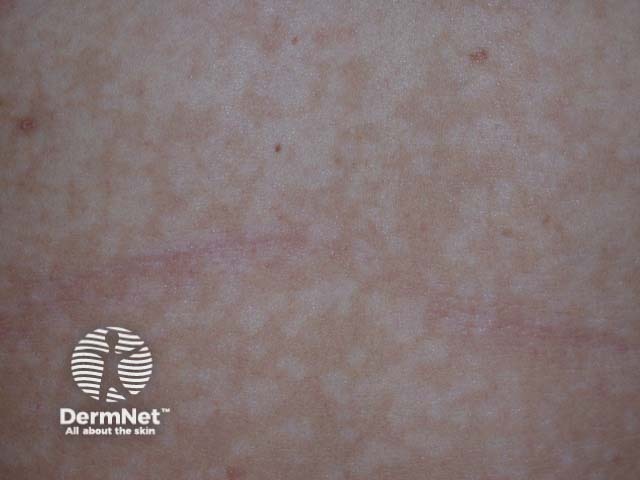
Pityriasis versicolor
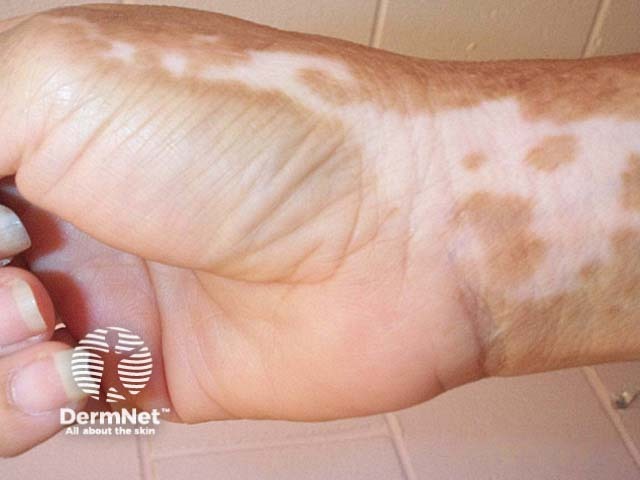
Thermal burn
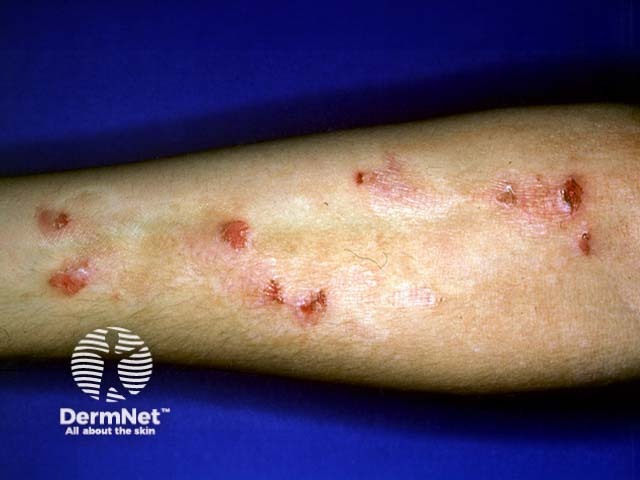
Longstanding prurigo
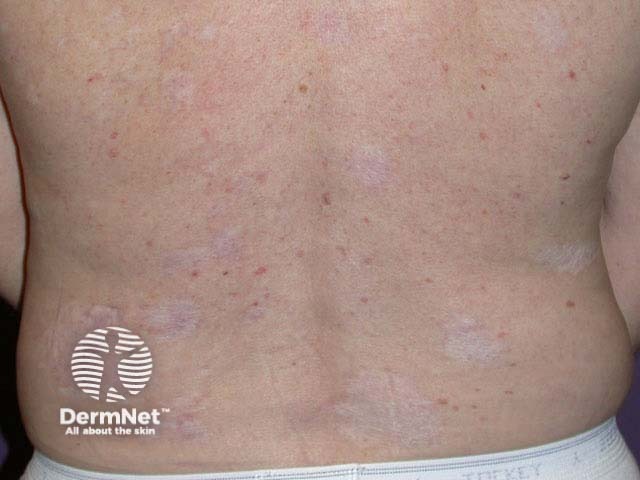
Surgery and cryotherapy
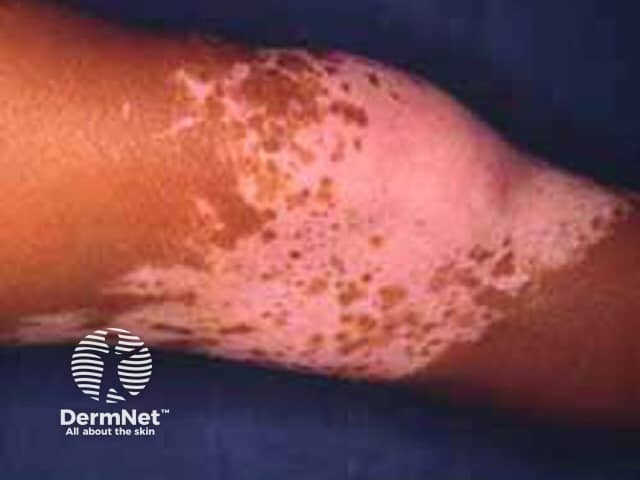
Vitiligo
Hypopigmentation due to inflammatory skin disorders and infections usually resolves by itself over weeks to months once the underlying disorder has been cleared. There is no effective treatment for achromia due to scarring. The response of vitiligo to therapy is highly variable.