Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Rajan Ramji, Final Year Medical Student, University of Auckland, Auckland, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editors: Gus Mitchell/Maria McGivern. June 2017.
Introduction
Introduction - skin of colour
Demographics
Causes
Clinical features
Diagnosis
Differential diagnoses
Treatment
Outcome
Melanoma is a form of skin cancer formed from the uncontrolled growth and replication of melanocytes (pigment cells) [1]. Melanoma is sometimes referred to as malignant melanoma and has a variety of subtypes.
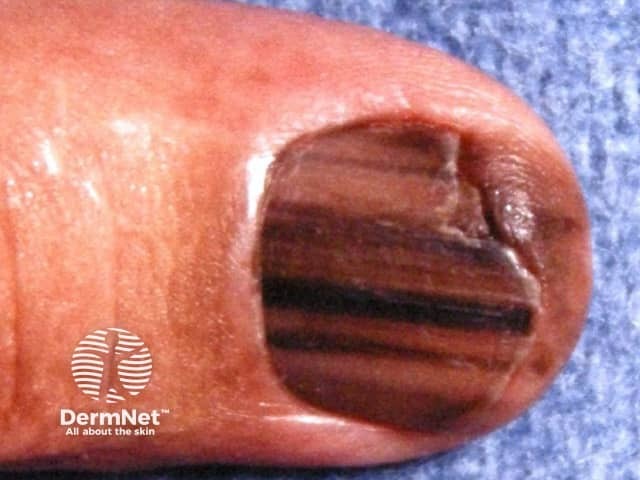
Ungual melanoma
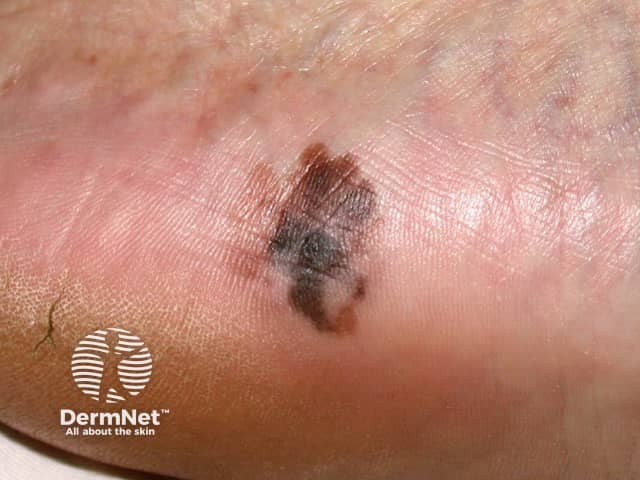
Acral lentiginous melanoma

Nodular melanoma
‘Skin of colour’ is a subjective term used to refer to a natural skin pigmentation ‘darker’ than white (ie, brown or black skin). When compared against a graded assessment of skin colour, such as as the Fitzpatrick phototypes, skin of colour may refer to skin classified as type IV or higher [2]. In some contexts, skin of colour is also used to describe the skin of different non-white ethnic groups, including those of African, Asian, South American, Pacific Island, Maori, Middle Eastern, and Hispanic descent [3]. See ethnic dermatology.
Melanoma may develop in any skin type, but it is most commonly seen in those with light coloured skin. Conversely, a darker skin colour is associated with a reduced risk of developing melanoma [4]. This trend is evident when comparing the rates of melanoma seen in diverse ethnic groups predisposed to different skin colours.
In the USA during the period from 1999 to 2006, of 288,741 advanced melanoma patients [5]:
In New Zealand during the period from 1996 to 2006, of 16,425 newly registered cases of melanoma [6]:
Skin colour is an independent but significant risk factor for melanoma across diverse ethnic groups, with most cases being diagnosed at a median of 50–65 years of age [5].
People with skin of colour tend to have:
People of all skin colours with a family history of melanoma are at increased risk of developing melanoma due to a genetic predisposition [8].
Melanoma is due to uncontrolled proliferation of melanocytic stem cells following progressive genetic transformations [1,9,10].
In most cases, this genetic change is triggered by sun exposure. Ultraviolet (UV) radiation damages and mutates the DNA [9,10]. In darker skin, a higher content of UV radiation-absorbing melanin is protective [7,11,12], and the use of sunscreens is not required to protect them from melanoma.
Melanoma may also arise in areas not exposed to sunlight and in tissue other than the skin. The rates of these melanomas can be higher in non-white ethnic groups [13].
Melanoma can occur anywhere on the skin. In skin of colour, melanoma frequently develops in sites that have low sun exposure, such as the palms or soles (acral lentiginous melanoma) [5,6,14,15]. Less commonly, melanoma may occur on mucous membranes, such as the mouth or genitals, or in other parts of the body, including the brain and the eyes.
It can be harder to identify melanomas, their growth phase, and their pattern in skin of colour as the surrounding skin may mask or match the colour of the melanoma. Characteristic features follow. Note: these features are not always present and do not always indicate malignant growth [1,4].
Melanoma in skin of colour may develop from normal skin or other skin lesions, including [1,16]:
Skin lesions of concern are compared with the person’s other skin lesions. If they appear distinctive, they are often examined using by dermoscopy to look for features not otherwise identifiable with the naked eye. Diagnosing melanoma by visual inspection can be difficult — especially in skin of colour where, as mentioned above, the surrounding skin may mask or match the colour of the melanoma [1,4].
Suspicious lesions are then surgically removed for pathological examination (diagnostic excision) using a 2–3 mm margin around the lesion. Partial biopsies are sometimes considered for larger suspicious lesions [1].
Pathological diagnosis of melanocytic lesions can also be difficult. The use of immunohistochemical stains may be considered to confirm whether a suspicious lesion is a melanoma [1].
Differential diagnoses for melanoma include:
In skin of colour especially, the following diagnoses should be considered as alternative diagnoses.
Naevi of special sites are naevi that develop in atypical areas, including the genitals, breasts, palms, soles of the feet and flexural regions (armpits, elbows, backs of knees). While benign, they may show a histological structure similar to melanoma. This diagnosis should particularly be considered in skin of colour, as these naevi occur in sites where melanoma commonly occurs in these skin types [5,6,11,14,15].
Postinflammatory hyperpigmentation is the darkening of the skin following inflammation; this is often is more intense and persistent in skin of colour, which may cause undue distress and confusion in patients [12].
A keloid scar is a raised scar that grows beyond the boundaries of the original injury. Keloid scarring is more common in skin of colour and may resemble a resemble a desmoplastic melanoma (which is very rare) [17–19].
Confirmed melanoma usually undergoes a second surgical procedure known as wide local excision. The clinical margins of this excision are dependent on the size and thickness of the melanoma [1]. The Recommended New Zealand margins for excision of melanoma are as follows:
It is also important to determine the extent or ‘stage’ of the melanoma and whether it has spread from the site of origin. The American Joint Committee on Cancer (AJCC) cutaneous melanoma staging guidelines (2009) are the commonly used staging criteria. The AJCC staging criteria for cutaneous melanoma are as follows [20]:
Note: non-cutaneous forms of melanoma may have different staging criteria [1,20].
If a melanoma spreads beyond its site of origin (becoming ‘metastatic melanoma’), the surrounding lymph nodes may become enlarged. In such cases, the lymph nodes should be surgically removed under a general anaesthetic [1].
Normal, unenlarged lymph nodes may also be tested to identify microscopic spread of melanoma; this test is called a sentinel node biopsy and may help in cancer staging [1].
Systemic therapies may be offered in cases of advanced melanoma or metastatic melanoma (AJCC stages IIB, IIC and IIIC) [21].
Immunotherapy involves the use of drugs that stimulate the body’s immune system to work against melanoma cells; it can include:
Chemotherapy drugs for melanomas have demonstrated limited success in treating melanoma and are not thought to improve overall survival [21]. They include:
Targeted therapy drugs are offered to patients with advanced or non-operable melanomas that express specific mutations [21].
Targeted chemotherapies for melanoma available in New Zealand include [27–32]:
Radiotherapy may be given over several weeks in the treatment of persistent melanomas or melanoma unsuitable for excision. In metastatic melanoma, radiotherapy may be used to alleviate the symptoms associated with metastases [21,33].
The prognosis for melanoma in skin of colour may be poorer overall compared to melanoma in white skin. This could be due to late presentation or detection leading to thicker melanomas or more aggressive subtypes of melanoma [4–8]. Regardless of skin colour, prognosis is generally dependent on the AJCC stage of melanoma, Clark level of invasion, and Breslow thickness at the time of excision of the primary lesion [1].
The 5-year survival rates (%) according to the simplified AJCC staging classification [34] are as follows:
The 5-year survival rates at different tumour depths for differing ethnic groups from 17 US population-based cancer registries in the period from 1999 to 2005 are shown in Table 1 [5].
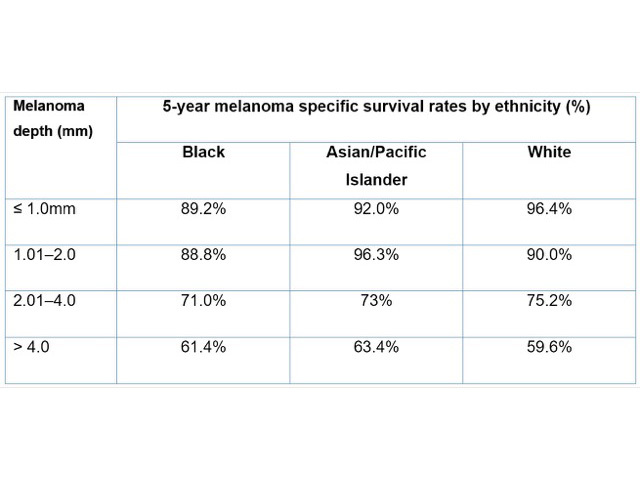
Table 1. Five-year survival rates by melanoma depth and ethnicity