Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Cutaneous metastasis (plural ‘metastases’) refers to the growth of cancer cells in the skin originating from internal cancer. In most cases, cutaneous metastasis develops after the initial diagnosis of the primary internal malignancy (such as breast cancer and lung cancer) and late in the course of the disease. In very rare cases, skin metastasis may occur at the same time or before the primary cancer has been discovered and may be the prompt for the further thorough investigation.
Cutaneous metastasis may also occur from skin cancer, usually melanoma. The original or ‘primary’ melanoma produces metastases or ‘secondary’ growths in surrounding or distant skin sites and other tissues such as the lungs or brain.
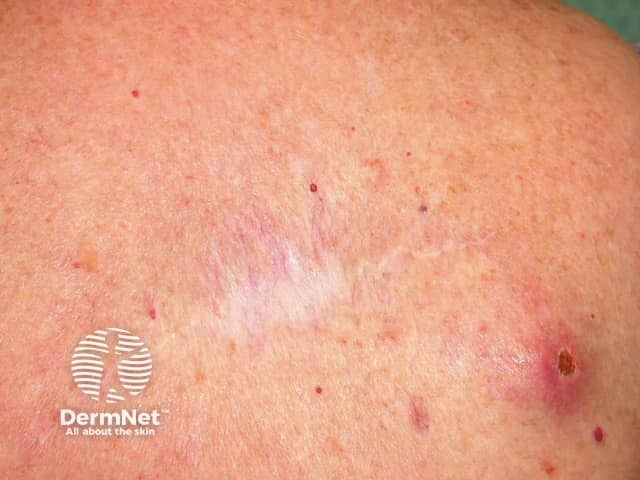
Metastatic melanoma near excision site
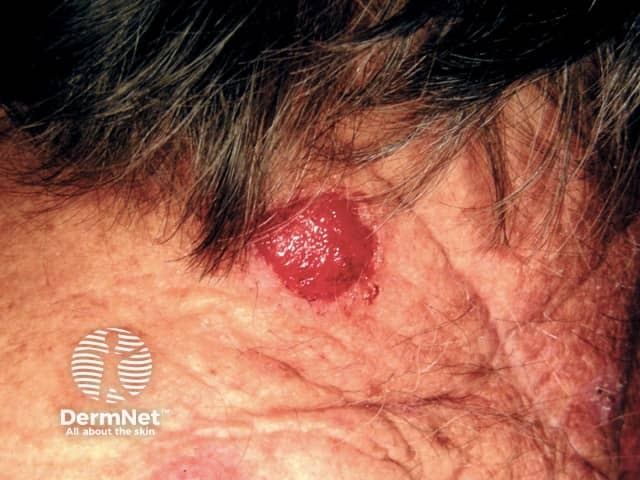
Distant metastatic melanoma
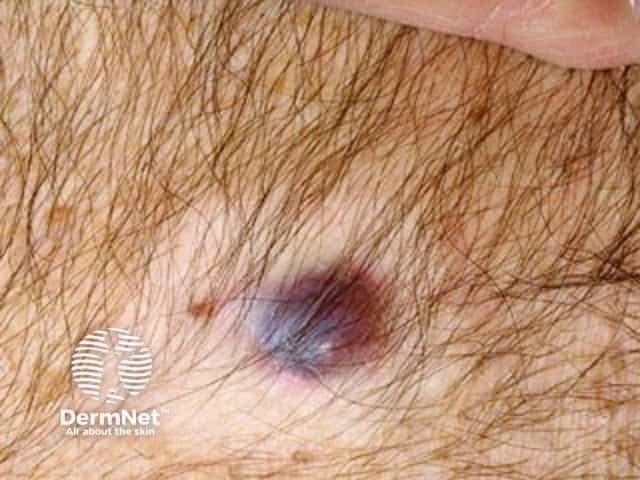
Metastatic melanoma
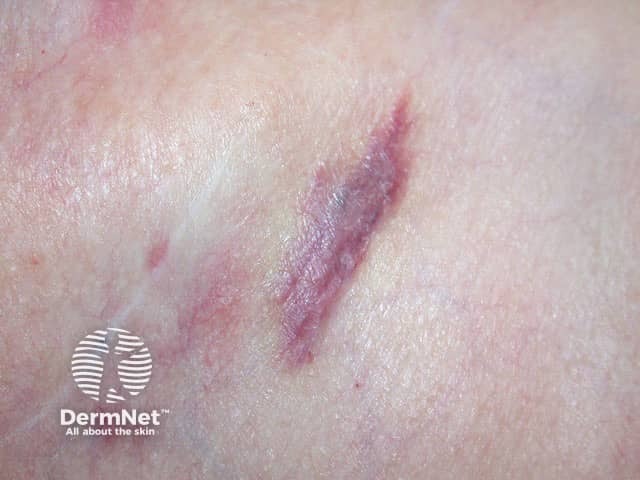
Metastatic breast cancer
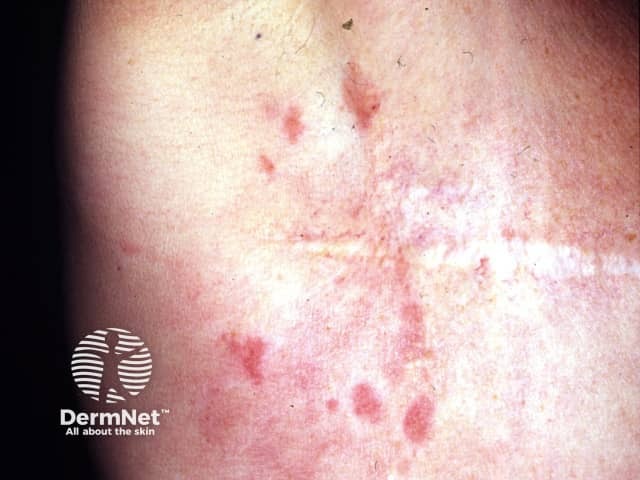
Metastatic breast cancer
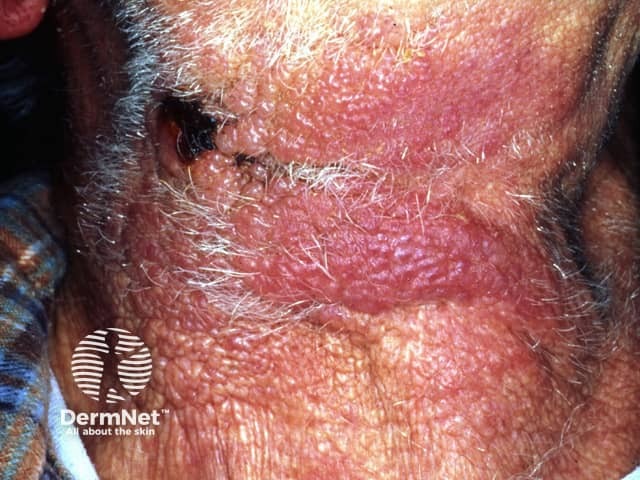
Metastatic adenocarcinoma of unknown origin (carcinoma erysipeloides)
Cutaneous metastasis occurs when cancerous cells break away from a primary tumour and make their way to the skin through the blood circulation or lymphatic system. Most malignant tumours can produce skin metastasis, but some are more likely to do so than others. When the following cancers have metastasised, they have quite a high chance of affecting the skin.
The incidence of skin metastasis varies but is somewhere between 3—10% in patients with a primary malignant tumour.
The sex and age of an individual also appear to determine the frequency of skin metastasis in certain primary cancers. The reason for this is unknown. In women, about 70% of cutaneous metastases originate from the breast. In men, cutaneous metastases are most often from the lung (24%), colon (19%), skin (melanoma, 13%) or oral cavity (12%).
Below lists the common internal cancers that cause skin metastasis in decreasing order of frequency according to sex and age group.
Men |
Women |
||
|---|---|---|---|
40 yr |
> 40 yr |
40 yr |
> 40 yr |
Melanoma |
Lung cancer |
Breast cancer |
Breast cancer |
Most cutaneous metastasis occurs in a body region near a primary tumour. The first sign of the metastasis is often the development of a firm, round or oval, mobile, non-painful nodule. The nodules are rubbery, firm or hard in texture and vary in size from barely noticeable lesions to large tumours. These may be skin coloured, red, or in the case of melanoma, blue or black. Sometimes multiple nodules appear rapidly. The skin metastases may break down and ulcerate through the skin. Specific patterns include:
Depending on the location of the primary tumour, cutaneous metastasis display certain characteristic features.
Organ of cancer origin |
Features of cutaneous metastasis |
|
|---|---|---|
Breast |
|
|
Lung |
|
|
Melanoma |
|
|
Colon and stomach |
|
|
The underlying primary tumour needs to be treated. However, in most cases where skin metastasis has occurred, the primary cancer is widespread and may be untreatable. In this case, palliative care is given and includes keeping lesions clean and dry. Debridement can be done if lesions bleed or crust. Other therapies that may be helpful include:
In many cases, cutaneous metastasis causes disfigurement and discomfort. Removal of skin lesions by simple excision may enhance the patient’s quality of life but has little effect on the final outcome that is dictated by the primary cancer.