Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Nicole Kah Mun Yoong, St George Hospital, Australia; Hana Numan, Senior Medical writer, DermNet (2022)
Previous contributors: Hon A/Prof Amanda Oakley, Dermatologist, New Zealand (2010)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Prevention Outcome
A keloid scar is a firm, smooth, hard growth that occurs as a result of excessive scar formation. Keloids occur after skin injury; rarely, keloids can occur spontaneously without any significant preceding skin injury. They may develop on any part of the body and extend beyond the original wound margin, although the upper chest, shoulders, ears, and neck are especially prone to them.
Unlike keloid scars, hypertrophic scars are limited to the area of damaged skin. They are prone to occur when there is a lot of tension on a healing wound, the resultant scar is thicker than usual. Hypertrophic scars are more likely to regress and resolve compared to keloids as these tend to persist.
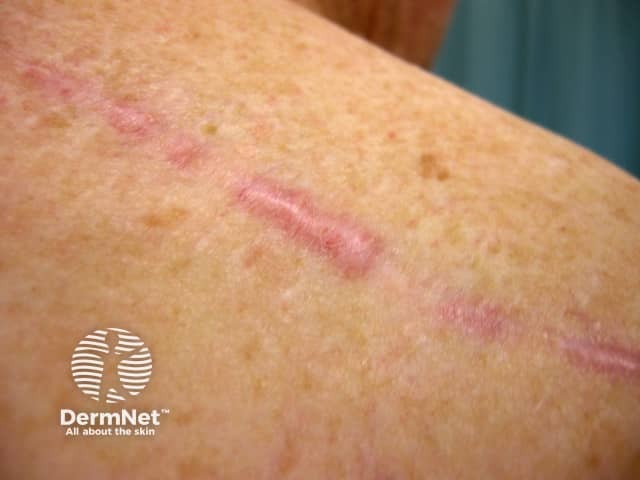
A hypertrophic scar on the upper back - the thickening does not extend beyond the confines of the injury
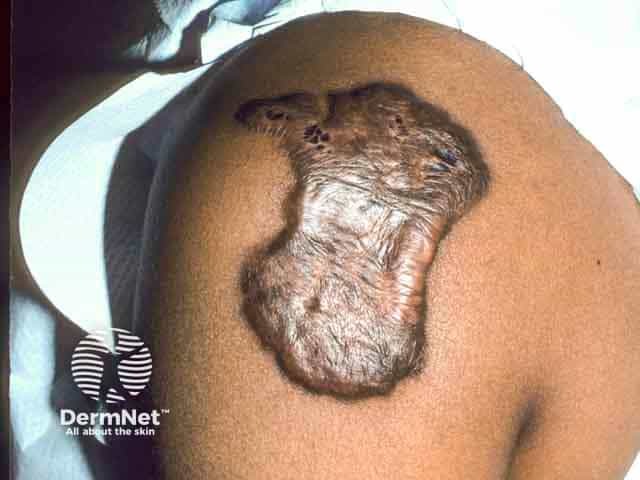
A large keloid on the deltoid area after smallpox vaccination

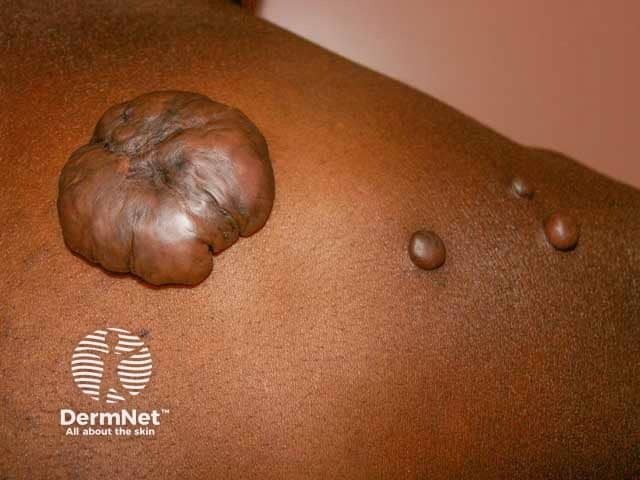
A large 'dumbbell' keloid on the earlobe
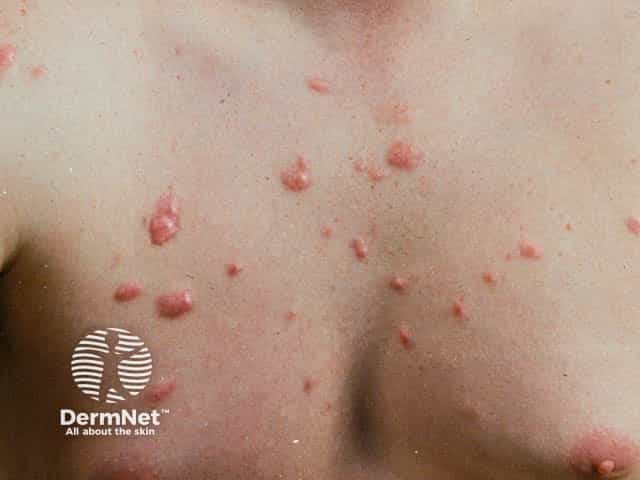
Post-acne keloid scars
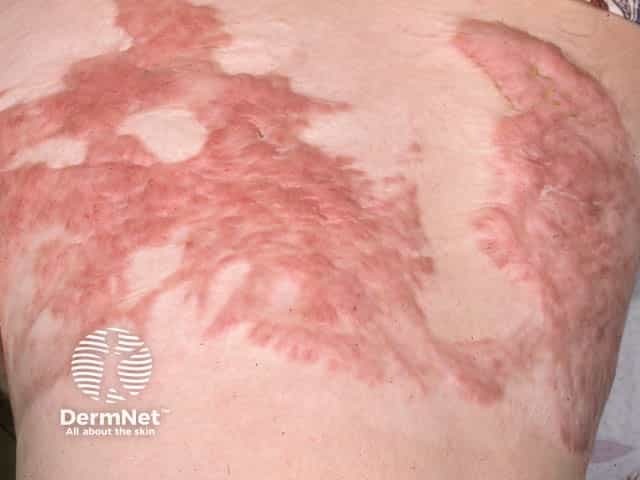
Keloid scarring after skin grafting
Keloids over the upper back
Hypertrophic scarring is common and can occur in all races and ages whereas keloid scars are less common and are more frequent in those with Fitzpatrick skin types III to VI.
Keloids are self-reported in 16% of Black individuals, and Chinese individuals are more likely to develop them when compared with those of Indian or Malaysian origin. White-skinned individuals and albinos appear to be the least affected. A genetic association has been noted with some HLA haplotypes and blood group A.
Multiple spontaneously arising keloids have been rarely associated with a number conditions including:
The exact pathogenesis of keloids and hypertrophic scar formation is unknown. Keloids may develop after minor injuries such as trauma, burns, insect bites, surgery, cryotherapy, topical therapies (eg, imiquimod), acne, infections (eg, shingles), and immunisation. They are more common in wounds that have been allowed to heal by secondary intention. Keloids can arise months to years after an injury.
The pathogenesis is hypothesised to involve dysregulation of the normal healing process resulting in excessive production of collagen, elastin, proteoglycans, and extracellular matrix proteins. There is an increase in the number of fibroblasts and mast cells. Growth factors and cytokines are altered in keloid scars, with increased amounts of TNF alpha, interferon-beta and interleukin 6.
Keloids are usually:
Hypertrophic scars are usually:
They most commonly occur in areas of high anatomic skin tension:
Keloids are more common in those with darker skin types; the lesions are less pink and more pigmented.
Keloids and hypertrophic scars are diagnosed clinically on the basis of history and clinical features. A skin biopsy may be needed if there is diagnostic uncertainty.
Although distinguishing between keloids and hypertrophic scarring can be difficult, it is important when considering intensive treatment options. Distinguishing clinical features include onset from injury, raised appearance, growth outside of wound margins, and regression.
The histology of hypertrophic scars may reveal:
Keloids may reveal:
Lesions that may mimic keloids in appearance include:
A hypertrophic scar may resolve spontaneously and is likely to respond better to treatment than a keloid. Conversely, keloids are likely to persist without spontaneous resolution and prove resistant to treatment.
The aims of treatment are to reduce the cosmetic disfigurement and functional problems caused by the keloid and reduce pain and itch.
The following measures are helpful in at least some patients:
Scar dressings should be worn for 12–24 hours per day, for at least 8 to 12 weeks, and perhaps for much longer.
As these often occur after trauma, the following strategies may help prevent their formation:
Hypertrophic and keloid scars are harmless and do not change into skin cancer. However, patients with keloids have a slightly higher risk of skin cancer than non-keloid individuals.