Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Jonathan Chan, Resident Medical Officer, Waikato Hospital, Hamilton, New Zealand. DermNet New Zealand Editor-in-Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Gus Mitchell. September 2017.
Introduction
Causes
Clinical features
Complications
Treatment
Noonan syndrome is a common autosomal dominant disorder associated with mutations in the Ras/mitogen–activated protein kinase (MAPK) pathway and is one of a group of conditions that are collectively known as RASopathies.
Noonan syndrome is characterised by:
Noonan syndrome is also known as:
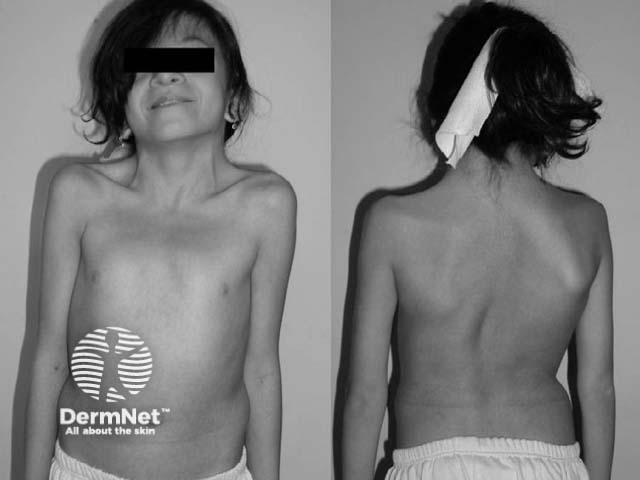
Noonan syndrome
Source: Wikipedia
Noonan syndrome is caused by mutations in the genes associated with the Ras/MAPK cell-signalling pathway, which is required for normal cell division, proliferation, differentiation and migration. These mutations lead to the loss of regulation of cell growth and division.
Mutations in the PTPN11 gene are implicated in over 50% of Noonan syndrome cases. Gene mutations in SOS1 are implicated in 10–15% of cases and mutations in the RAF1 gene and the RIT1 gene account for approximately 5% each. A number of other genes account for the rest.
The genetic cause behind Noonan syndrome is unknown in up to 20% of cases.
Noonan syndrome both sexes and all races; 50–70% of people with Noonan syndrome are of short stature. Weight and length at birth are usually normal, but growth slows over time. This is thought to be associated with abnormal levels of growth hormone.
Noonan syndrome presents with distinctive facial features, such as:
Other clinical manifestations of Noonan syndrome include:
Congenital heart disease is common in most cases of Noonan syndrome, with the most common defect being pulmonary valve stenosis.
Cutaneous symptoms of Noonan syndrome are varied and literature on the topic is limited. Documented cutaneous effects of Noonan syndrome include:
Noonan syndrome with multiple lentigines, formerly known as LEOPARD syndrome, is similar to Noonan syndrome. It has characteristic cutaneous features, including:
Hypertrophic cardiomyopathy is common in individuals with critical congenital pulmonary valve stenosis.
Individuals with Noonan syndrome have an eight-fold increased risk of developing haematological malignancies, the most common being leukaemia.
There is no specific treatment for the syndrome. Any complications such as heart disease should be monitored and treated according to symptoms, signs and the results of investigations.