Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. Updated by Dr Jonathan Chan, RMO, Waikato Hospital, 2017.
Noonan syndrome with multiple lentigines (NSML), formerly known as LEOPARD syndrome, is a very rare inherited disorder that is characterised by skin, heart, ear, genital, head and facial abnormalities. It is one of a group of syndromes collectively known as RASopathies.
The mnemonic LEOPARD describes these characteristic abnormalities associated with the disorder.
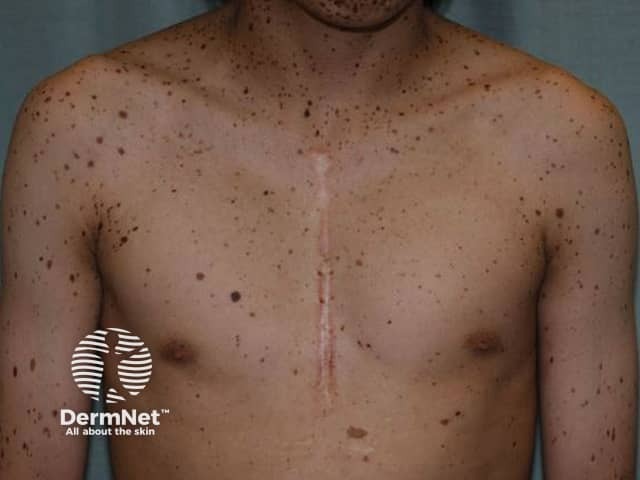
LEOPARD syndrome
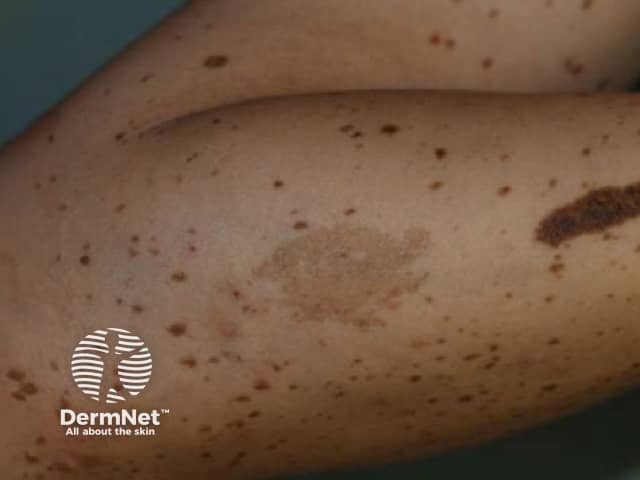
LEOPARD syndrome
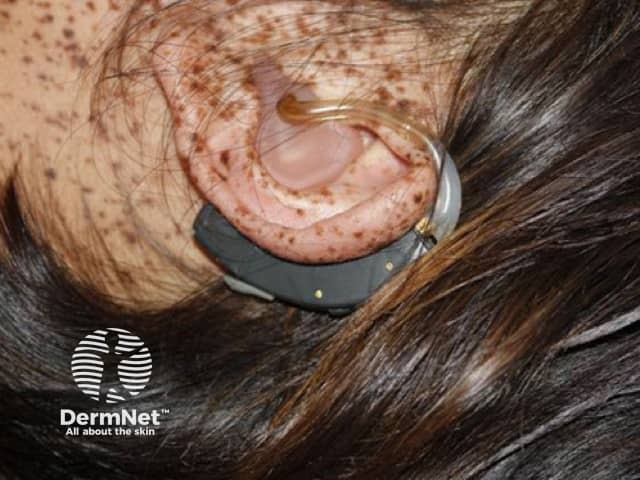
LEOPARD syndrome
Noonan syndrome with multiple lentigines is similar to the condition Noonan syndrome, with the two syndromes being difficult to discern from one another in early childhood. The characteristic dermatological features of each variant develop from later childhood to early teens.
The clinical features of Noonan syndrome with multiple lentigines vary considerably between patients, with most only manifesting 3–5 abnormalities. Lentigines are the most common feature of the syndrome and occur in more than 90% of patients. However, they do not have to be present to diagnose the syndrome.
The lentigines are small, dark pigmented flat or slightly raised lesions with well defined borders.
Other skin abnormalities include:
Non-cutaneous features of Noonan syndrome with multiple lentigines include:
Noonan syndrome and Noonan syndrome with multiple lentigines are classed as RASopathies. They are due to mutations in genes associated with the RAS/MAPK cell signalling pathway. These mutations lead to dysregulation of cell division and differentiation.
Approximately 75% of patients with Noonan syndrome with multiple lentigines carry mutations in the PTPN11 gene (protein-tyrosine phosphatase, nonreceptor type 11). Ten percent have mutations in the RAF1 gene. In rare cases, mutations in BRAF and MAP2K1 genes are implicated.
Noonan syndrome with multiple lentigines is inherited in an autosomal dominant manner, which means that if one parent is affected there is a 50% chance that each child will be affected. About 70% of cases have a family history. The remainder are sporadic cases occurring from new mutations.
The signs and symptoms experienced by people with Noonan syndrome with multiple lentigines vary greatly. Some patients may have a partial form of the syndrome and suffer mild symptoms while others with the full syndrome are more severely affected.
Diagnosis based on clinical features. Noonan syndrome with multiple lentigines should be suspected in patients who demonstrate one or more of the following cardinal features:
Proposed minimum criteria are:
Diagnosis may be based on molecular genetic testing. Single gene or multi-gene panels can be used to identify mutations.
A team of specialist doctors including a cardiologist, endocrinologist, orthopaedist and dermatologist should manage Noonan syndrome with multiple lentigines.
If necessary, isolated lentigines can be removed through the use of chemical peels, cryotherapy, laser treatments or surgical excision. For some patients, treatment with topical retinoids and hydroquinone cream may be helpful.