Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Ahmed Tahoun, Dermatologist, Menoufia University, Egypt (2023)
Previous contributors: Vanessa Ngan, Staff Writer (2006)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Causes - phototoxic contact dermatitis Causes - photoallergic contact dermatitis Clinical features Clinical features - phototoxic contact dermatitis Clinical features - photoallergic contact dermatitis Variation in skin types Complications Diagnosis Differential diagnoses Treatment Prevention Outcome
Photocontact dermatitis (PCD) is an inflammatory skin reaction that occurs when ultraviolet or visible light interacts with a topically applied or systemically taken photoreactive substance on or in the skin.
PCD can be classified into two types:
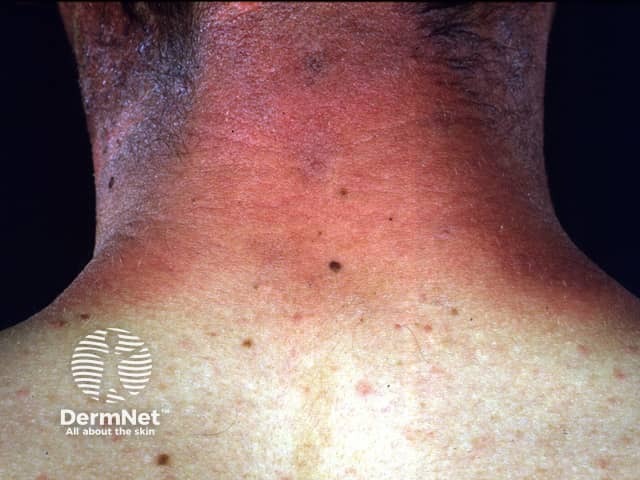
Photoallergic contact dermatitis due to a chemical sunscreen
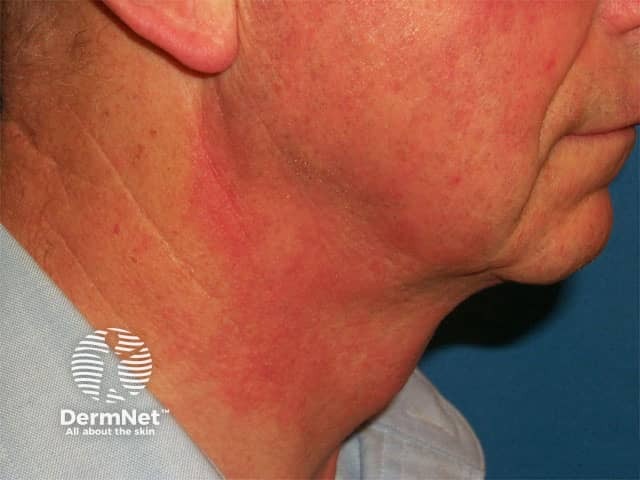
Photoallergic contact dermatitis due to a fragrance in an aftershave
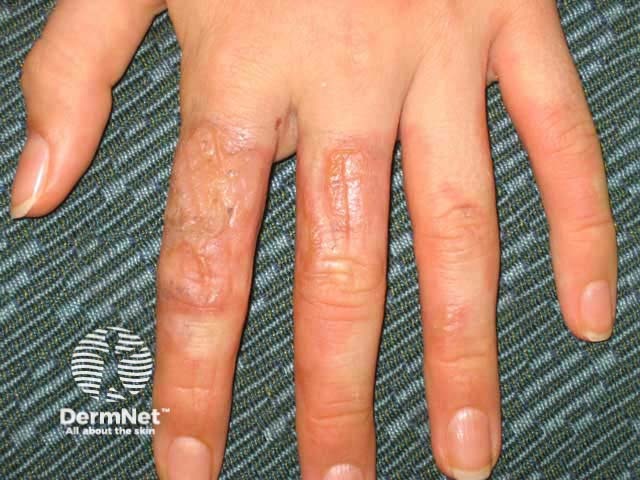
Phototoxic contact dermatitis due to accidental lime juice contact on a sunny day

Phototoxic contact dermatitis due to the ingestion of celery seeds
Anyone, male or female, can get PCD.
Prevalence in the general population:
Occupational risk factors include working outside (eg, gardeners, farmers, builders, carpenters, roofers, and road workers) and working with plants that contain psoralens (eg, celery harvesters and canners).
PCD can also occur as a reaction to sunscreen use, fragrances and perfumes, medications, cosmetics, and other substances.
Photocontact dermatitis (PCD) results from the interaction of two factors:
Phototoxic contact dermatitis (PTCD) is a non-immunological reaction, thought to develop as a result of free radicals produced by phototoxic reactions directly harming the skin. Anyone exposed to sufficient phototoxic agents and light of an appropriate wavelength can develop phototoxic dermatitis.
Common phototoxic agents include:
PACD is an immunological reaction — specifically, a delayed-type hypersensitivity reaction that occurs against a light-activated photosensitising agent. When this agent is applied to the skin and then exposed to UV rays, in some individuals a small portion of the substance (hapten) binds to a protein in the skin to form an antigen. This antigen is then taken up by an antigen-presenting cell and transported to the nearby lymphocytes where specific T-cells are activated. If the sensitised patient uses the same chemical again, sun exposure can cause an eczematous reaction.
Commonly encountered photoallergic agents (photoallergens) include:
In both types of photocontact dermatitis, skin lesions are generally confined to sun-exposed sites: the face, neck, V-shaped area of the chest, and dorsal upper extremities.
The following areas are usually spared: the upper eyelids, the area below the chin, the area behind the ears, and the skin folds of the neck.
PTCD looks like an exaggerated sunburn and is limited to sun-exposed sites. Patients may report pain and a burning sensation. Blisters and distal onycholysis are sometimes seen. Postinflammatory hyperpigmentation frequently follows PTCD.
Phytophotodermatitis, a type of plant dermatitis, is a phototoxic reaction that develops after psoralen-containing plant sap comes in contact with the skin, which is subsequently exposed to ultraviolet A radiation (UVA). The rash manifests as painful non-itchy erythematous linear streaks and blisters. Phytophotodermatitis usually resolves leaving postinflammatory hyperpigmentation.
PACD looks like allergic contact dermatitis. The skin lesions are itchy and confined mainly to sun-exposed skin areas, although sometimes may involve non-exposed sites. With frequent exposure to the allergen, the skin lesions may become lichenified.
Patients with darker skin types are more likely to have postinflammatory hyperpigmentation.
Identify and avoid the causative photoreactive agents.
PCD gradually improves if the photoreactive agent is avoided. While photoallergic reactions can continue up to three weeks, phototoxic reactions often fade within a week.