Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003; Updated: Katrina Tan, Medical Student, Monash University, Melbourne, Australia; Dr Martin Keefe, Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. August 2021
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
Leukoderma, also called achromoderma, is a clinical sign describing a localised area of white depigmented skin due to total loss of epidermal melanin. It is not a diagnosis in itself and has many causes. Leukoderma must be distinguished from hypopigmentation, which is pallor due to reduced pigmentation.
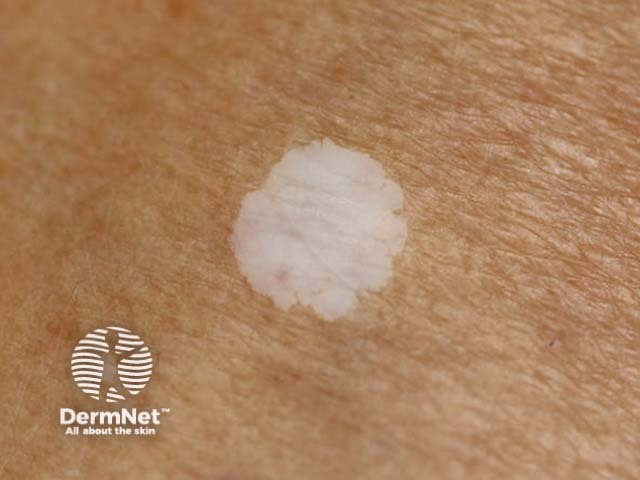
Idiopathic guttate hypomelanosis
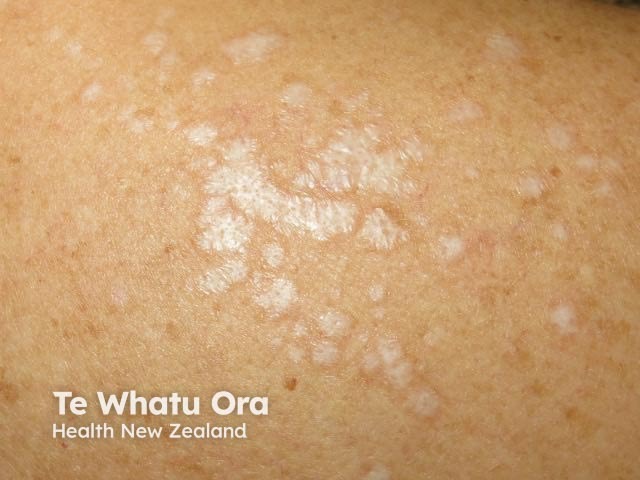
Lichen sclerosus
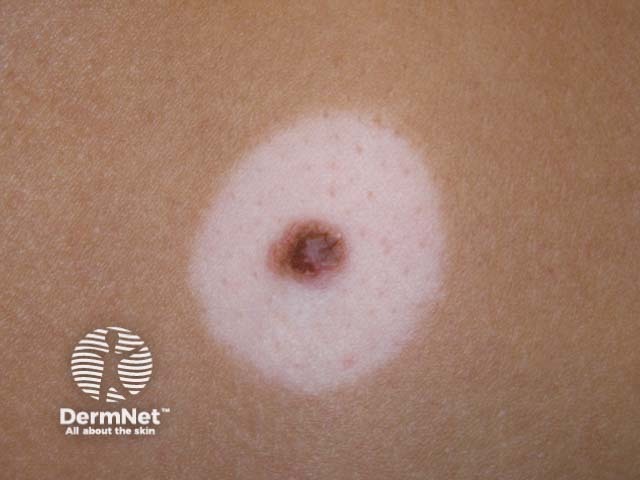
Halo naevus
Leukoderma can be seen in people of all ages and races, and both sexes. There may appear to be a female predominance due to cosmetic concerns. Leukoderma is more apparent in skin of colour than in ethnic white skin, but prevalence rates are difficult to determine.
Leukoderma is the visible result of loss of epidermal melanin. Melanocytes may be absent or present but unable to synthesise melanin or transfer it to the keratinocytes. There are many causes of leukoderma — some are listed below.
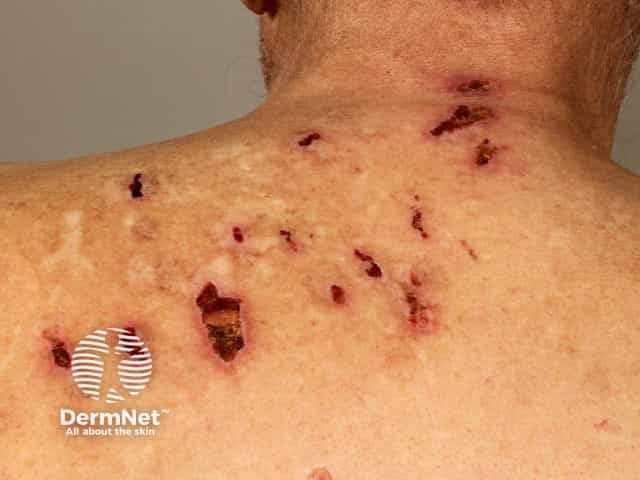
Leukoderma and compulsive picking
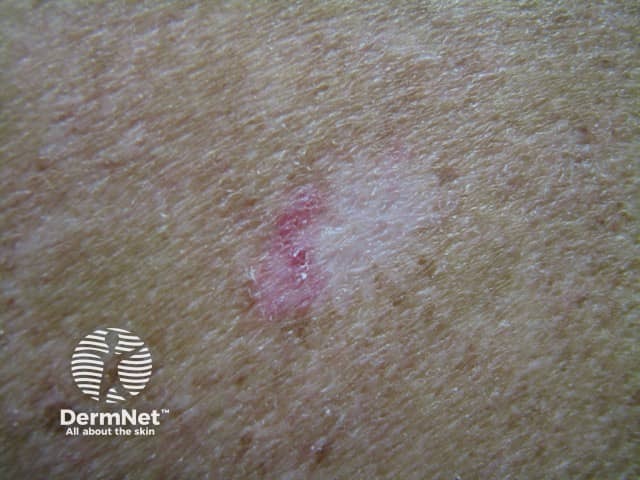
Cryotherapy-induced leukoderma with recurrent BCC
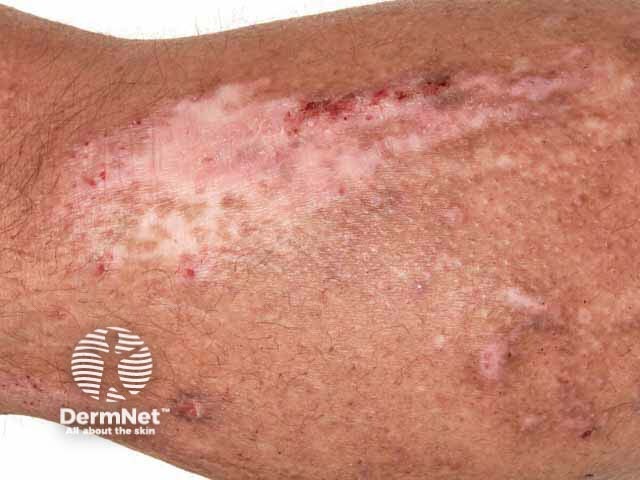
Leukoderma in lichenified atopic dermatitis
Leukoderma presents as a well-demarcated macule or patch of white skin with a normal surface texture or epidermal atrophy. The white patch itself is asymptomatic but there may be clinical features of the underlying condition.
Contact leukoderma is initially localised to the site of contact, with subsequent multiple small confetti-like white spots spreading beyond the known contact area.
Guttate leukoderma can be an early sign of Darier disease seen particularly in skin of colour. It often precedes the development of the typical keratotic papules and is distinct from post-inflammatory changes.
Melanoma-associated leukoderma can present as white areas of regression within the primary melanoma or the appearance of white patches distant from the melanoma.
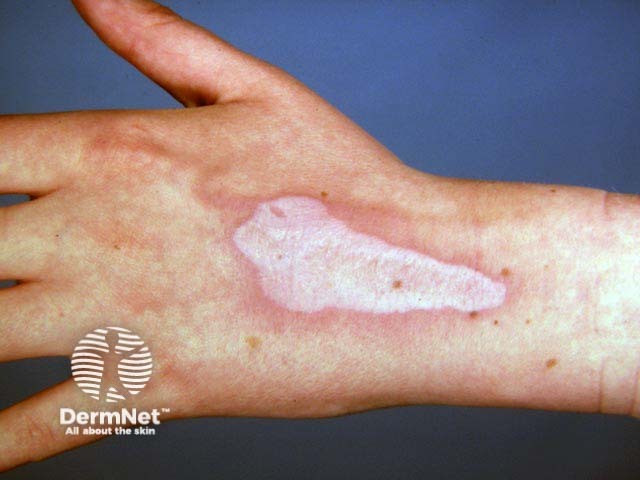
Chemical burn scar with leukoderma
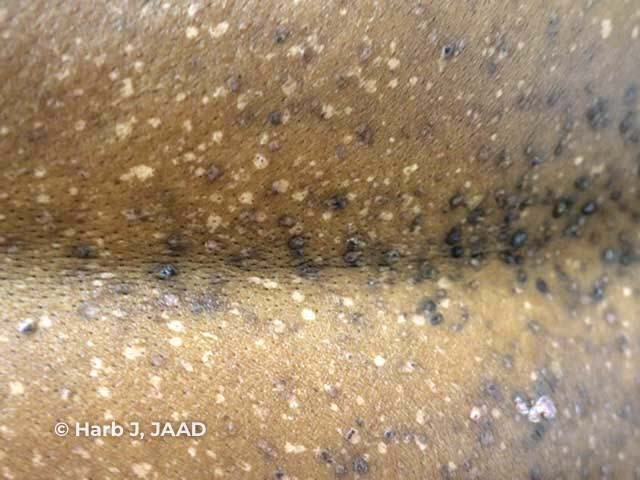
Guttate leukoderma in Darier disease
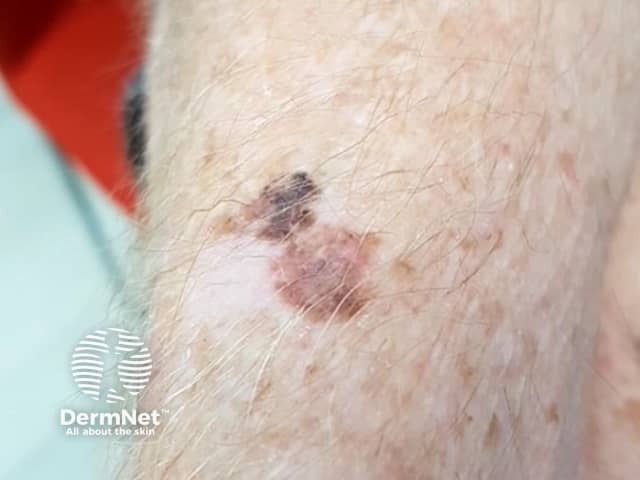
Melanoma-associated leukoderma
Image of Darier disease from: Harb JN, Motaparthi K. Clinicopathologic findings of guttate leukoderma in Darier disease: a helpful diagnostic feature. JAAD Case Rep. 2018;4(3):262–6.
Leukoderma is more obvious in racially pigmented or tanned skin compared to ethnic white skin.

Facial vitiligo is likely to have psychosocial effects
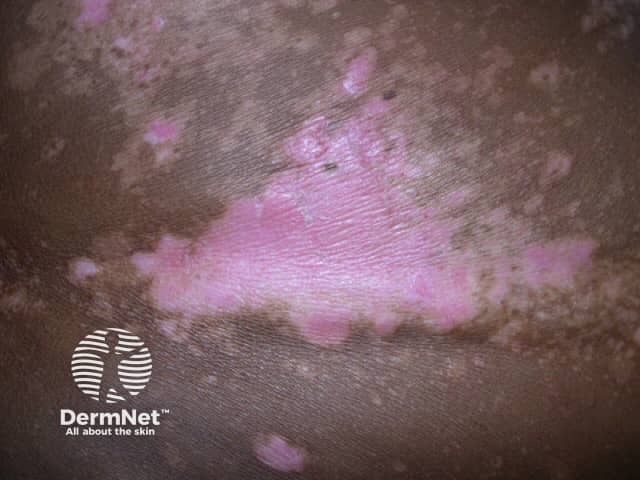
Sunburn in vitiligo
Leukoderma is a clinical diagnosis confirmed on Wood lamp examination.
Dermoscopy can be helpful in the diagnosis of some forms of leukoderma. [see Dermoscopy of vitiligo, Idiopathic guttate hypomelanosis dermoscopy]
Skin biopsy is not routinely required but can confirm the absence of melanocytes and/or melanin in the epidermis. A biopsy may be taken to determine an associated underlying skin condition.
Leukoderma may recover slowly if the cause can be avoided, such as cessation of a drug or chemical exposure, or treated such as inflammatory dermatoses. Leukoderma of the congenital patterned form or due to scarring is likely to be stable and persistent.