Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2004; Updated: Willian Hao Syuen Ng, Medical Student, University of Newcastle, Newcastle, Australia; Dr Paul Chee, Dermatologist and Director of Dermatology, John Hunter Hospital and Royal Newcastle Centre, Newcastle, Australia. Copy edited by Gus Mitchell. June 2021
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Dermoscopy
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Idiopathic guttate hypomelanosis is a benign, common, acquired form of leukoderma that presents as small flat pale or white spots on sun-exposed limbs.
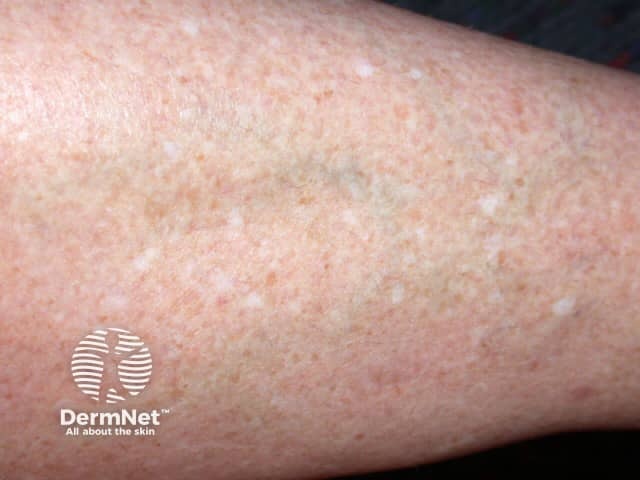
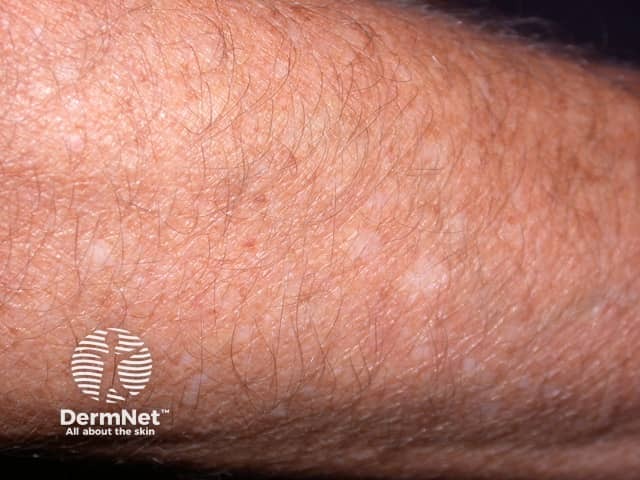

Idiopathic guttate hypomelanosis can affect both sexes, all races, and all skin phototypes. Women and patients with skin of colour are most likely to present for medical attention.
Idiopathic guttate hypomelanosis becomes more common with age, affecting <50% in the fourth decade (31–40 years), 50–80% of people over 40 years of age, and >90% in the ninth decade (81–90 years). It has been reported uncommonly in children and teens. Familial cases are common.
Although not fully understood, the aetiopathogenesis of idiopathic guttate hypomelanosis is probably multifactorial:
Abnormal keratinocyte phagocytosis has been demonstrated resulting in reduced transfer of melanin from melanocytes.
Idiopathic guttate hypomelanosis typically presents as smooth pale (hypopigmented) or white (depigmented) macules 2–5mm (range up to 1.5cm) in diameter most commonly on the sun-exposed aspects of the forearms, shins, and V of chest. Lesions are usually multiple and asymptomatic.
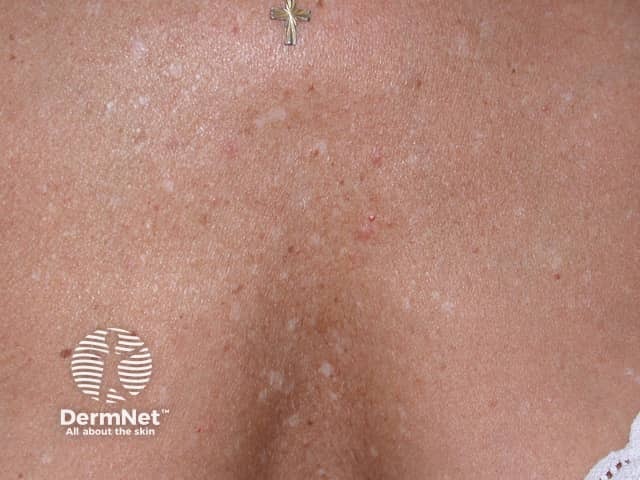
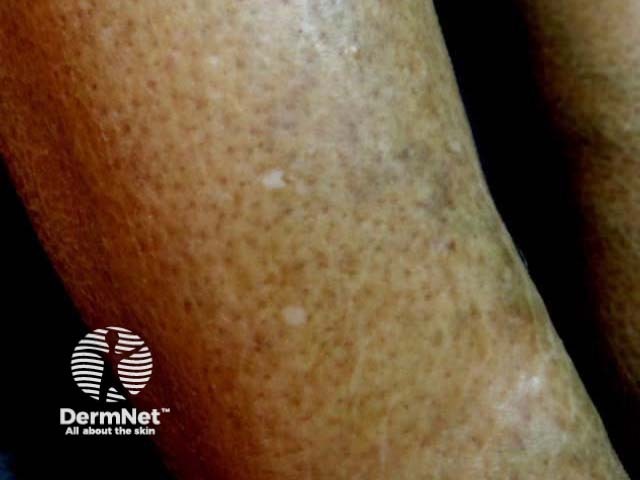
Porcelain-white patch extending peripherally
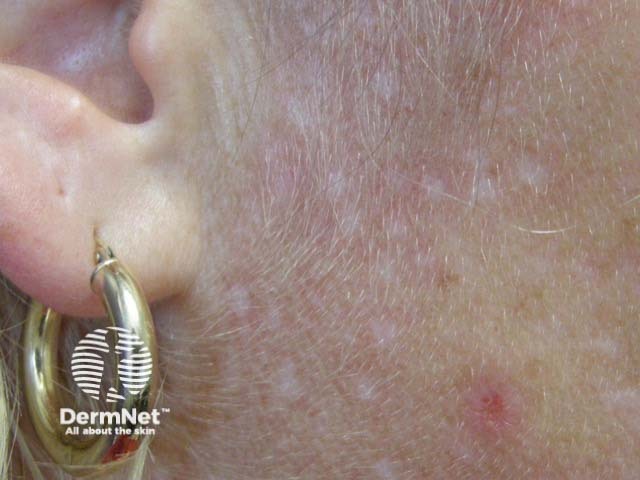
Three morphological variants have been described:
Wood lamp examination emphasises the loss of pigment.
Idiopathic guttate hypomelanosis is more obvious in skin of colour.
For a more detailed description and images see Idiopathic guttate hypomelanosis dermoscopy
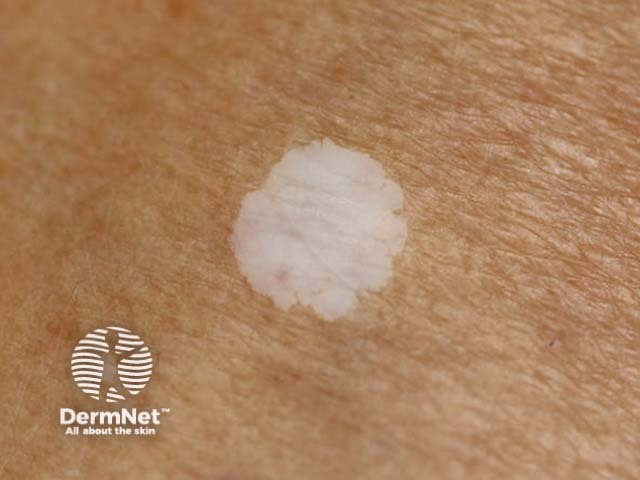
Macroscopic view
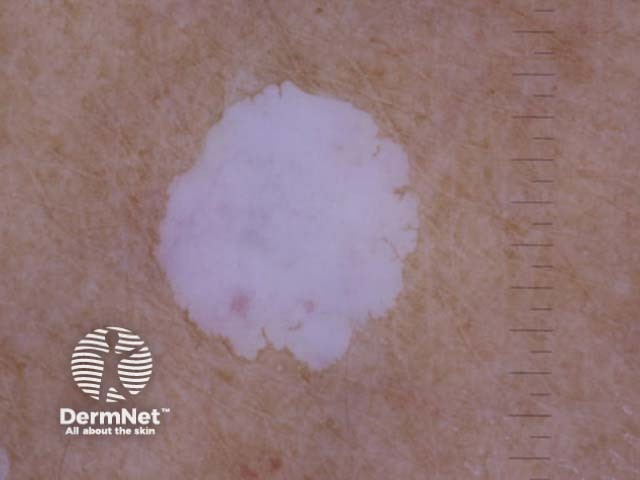
Nonpolarised dermoscopy view
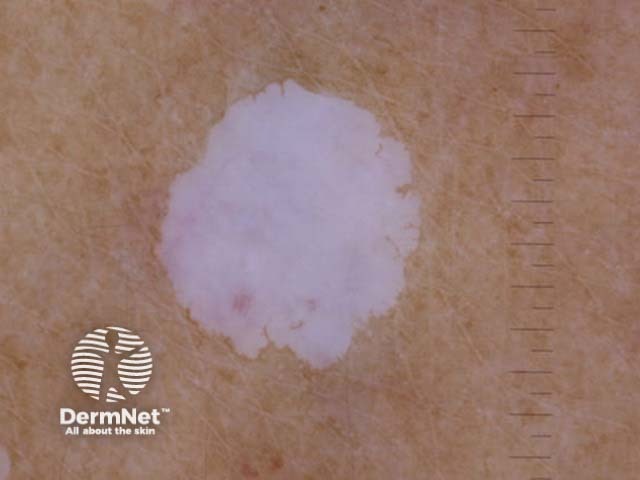
Polarised dermoscopy view
Idiopathic guttate hypomelanosis is a benign condition of cosmetic significance. It can impact quality of life particularly in skin of colour.
Idiopathic guttate hypomelanosis is usually a clinical diagnosis.
Skin biopsy may be performed to rule out other conditions and histology is specific:
Idiopathic guttate hypomelanosis usually does not require treatment apart from reassurance as to the benign nature of the condition.
Sun protection is recommended.
Treatment options:
Idiopathic guttate hypomelanosis does not require treatment due to its benign nature.
It does not spontaneously repigment. With age, lesions may slowly enlarge and increase in number.