Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Reactions Autoimmune/autoinflammatory
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. June 2017.
Introduction - vitiligo Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
Vitiligo is a common pigmentation disorder in which the pigment cells (melanocytes) are destroyed by an autoimmune process. The result is the appearance of slowly increasing white patches, without any change in the skin texture. The white patches of skin are prone to sunburn.
Drug-induced vitiligo is similar to the non-drug-induced form of vitiligo and is likely due to a similar autoimmune process. It is also called drug-induced leukoderma.
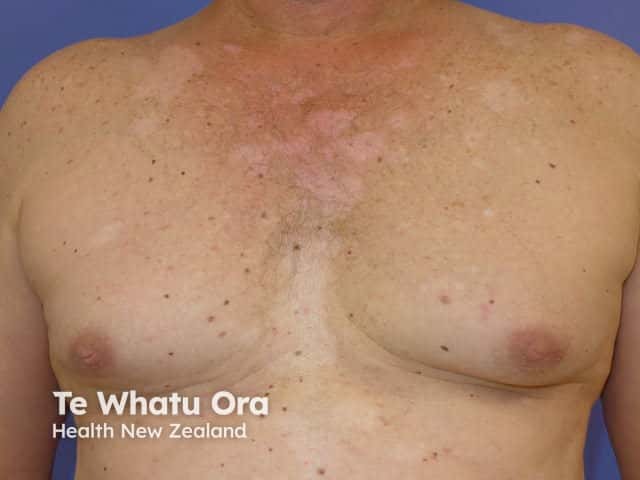
Induced by vemurafenib
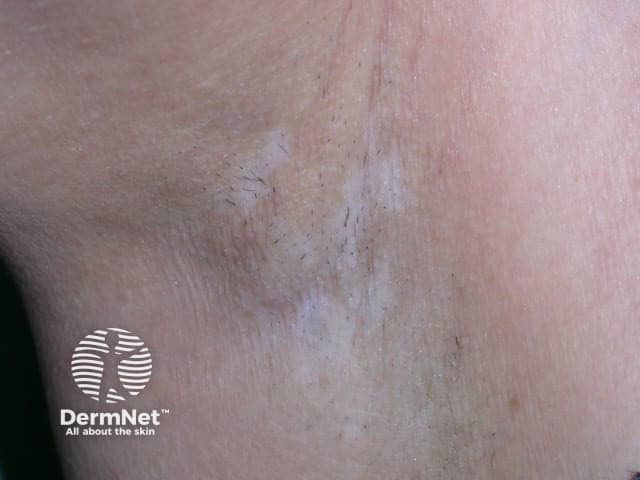
Induced by infliximab
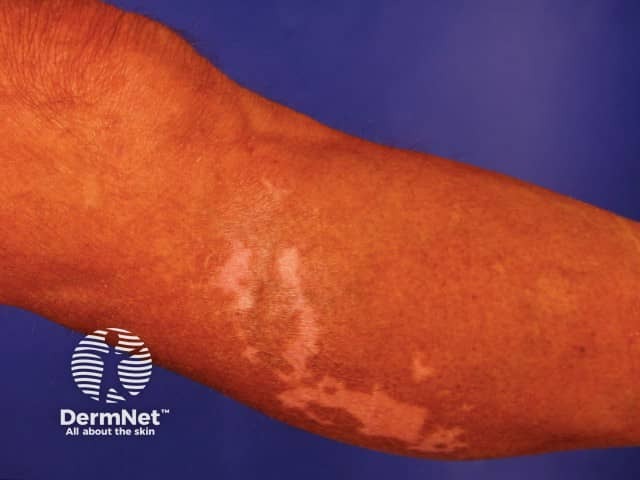
Induced by anticonvulsant
Drug-induced vitiligo has similar risk factors to those for non-drug-induced vitiligo. These risk factors include:
Affected individuals may also develop other autoimmune disorders — especially Addison disease, autoimmune thyroid disease (both hyperthyroidism and hypothyroidism), diabetes mellitus, pernicious anaemia and alopecia areata.
A previous history of vitiligo can also make a patient more vulnerable to a drug-induced extension of their pigment loss.
The most common causes of drug-induced vitiligo are immune-modulating, biologic or targeted medicines. These medicines include:
Rare cases of drug-induced vitiligo have also been reported from:
Note: phenols that cause localised contact leukoderma, such as monobenzyl ether of hydroquinone, paraphenylenediamine and rhododendrol, may also cause generalised vitiligo in rare cases.
The mechanism of drug-induced vitiligo is uncertain and there are currently autoimmune, neural and cytotoxic theories in relation to this.
Drug-induced vitiligo has similar features to non-drug-induced vitiligo, with the exception that it tends to have both a rapid onset and extension. Small confetti-like white macules are common in new body sites. Drug-induced vitiligo results in flat patches of depigmented skin with irregular but defined borders. The areas of the body most likely to be affected are the face, elbows and knees, the backs of hands, and the genitals.
Vitiligo is more visible in dark-skinned people, and it so often causes emotional stress or embarrassment, and reduces the affected individual’s quality of life.
The diagnosis of drug-induced vitiligo is based on the patient’s history and careful general skin examination. Investigations could include:
The causative drug is stopped, where possible. Treatment options for drug-induced vitiligo include:
Drug-induced vitiligo usually resolves when the offending drug is discontinued, but the time it takes to happen can vary greatly. Vitiligo is difficult to treat.