Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Eugene Tan, Medical Registrar, Waikato District Health Board, Hamilton, New Zealand, 2007.
Introduction
Skin rashes and chemotherapy
Acral erythema
Alopecia
Photosensitivity
Recall reactions
Acneform (pimple-like) eruptions
Skin necrosis
Neutrophilic eccrine hidradenitis
Eccrine squamous metaplasia
Hyperpigmentation
Nail changes
Mucositis
Sclerotic dermal reactions
Vascular phenomenon
Xerosis
Other reactions
Each year, 10.9 million people worldwide are diagnosed with cancer, and this incidence is rising. This increase reflects the world's growing population and the fact that people are living longer. Chemotherapy is a crucial component to all cancer management, and with this rising cancer burden, doctors and patients alike will see an increasing incidence of chemotherapy-related skin toxicity.
Acral erythema is also known as palmoplantar erythrodysesthesia (PPE) or hand-foot syndrome. It manifests as painful erythema (redness of the skin) of the palms and soles, with or without bullae (large blisters). Swelling, tingling, hyperkeratosis, fissuring and ulceration may also occur. These symptoms can be preceded by dysaesthesia (altered sensation of the skin). The pain from this rash may be so severe that daily activities are limited.
If recognised early, the usual course of acral erythema is desquamation (shedding of the outer layers of the skin) followed by re-epithelialization (re-growth of the outer layers of the skin). The risk increases with each dose of chemotherapy.
The exact mechanism is unknown, but it is postulated that the skin of the hands and feet favour a higher level of certain chemotherapy drugs which causes direct toxicity to the skin cells.
Toxic erythema of chemotherapy is a similar reaction extending to involve other sites, particularly intertriginous sites such as axillae and groin, and the knees.
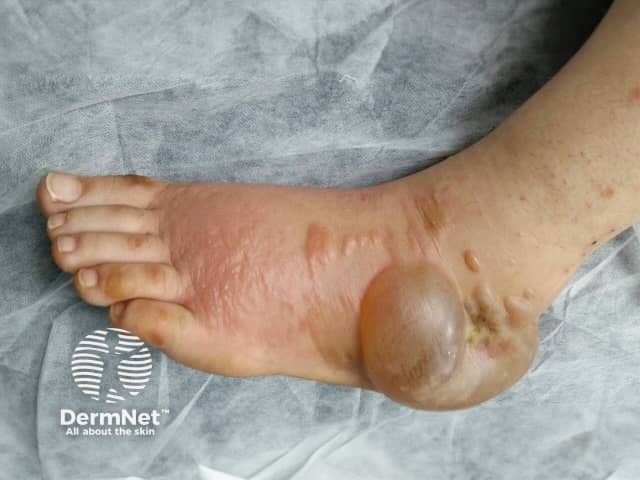
Hand-foot syndrome due to sorafenib
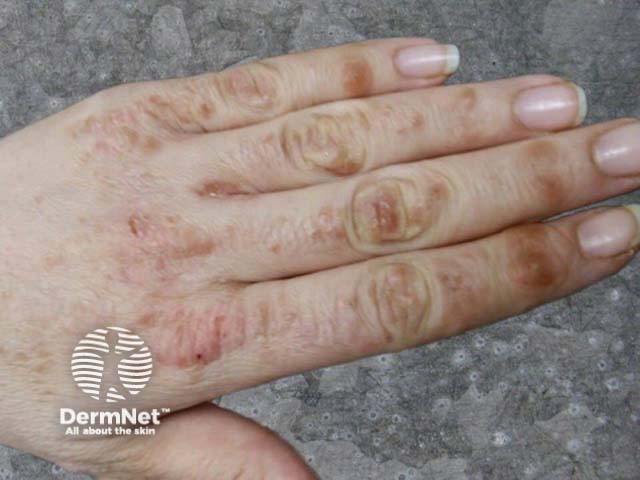
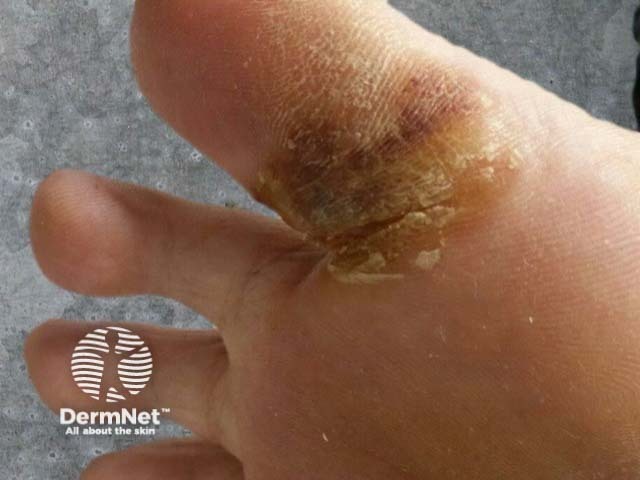
The most associated drugs include:
Often stopping or reducing the dose of the chemotherapy drug will result in regression of acral erythema over about 14–28 days. Supportive care may include wound dressings, analgesia (pain relief) and cold compresses.
Alopecia (hair loss) is the most common side effect of cancer treatment and often is the most distressing to the patient's self-image. It occurs 7-10 days after treatment and continues to progress over 2-3 months.
There are two main ways chemotherapy drugs cause alopecia:
Alopecia is often temporary and resolves after treatment is stopped but some chemotherapy drugs such as busulphan and cyclophosphamide can cause permanent hair loss.
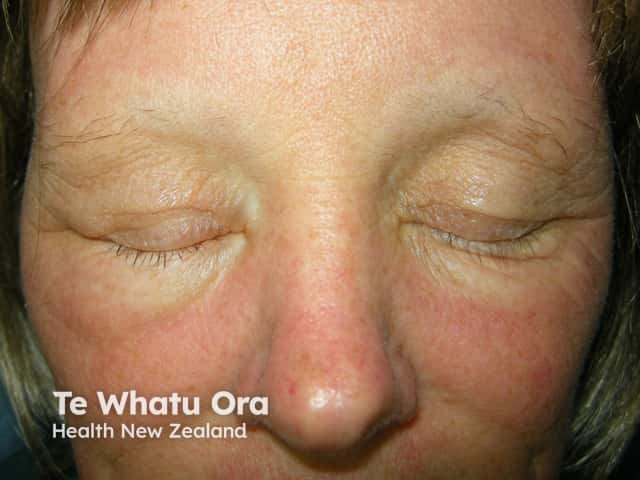
Anagen effluvium: loss of eyebrows from chemotherapy
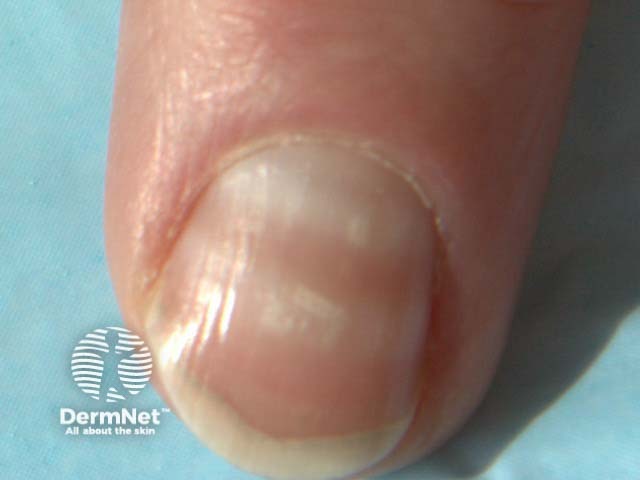
Striate leukonychia during chemotherapy
Most chemotherapy drugs cause alopecia but the most common culprits are the following:
Several strategies have been tried to reduce alopecia such as:
Unfortunately, none have consistently been shown to be effective. It is important to advise patients of this potential side effect and to provide a wig.
Epidermal growth factor receptor inhibitor (EGFR) treatment has been reported to cause slowing of the growth of hair, brittle hair and abnormally thick hair.
Certain chemotherapy drugs result in photosensitivity (increased sensitivity to sunlight) causing sunburn with minimal sun exposure.
The chemotherapy drugs which most commonly cause this are:
Patients should be advised of this potential side effect of photosensitivity and to protect themselves from the sun. This involves the use of sunscreen and protective clothing.
The term recall reaction refers to erythema (redness of the skin) in areas of previously quiescent sunburn or radiotherapy. The exposure to the sun or radiotherapy may have been weeks to months ago and the skin may have fully recovered until the patient was given chemotherapy.
The actual mechanism is not fully understood but it has been postulated to occur as a result of the recovering keratinocytes (skin cells) being damaged by the chemotherapy drugs, as these cells are the ones which are most rapidly dividing and regenerating.
The most common drugs which can cause this are:
Treatment involves minimising exposure to the sun, good wound care. There is possibly a role for topical steroid creams to reduce the inflammation.
Also known as folliculitis, an acneform reaction begins as facial erythema followed by papules (small bumps) and pustules (small pockets of pus) over the face and upper trunk. Unlike true acne, the pustules are sterile (they contain no bacteria).
Actinomycin D is the most common cause. Other drugs may also cause folliculitis, particularly the epidermal growth factor receptor (EGFR) inhibitors such as gefitinib and cetuximab.
Oral tetracycline antibiotics (e.g. doxycycline) and topical antibiotics can help. Even though bacteria do not appear to be involved in the acneform eruptions, these antibiotics have an anti-inflammatory effect over and above their anti-bacterial properties. Topical retinoids and benzoyl peroxide may also help.
Skin necrosis is the term used to describe dead skin cells, which blacken and peel off. Most chemotherapy drugs are toxic when exposed to the skin. Drugs that are meant to be delivered into veins and arteries may leak into the subcutaneous tissue (extravasation).
There are two types of skin necrosis reaction:
Most chemotherapy drugs are irritants if they extravasate. Doxorubicin is the most vesicant and can cause necrosis, ulceration and thrombosis (blood clots).
Local wound care and the use of cold packs or heat packs can help with wound healing. When vesicants like doxorubicin leak into the skin, early plastic surgical advice may be required due to the expected death of extensive areas of skin.
Neutrophilic eccrine hidradenitis is characterised by tender red papules, plaques or nodules on the trunk, face and ears. The diagnosis of this condition relies on skin biopsy and analysing the histological (microscopic) changes. Neutrophils (a type of white cell) are seen surrounding eccrine (sweat) glands.
The cause is thought to be the high concentrations of chemotherapy drugs secreted into the sweat glands.
The most commonly implicated agents are:
Neutrophilic eccrine hidradenitis often heals without treatment within days to weeks. Appropriate management involves performing a skin biopsy to help establish the diagnosis. Supportive treatment such as systemic steroids, non-steroidal analgesics and dapsone helps to shorten the duration of the rash and relieve pain.
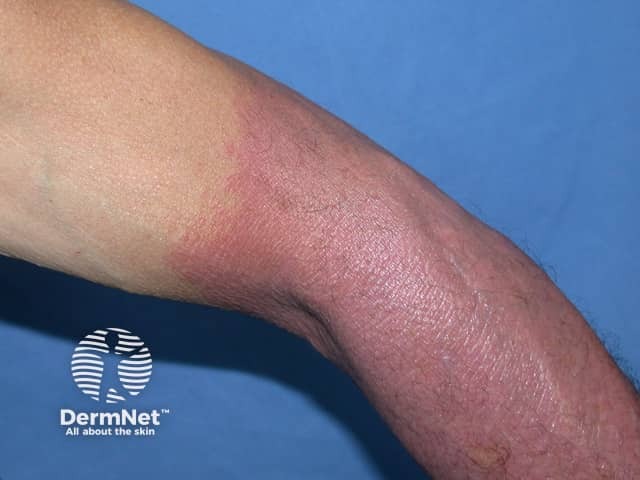
Drug-induced photosensitivity
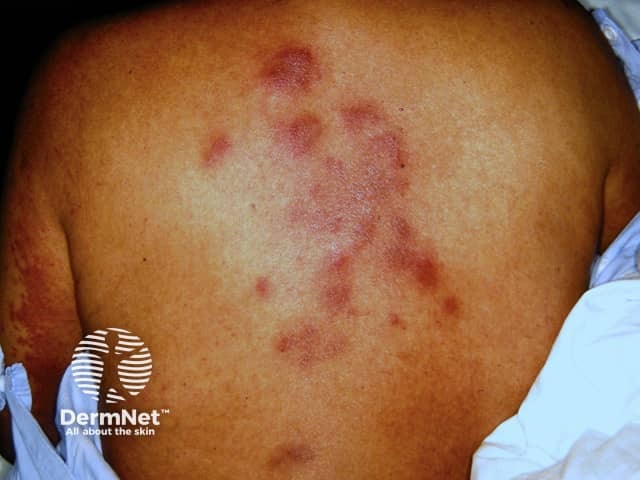
Neutrophilic eccrine hidradenitis
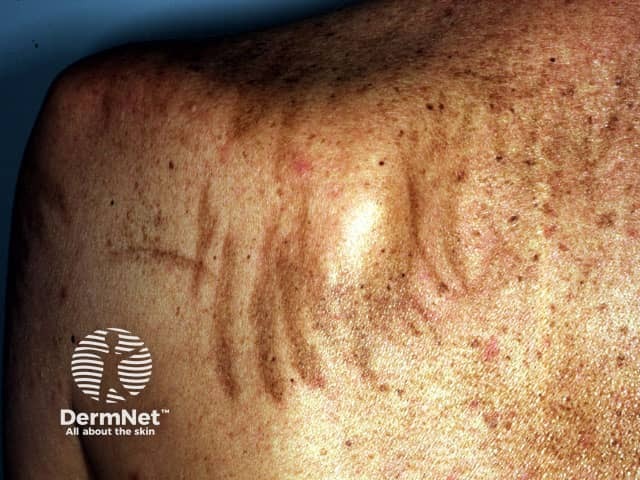
Pigmented streaks caused by bleomycin
Eccrine squamous metaplasia is a rare skin reaction. It is also known as syringometaplasia and affects the upper part of the eccrine sweat duct. It presents as non-specific red plaques or a papular, crusted eruption.
A distinctive subtype affecting armpits, groin and the sides of the neck has been described.
Three large groups of chemotherapy drugs have been known to cause this skin reaction.
The treatment of eccrine squamous metaplasia is similar to that for neutrophilic eccrine hidradenitis. Spontaneous resolution generally occurs. It may recur in about 50% on reintroducing chemotherapy with the same drugs.
The most unique pattern of hyperpigmentation is the flagellate hyperpigmentation caused by bleomycin. This reaction occurs as dark brown linear streaks about 10cm in length and crisscrossing one another in a pattern resembling a flagellum (whip-like structure of certain bacteria that assists them in moving).
Various mechanisms have been reported to explain the cause of this hyperpigmentation. The most well-accepted hypothesis is that bleomycin induces pruritus (itching) of the trunk causing the patient to scratch. The action of scratching causes local accumulation of bleomycin into the skin.
Fluorouracil, vinorelbine and daunorubicin can cause hyperpigmentation of the skin, nails and oral mucosa. Although not characteristically flagellate in nature, pigmentation caused by these agents can follow the distribution of veins (called serpentine supravenous hyperpigmentation) or may simply be patchy and macular (flat nonspecific colour change).
Oral antihistamines may be helpful if there is marked itching. Topical bleaching agents such as hydroquinone can decrease melanin production and assist in the clearing of areas of pigmentation. However, when the chemotherapy drug is stopped, the pigmentation may be expected to slowly disappear without treatment.
There are several changes that can occur in the nail (nail diseases). This is due to the direct toxicity of the chemotherapy drug to the nail plate.
Two groups of chemotherapy drugs are particularly prone to cause nail changes:
Nail changes may also be seen with hydroxyurea.
Paronychia has also been observed and they occur with an incidence of 10–15% with EGFR therapy and < 1% with capecitabine therapy. Although supportive therapy is the best form of treatment, there has been some success with the use of doxycycline. In its most severe form a pyogenic granuloma can occur.
Often nail changes disappear when the damaged nail is replaced by the growth of new nails. The optimal management may need to include pain killers as some of these nail changes can be exquisitely painful.
Mucositis refers to inflammation of mucosal surfaces. The lining of the mouth and the gastrointestinal tract are extremely susceptible to being damaged by chemotherapy drugs due to high cell regeneration and growth rate. Up to 80% of chemotherapy patients suffer from this complication.
The symptoms begin with burning and erythema of the mouth followed by erosions and ulcerations that are intensely painful. Although the signs in the mouth are most apparent, any part of the gastrointestinal tract may be involved so patients may also develop diarrhoea.
Almost all chemotherapy drugs have the potential to cause mucositis but agents that affect DNA synthesis and are S-phase specific (this is the synthesis phase of the cell cycle) cause the most mucositis.
Examples include:
Mucositis may rarely be life-threatening and when severe, may require the use of feeding tubes. The pain and discomfort from mucositis can greatly impact on the nutritional status of the patient.
Treatment of mucositis is supportive and aimed at symptom control.
Scar-like skin reactions that mimic morphoea or systemic sclerosis may accompany the use of bleomycin and docetaxel.
In some cases, these reactions have resolved after the drug has been stopped. The exact mechanism is unknown but it is postulated that these drugs increase the activity of fibroblasts in the skin.
Raynaud phenomenon is an exaggerated response of the blood vessels to cold temperature or emotional stress. The symptoms are that of sharply demarcated colour changes of the skin of the digits.
Vasculitis refers to inflammation of the vessel walls and as a result of this inflammation, there is a compromise to the lumen of the vessel causing tissue ischaemia and necrosis.
Vasculitis can present as livedo reticularis, ulceration and thromboembolism (blood clots).
Drugs reported to cause Raynaud's phenomenon or vasculitis include:
Correct diagnosis of vasculitis is important and a skin biopsy assists in diagnosis. The treatment of vasculitis involves stopping the offending drug and the use of high dose systemic corticosteroids.
Raynaud phenomenon often improves with discontinuation of the drug. Simple measures such as avoiding exposure to cold, hand warmers and the use of protective clothing are universally helpful. Medications that can be used include calcium channel blockers and ACE inhibitors which promote vasodilations (opening up) of blood vessels in the fingers.
Xerosis (dry skin) is commonly observed in patients receiving epidermal growth factor receptor EGFR) inhibitors. At times, the dry skin can be observed with concomitant greasy scales resembling seborrhoeic dermatitis. It is postulated that the EGFR inhibitors cause growth arrest of the keratinocytes (skin cells) and initiates terminal maturation. Mucosal surfaces of the skin such as the vagina, mouth and eyes may also be affected.
Like other drugs, chemotherapy medications may cause other adverse reactions, including: