Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Causes Clinical features Complications Diagnosis Treatment Outlook
Onchocerciasis is a chronic and progressive skin, eye, and neurological disease caused by Onchocerca volvulus, a filarial nematode (worm). The eye disease is often called river blindness.
Over 90% of cases of onchocerciasis occur in 31 countries in sub-Saharan Africa; the remainder are found in Latin America, and Yemen in the Arabian Peninsula. According to the WHO, onchocerciasis has been eradicated from Columbia, Ecuador, Guatemala, and Mexico but persists in the Amazon region of Brazil and Venezuela.
Of the 218 million people who live in endemic areas, at least 18 million are currently infested; 4 million have a skin disease, and 2 million are blind or visually impaired.
Initial infestation may occur in childhood and produce no symptoms for long periods. However the neurological manifestations mainly affect children.
Short-term travellers to endemic areas are at low risk of onchocerciasis, as multiple bites are required for infestation. Travellers who visit endemic areas for extended periods and live or work near blackfly habitats are at greatest risk of infection.
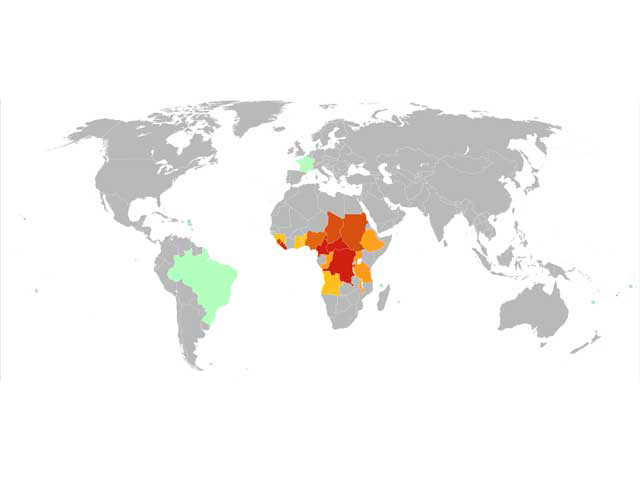
Distribution of onchocerciasis
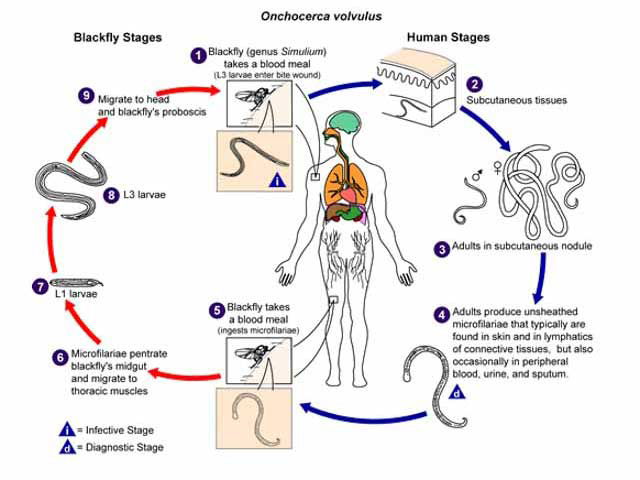
Lifecycle of onchocerciasis
Credit: Onchocerciasis map from Wikimedia
O. volvulus is transmitted to humans through the bite of a female blackfly (Simulium spp). Blackflies are found near fast-flowing rivers and streams in the inter-tropical zones, and bite during the day.
In humans, the adult worms live in nodules scattered under the skin. The female worm produces millions of larval worms (microfilariae). Microfilariae migrate through the lymphatic system under the skin and are ingested by blackflies during a blood meal. The larvae mature in the blackfly over the next two weeks. When the blackfly bites another human, the larvae enter through the wound, penetrate the tissues, and develop into adult worms.
A female worm can live for up to 15 years and produce hundreds of microfilariae each day. The microfilariae mature over 2 to 3 years, and their death releases symbiotic Wolbachia bacteria causing an inflammatory reaction in the skin and eye.
Years of exposure may lead to skin disfiguration and irreversible blindness.
Six skin disease patterns have been described. Two or more patterns may be present in a single patient, and the patterns may evolve and change over time.
Classification |
Skin features |
|
|---|---|---|
Acute papular onchodermatitis |
Widespread itchy eczema-like rash with multiple small itchy papules which progress to become vesicles and pustules. The face, trunk, and extremities are often affected. |
|
Chronic papular onchodermatitis |
Severely itchy rash with scattered flat-topped papules and areas of hyperpigmentation. The shoulders, buttocks, and extremities are typically affected. The most common pattern of skin disease. |
|
Lichenified onchodermatitis |
Thickened scaly and hyperpigmented itchy plaques. The lower extremities are commonly affected, and lymph nodes are often enlarged. |
|
Onchocercal atrophy |
Large areas of wrinkled thin, dry inelastic skin. Commonly affects buttocks and lower back. |
|
Onchocercal depigmentation |
Also called “leopard skin”. Areas of pigment loss (leukoderma), with islands of normally pigmented skin surrounding hair follicles. Often affects the shins in a symmetrical pattern and is not usually itchy. |
|
Palpable onchocercal nodules (oncocercoma) |
Subcutaneous lumps found over bony prominences contain the adult worms. The subcutaneous nodules range in size from a few millimetres to several centimetres, and each contains 2 to 4 adult worms that can reach a length of 80 cm. |
|
Other classic clinical presentations of onchocerciasis include:
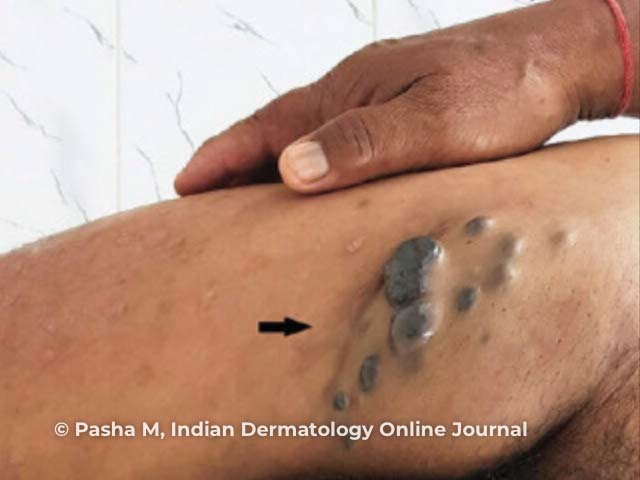
Hanging groin sign
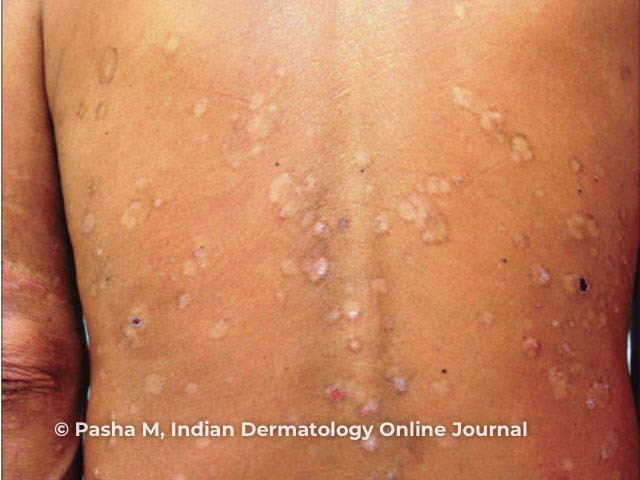
'Leopard skin' sign of cutaneous onchocerciasis
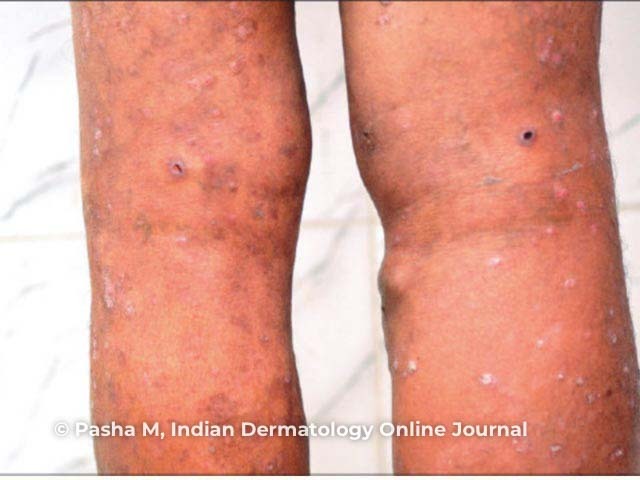
Onchodermatitis and limb oedema
Images from: Pasha MM, Patil CC, Tanuja M, Mitra D. A rare case of cutaneous onchocerciasis in north-east India, review of literature. Indian Dermatol Online J. 2020;11(4):600-3.
Inflammation and bleeding in an eye occurs when microfilariae in the cornea and/or back of the eye die. Early symptoms include itching, redness, pain, and photophobia. Repeated episodes of inflammation in the cornea cause a chronic keratitis and sclerosis affecting the clarity of the cornea. Blurring of vision, night blindness, glaucoma, visual field loss, and eventually blindness may develop in the affected eye.
Onchocerciasis has been successfully eradicated from some countries and programmes continue in many others. Treatment of established infestation is not curative, but aims to stop progression of disease. Prevention is the most cost-effective measure.