Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Systemic diseases Diagnosis and testing
Author: Hon A/Prof Amanda Oakley 2008/2016. Updated: Dr Axel Baumgartner, General Surgeon and Director of the Hanse-Klinik, Lübeck, Schleswig-Holstein, Germany. Copy edited by Gus Mitchell. October 2020.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Complications
Lipoedema is a chronic, usually progressive disorder in women defined by symmetrical accumulations of subcutaneous fatty tissue and orthostatic oedema. In most cases, the lower extremities are affected.
Lipoedema almost exclusively affects women. Due to oestrogen receptors in the white adipose tissue, oestrogen is considered to be a major factor. Similar changes to lipoedema can occur in men with hormone disorders such as testosterone deficiency in association with cirrhosis of the liver and renal failure, testicular cancer, and hypogonadism.
The pathogenesis of lipoedema is poorly understood; although hormones and inheritance are thought to play an important role.
An influence of hormones is assumed, with the possible onset of lipoedema during puberty and progression during pregnancy and menopause. In the majority of patients, the disease starts almost imperceptibly after puberty, but may also develop in other age groups, especially at times of hormonal changes such as during pregnancy or menopause.
Autosomal dominant inheritance is assumed with a higher prevalence of the disorder in family members.
The extent to which the adipokines or other messenger substances released in obese patients is still poorly understood. Lipoedema cells show reduced amounts of adiponectin and leptin. The disproportionate fat distribution is unresponsive to dieting or intensive exercise.
The latest cell biology studies show significant differences in the differentiation of the adipocytes (fat cells) in patients with lipoedema. They also report significantly increased protein expression of proinflammatory factors, which constitutes a promising approach for understanding lipoedema as a disorder.
Several factors are responsible for lipoedema, including:
In the early stages of lipoedema, the function of the lymphatic system is not affected, and removal of the lymphatic load may even be increased. A lymphoscintigraphic function test will generally not yield any abnormal findings. As the disease progresses, the lymphatic system is no longer able to completely remove the volume accumulating in the thighs and the lower legs in the evening. This is due to increased vessel permeability, in particular in conjunction with orthostatic hypertension, leading to high volume insufficiency. After years of exceeding the transport capacity of the lymphatic system, the system decompensates. Its functional reserves are depleted, leading to low volume insufficiency. The persistent protein accumulation in the interstitium causes non-bacterial inflammation, which in turn brings about lymphangiosclerosis and perilymphovascular fibrosis. This marks the onset of secondary lymphoedema.
The key finding on examination of patients with lipoedema is the symmetrical disproportion between the slim trunk and voluminous legs and arms. In many cases, patients exhibit column-shaped or lobular legs. The tops of the feet, toes, and hands do not show swelling, resulting in the cuffing sign at the ankle and wrist. Patients report tenderness, swelling, feelings of tightness and heaviness in the legs, and easy bruising.
A three-stage system was developed in Germany to classify lipoedema. The system describes only the morphology of the skin, and not the signs and symptoms.
Stage I: Smooth skin surface, homogeneous subcutis.
Stage II: Uneven skin surface, palpable subcutaneous nodules.
Stage III: Disfiguring lobules of fat, skin folds, grossly nodular tissue structure.
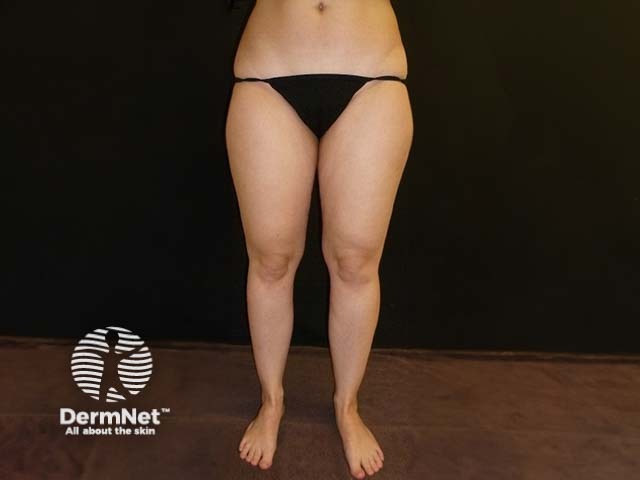
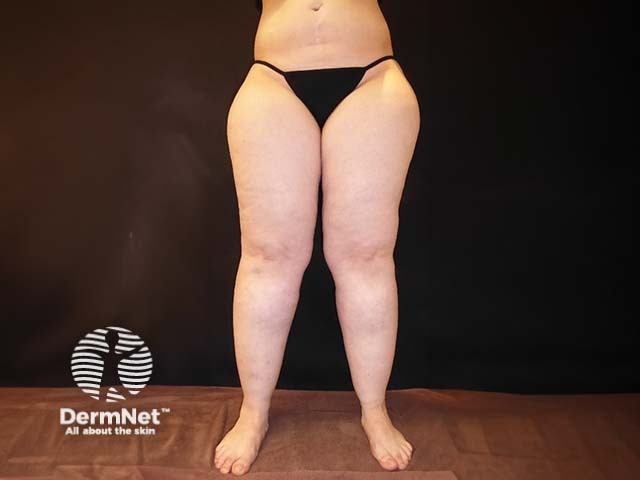
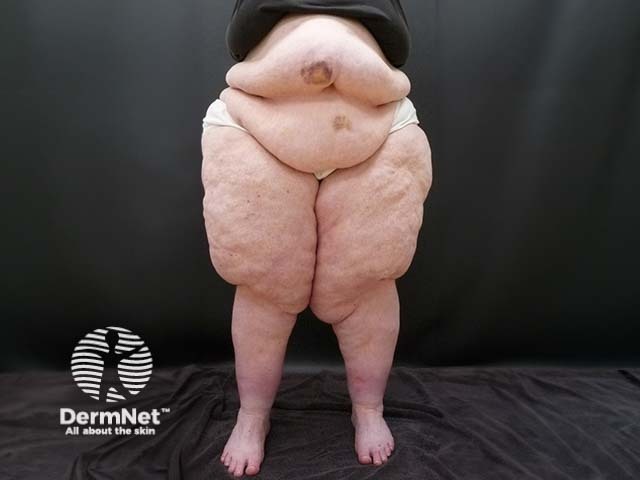
During palpation, depending on the stage, the nodular changes of the subcutaneous tissue are noticeable. The skin is also sensitive to touch and pressure, although this varies from person to person. The extent of orthostatic oedema may be tested by observing pretibial indentations (pitting oedema).
Most patients with lipoedema eventually develop a combination of diagnoses with varying degrees of phlebolymphostatic oedema, lymphoedema, and obesity.
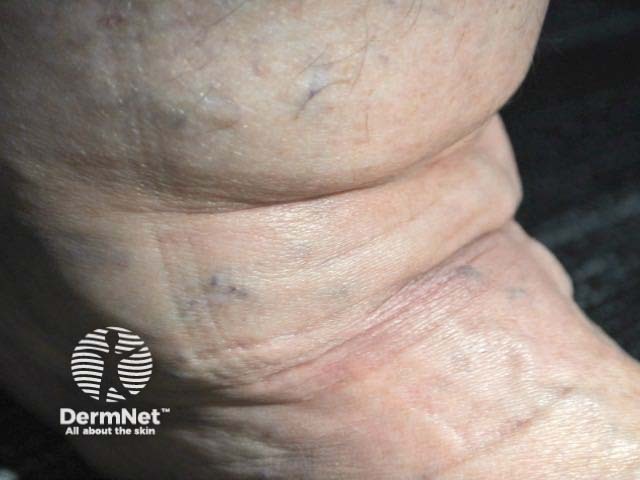
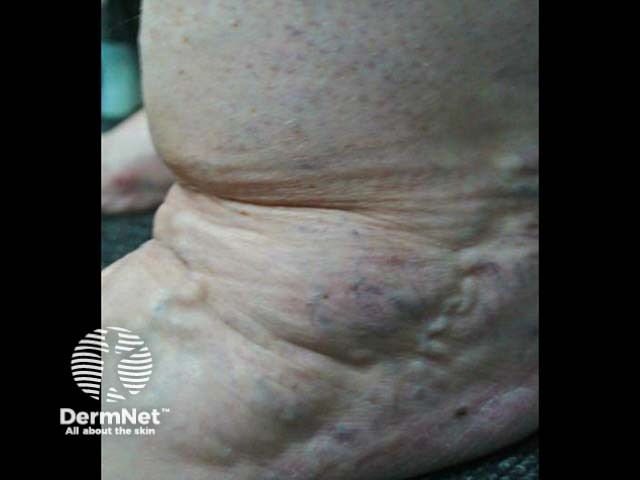
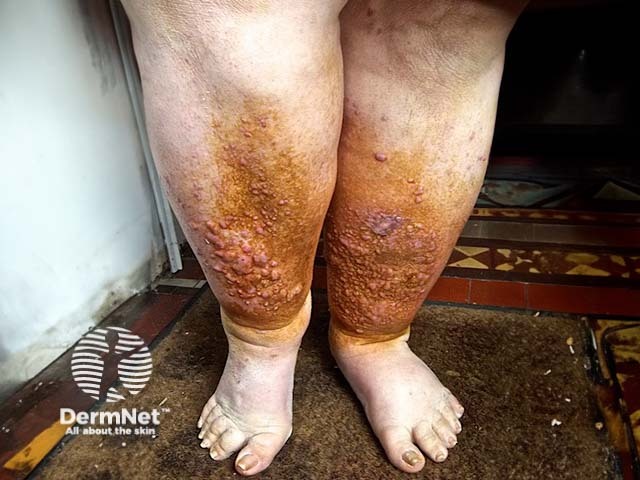
Lipoedema is primarily a clinical diagnosis.
A patient history must be taken eliciting information about the age of onset, signs and symptoms of swelling, sensitivity of the tissue to pressure, tendency to develop oedema when standing, weight gain, and stress. It is also important to ask about complications associated with increased volume, such as irritated skin, impaired gait, and the development of secondary lymphoedema.
General investigations can be carried out to identify reasons for the limb swelling and rule out any underlying medical disorder. Imaging is not usually necessary, but may include:
Important differential diagnoses of lipoedema are shown in Table 1 and Table 2.
Table 1: Typical clinical signs used to differentiate lipoedema, lipohypertrophy, obesity, and lymphoedema
Lipoedema |
Lipohypertrophy |
Obesity |
Lymphoedema |
|
Increased fat tissue |
+++ |
+++ |
+++ |
(+) |
Disproportion |
+++ |
+++ |
(+) |
|
Oedema* |
+++ |
Ø |
(+) |
+++ |
Pain on pressure |
+++ |
Ø |
Ø |
Ø |
Easy bruising |
+++ |
(+) |
Ø |
Ø |
Symbols: + to +++; (+) Ø not present
*The severity of oedema is variable and depends on prior therapy and the stage of disease.
Table 2: Additional differential diagnoses including treatment options.
Diagnosis |
Symptoms/Signs |
Treatment options |
Lipoedema |
Symmetric, predominantly affecting the limbs, disproportionate pain |
Compression |
Lymphoedema |
Oedema, typically including feet/hands |
MLD |
Lipoedema with secondary lymphoedema |
Symmetric, predominantly affecting the limbs, disproportionate pain |
MLD |
Lipoedema with concomitant obesity |
Combined symptoms of lipoedema and obesity, see above and below |
Weight reduction |
Phleboedema |
Oedema of the legs/arms |
Compression |
Lipohypertrophy |
Localised lipohypertrophy |
Liposuction |
Obesity |
Generalised lipohypertrophy |
Weight reduction |
Obesity with secondary oedema (obesity-related oedema) |
Generalised lipohypertrophy with secondary oedema |
Weight reduction |
Obesity with fibromyalgia |
Generalised lipohypertrophy and pain |
Weight reduction |
Lipomatosis |
Benign symmetric lipomatosis, particularly type III (pelvic region) |
Liposuction |
Myxoedema |
Doughy oedema |
Treatment of thyroid dysfunction |
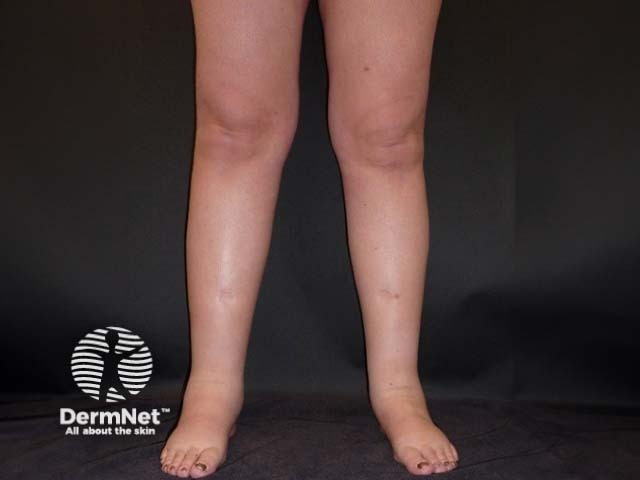
Primary lymphoedema
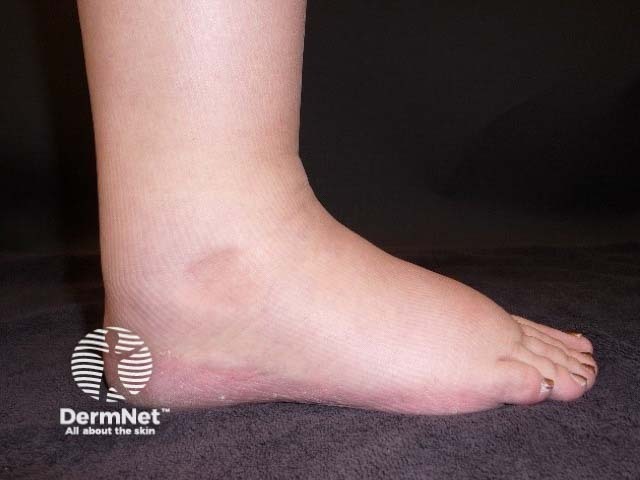
Lipoedema is a chronic progressive disorder. For many of those affected the symptoms deteriorate during the course of their lives. It persists lifelong and progresses gradually.
Mobility is restricted due to the proliferation of fatty tissue on the inner thighs and knees, which causes the legs to take on a knock knee position. The inability to exercise can result in secondary obesity.
Skin irritation and intertrigo can develop in the skin folds such as the groin and between the thighs.
The combination of increasing cosmetic and mechanical impairment and other complaints result in considerable emotional strain that can lead to social withdrawal and compromised quality of life.
See also Therapy for lipoedema.