Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. 1997/2014. Updated: Dr Brent J Doolan, Dermatology Research Fellow, The Skin Hospital, Sydney NSW, Australia. Dr Monisha Gupta, Dermatologist, The Skin Hospital, Sydney NSW, Australia. Copy edited by Gus Mitchell. October 2020. Minor update December 2025.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Melasma is a common acquired skin disorder that presents as a bilateral, blotchy, brownish facial pigmentation.
This form of facial pigmentation was previously called chloasma, but as this derives from the Greek meaning ‘to become green’, the term melasma (brown skin) is preferred. It was also known as the ‘mask of pregnancy’.
Melasma is more common in women than in men, with an onset typically between the ages of 20 and 40 years. Melasma is most common in people who tan easily or have naturally brown skin (Fitzpatrick skin phototypes III, IV). It is less common in people with fair skin (Fitzpatrick types I, II) or black skin (Fitzpatrick types V, VI).
The cause of melasma is complex; it has been proposed to be a photoageing disorder in genetically predisposed individuals. The pigmentation ultimately results from the overproduction of melanin by melanocytes (pigment cells); either taken up by keratinocytes (epidermal melanosis) and/or deposited in the dermis (dermal melanosis, melanophages).
Factors implicated in the development of melasma include:
Melasma presents as bilateral, asymptomatic, light-to-dark brown macules or patches with irregular borders.
Distinct patterns include:
Melasma can be separated into epidermal, dermal, and mixed types, depending on the level of increased melanin in the skin.
Epidermal melasma is defined by:
Dermal melasma is defined by:
Mixed melasma is the most common type, and is defined by:

Melasma
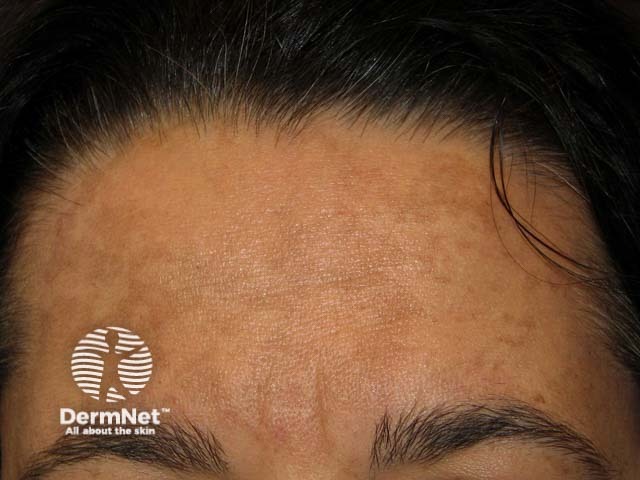
Melasma
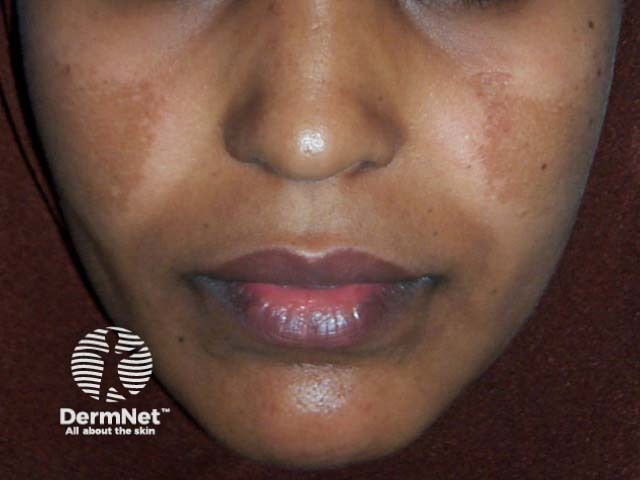
Melasma
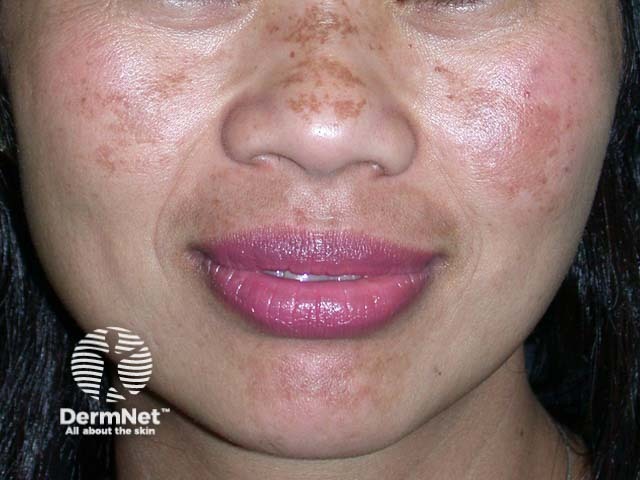
Melasma
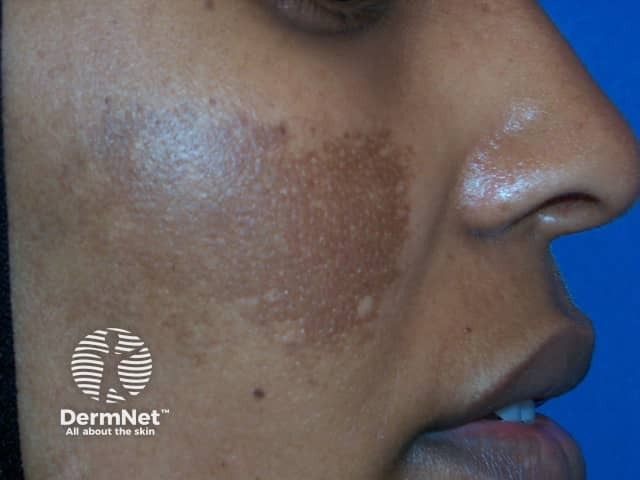
Melasma
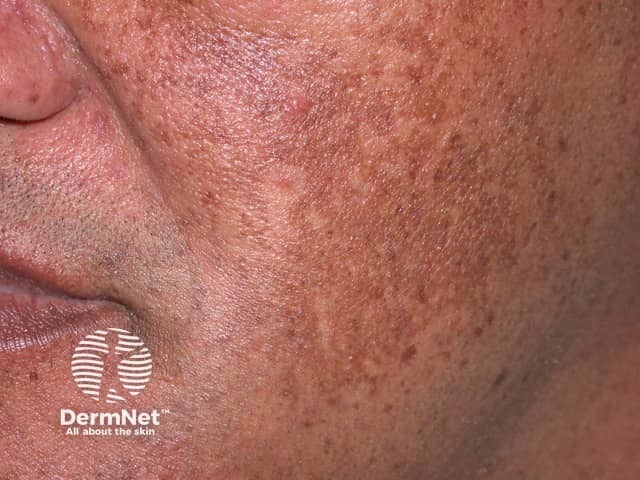
Melasma
See more melasma images.
Melasma can have a severe impact on quality of life due to its visibility.
Melasma is usually a clinical diagnosis based on the clinical appearance, and examination with a Wood lamp and dermatoscope.
Occasionally a skin biopsy may be taken. Histology varies with the type of melasma, but typically the following features are seen:
Serial photography and severity indices such as the Melasma Area and Severity Index (MASI) or modified MASI can be used to monitor response to treatment.
Other disorders that may resemble melasma clinically include:
A combination of measures is generally required.
The most successful formulation has been a combination of hydroquinone, tretinoin, and moderate potency topical steroid (skin lightening cream) reported to clear or improve 60–80%.
Other topical agents used alone or, more commonly, in combination have included:
Many other agents are under investigation. For example, 2-mercaptonicotinoyl glycine (2-MNG), which binds to certain melanin precursors, has shown promise in early clinical trials for preventing hyperpigmentation induced by ultraviolet or visible light.
Tranexamic acid blocks conversion of plasminogen to plasmin, with downstream effects inhibiting synthesis of prostaglandin and other factors involved in melasma.
More new oral treatments are being trialled.
Chemical peels and lasers can be used with caution, but carry a risk of worsening melasma or causing post-inflammatory hyperpigmentation. Patients should be pretreated with a tyrosinase-inhibitor, such as hydroquinone.
Superficial epidermal pigment can be peeled off using alpha-hydroxy acids (AHA), such as glycolic acid, or beta-hydroxy acids (BHA), such as salicylic acid.
Microneedling, intense pulsed light (IPL), and lasers including Q-switched Nd:YAG, ablative and non-ablative fractionated and picosecond lasers carry a high risk for relapse and the disease becoming more resistant to treatment, so require expert use.
Melasma can be frustrating to treat, both for the patient and the medical practitioner. It is slow to respond to treatment, especially if it has been present for a long time.
Even in those who get a good result from treatment, pigmentation may reappear on exposure to summer sun.
The chronicity and risk for relapse with the need for lifelong sun protection should be emphasised to set realistic goals and outcomes.