Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2005; Updated: Casey P Schukow, Medical Student, Michigan State University College of Osteopathic Medicine, Detroit, MI, United States of America; Dr Martin Keefe, Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. August 2021
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Scurvy (scorbutus) is the clinical disease caused by Vitamin C (ascorbic acid) deficiency with characteristic mucocutaneous and musculoskeletal manifestations.
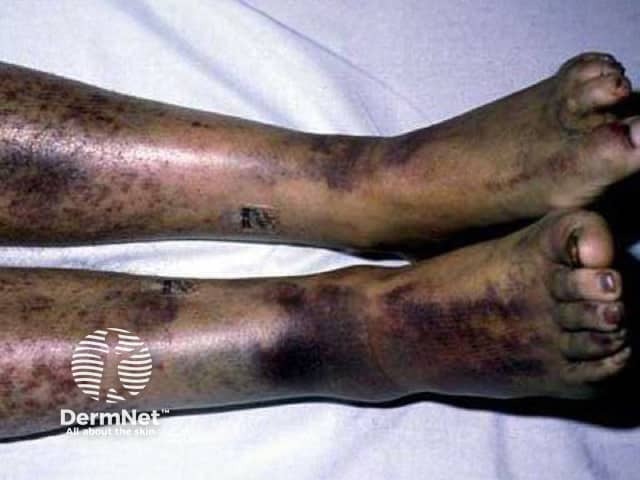
Ecchymoses
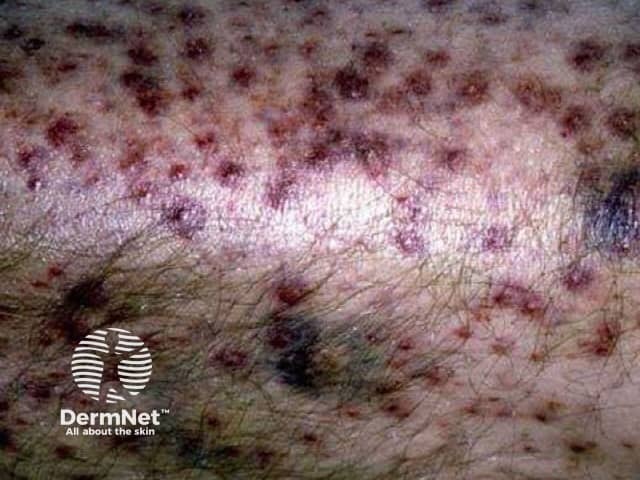
Perifollicular haemorrhage and ecchymoses
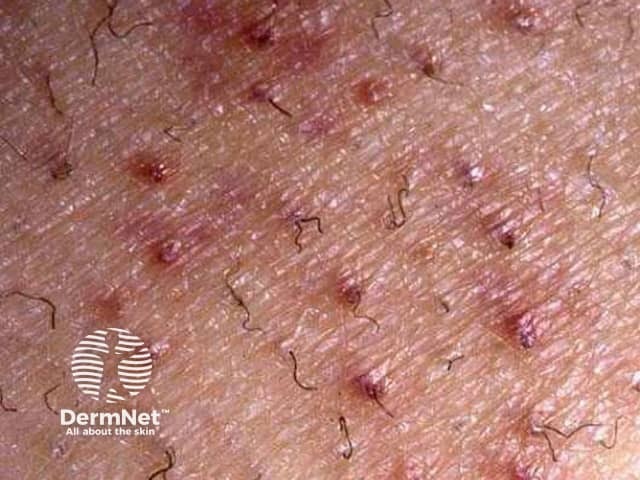
Corkscrew hairs and purpura
Scurvy can affect all age groups, both sexes, and all races. It remains surprisingly common worldwide in both developed and developing countries. The Vitamin C requirement is highest in children and during pregnancy, and lowest in the elderly.
In developed countries vitamin C deficiency affects up to 10% of women and 14% of men. Groups affected include:
In developing countries such as northern India, the incidence can be as high as 73.9% due to limited access to Vitamin C-rich fruit and vegetables.
Scurvy develops when sustained dietary deficiency of Vitamin C for several months reduces total body stores from 1500mg to less than 300mg. Unlike nearly all other animals, humans are unable to synthesise Vitamin C which must be obtained from the diet.
Vitamin C is required for:
The initial clinical features of scurvy are non-specific and include:
As the condition progresses, shortness of breath, wasting, anaemia, oedema, mucocutaneous changes, ocular and musculoskeletal symptoms develop.
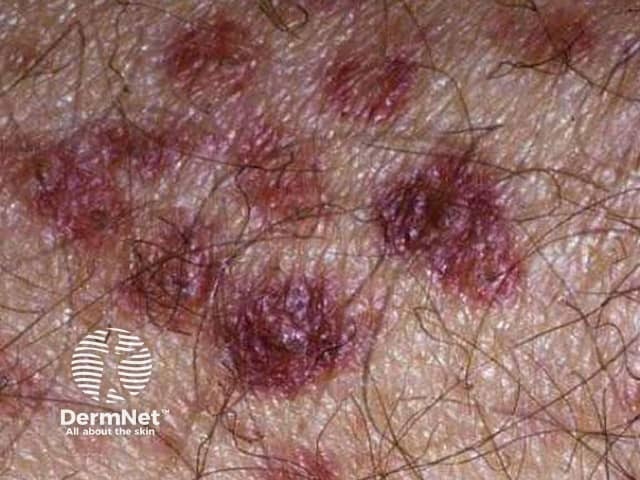
Purpura
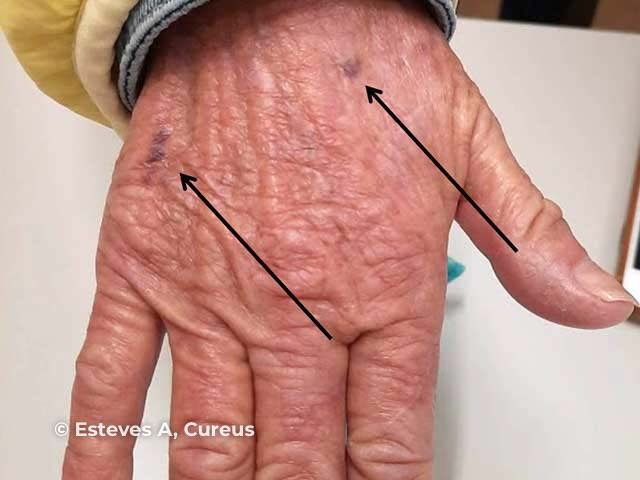
Ecchymoses
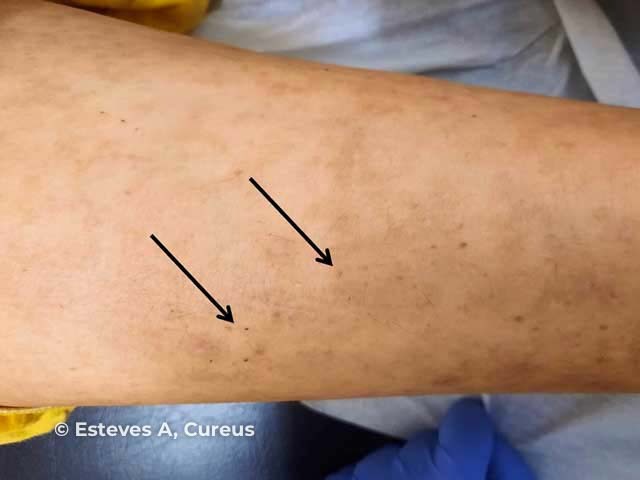
Corkscrew hairs
Images in this gallery of ecchymoses and corkscrew hairs from: Esteves A, Teixeira da Silva F, Carvalho J, Felgueiras P, Laranjeira P. Scurvy, starvation, and flea infestation - a case report from 21st century Europe. Cureus. 2021;13(2):e13158.
Other nutritional deficiencies are commonly associated with scurvy and clinical features may therefore be mixed and therefore confusing.
Perifollicular haemorrhages and ecchymoses may appear dusky blue or a violaceous colour in patients with dark skin types.
Scurvy should be considered on the clinical presentation and confirmed with recovery after Vitamin C supplementation.
Serum levels of Vitamin C reflect recent intake rather than body stores, so are unreliable. Investigation of other nutritional deficiencies should be undertaken.
Anaemia is common, and may be due to decreased iron absorption, bleeding, haemolysis, and other dietary deficiencies.
In children, characteristic changes are seen on X-ray:
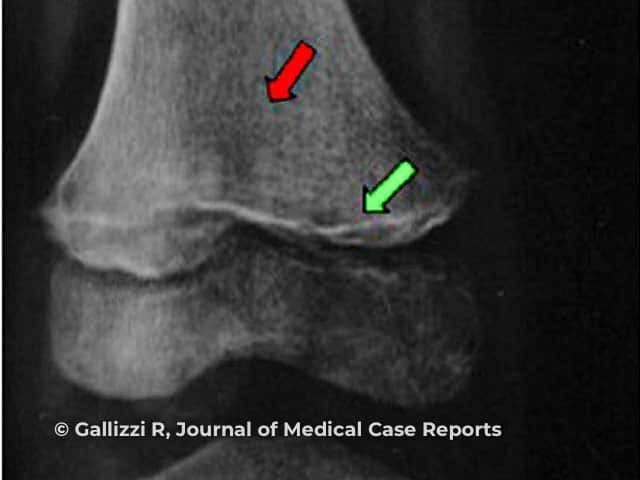
Frankel sign (green arrow), Trummerfeld zone (red arrow)
Image from: Gallizzi R, Valenzise M, Passanisi S, Pajno GB, De Luca F, Zirilli G. Scurvy may occur even in children with no underlying risk factors: a case report. J Med Case Rep. 2020;14(1):18.
The recommended daily intake of Vitamin C in Australia and New Zealand is 45 mg/d. Pregnant and lactating women need 55-85 mg/d. Smokers also require a higher Vitamin C intake due to increased metabolic turnover. A well-balanced diet including fresh fruit and vegetables provides sufficient Vitamin C for most people.
Adults: Oral Vitamin C 1000 mg/d in divided doses for at least one week, then 300-500 mg/d for a further week, followed by the recommended daily allowance.
Children: The American Academy of Paediatrics recommends children receive 100 mg 3 times daily for at least 1 week, followed by 100 mg daily until symptoms have resolved.
Vitamin C can also be given intravenously, intramuscularly, or per rectum.
Transfusion is sometimes required for severe anaemia, especially if acute related to haemorrhage.
Children with bone disease may require surgery if symptoms do not resolve with supplements.
Most symptoms of scurvy resolve rapidly within 24–72 hours of starting Vitamin C supplements. Bone changes may take several weeks to resolve. Full recovery is usual within 1–3 months. Loss of teeth and sequelae from haemorrhage are the only permanent disabilities.
If untreated, scurvy can cause sudden death.
Understanding the reason for developing scurvy, whether this be social or medical, and addressing this will reduce the risk of recurrence.