Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, November 2015.
Introduction Demographics Causes Clinical features Complications Diagnosis Treatment
Gingivitis is inflammation of the gums (gingiva), the visible mucosa around the teeth.
Periodontitis is a chronic, inflammatory disease affecting the gingiva, ligaments and the underlying alveolar bone.
Risk factors for developing gingivitis and periodontitis include:
Gingivitis is caused by:
The build-up of tartar leads to periodontitis. The tartar irritates the gingiva and forms pockets that fill with bacteria, plaque and tartar. Subsequent infection can be serious.
Patients with gingivitis present with:
Patients with the more advanced periodontitis may present with:
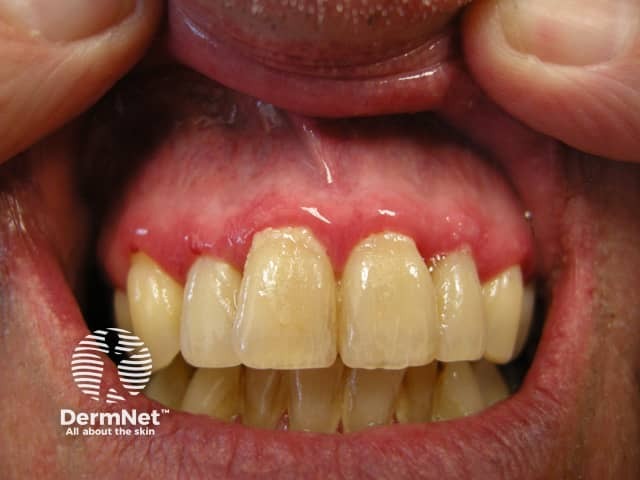
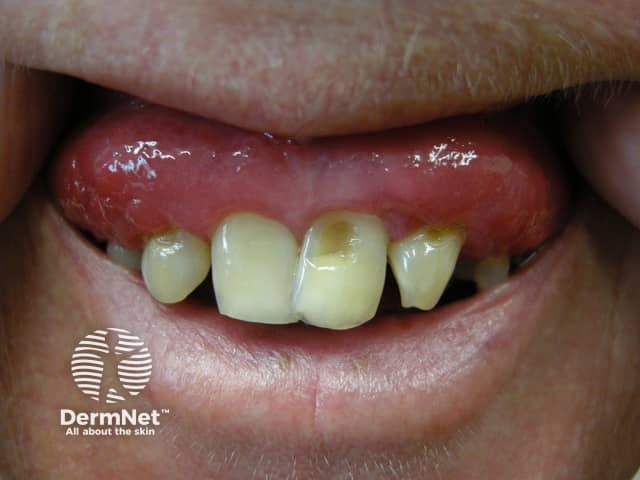
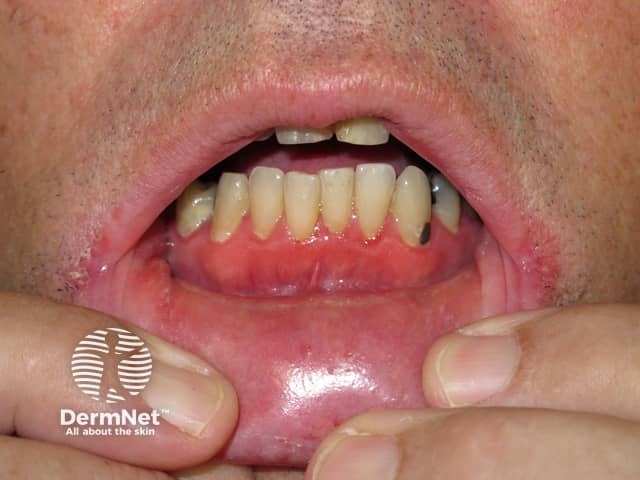
The main complication of untreated gingivitis is periodontitis. Complications stemming from periodontitis include:
The link between periodontitis and increased risk of these serious chronic conditions is not fully understood.
Diagnosis for gingivitis and periodontitis is based upon thorough examination of the patient’s mouth, including cheeks, gums, and tongue. Probes may be used to examine gingival pockets.
X-rays may also be taken to evaluate possible damage to underlying bone structures.
Treatment for gingivitis includes:
Additional treatment for periodontitis includes: