Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Autoimmune/autoinflammatory Rashes
Authors: Dr Kenneth Wong, Dermatology Registrar, Greenlane Hospital, Auckland, New Zealand, 2008; Updated: Dr Malini Sivasaththivel, Resident Medical Officer, Eastern Health, Melbourne, Australia; Dr Martin Keefe, Consultant Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. October 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Autoimmune progesterone dermatitis is a rare, cyclical mucocutaneous hypersensitivity reaction to peak levels of endogenous progesterone seen in the luteal phase of the menstrual cycle.
Autoimmune progesterone dermatitis is predominantly a condition of young adult women with a mean age of onset of 27.3 years; it has also been reported in adolescents after the menarche and in older premenopausal women. It often, but not always, occurs in women who have previously received exogenous progestogens, such as the oral contraceptive pill or fertility treatments. It may present in pregnancy or the post-partum period. There is no genetic risk.
The cause of autoimmune progesterone dermatitis is not known. Hypotheses include:
Sensitised patients then have cyclical symptoms due to an ongoing autoimmune response to the elevated levels of progesterone seen in the luteal phase of the menstrual cycle.
The cause in patients with no prior exposure to exogenous progestogens is unclear.
[see Allergies explained]
Autoimmune progesterone dermatitis characteristically presents as a rash that appears 3–4 days before menstruation when progesterone levels peak. The rash resolves within a few days after the onset of menstruation as progesterone levels reduce, only to recur just before the next period. This cyclical pattern may not be apparent in women with irregular menses.
The type of rash seen in autoimmune progesterone dermatitis can be variable, but the majority of patients present with:
Other reported eruptions include:
Skin changes typically affect the trunk and limbs but may involve the face, oral mucosa, lips, and genitalia.
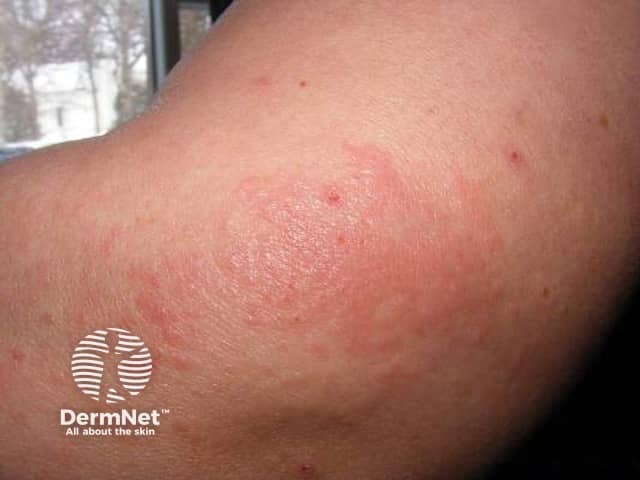
Autoimmune progesterone dermatitis: dermatitis presentation
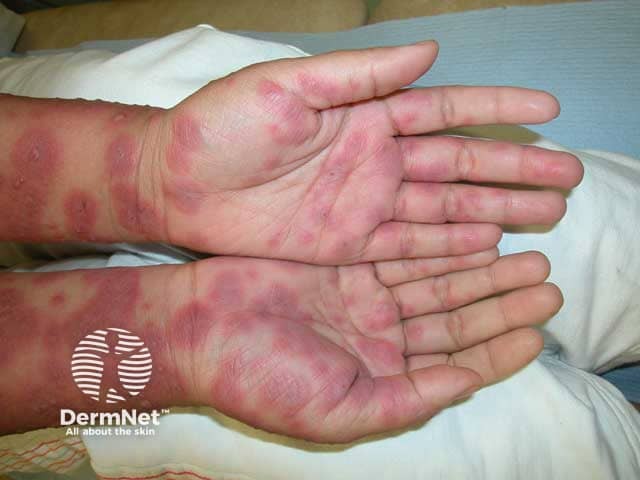
Autoimmune progesterone dermatitis: erythema mulitiforme pattern
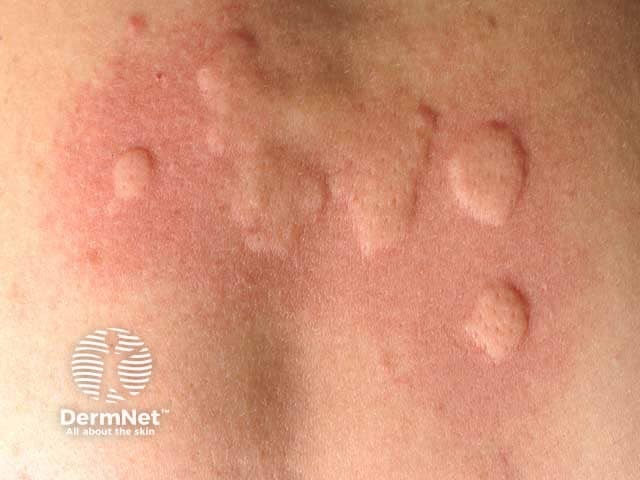
Autoimmune progesterone dermatitis: urticarial pattern
Autoimmune progesterone dermatitis should be considered if:
Intradermal tests with progesterone can be performed and may trigger local or systemic reactions. However, suitable reagents may be difficult to source, the tests are not standardised, and irritant reactions may occur.
Other tests not routinely available include lymphocyte transformation tests, interferon gamma release assay, and demonstration of progesterone-specific IgE on ELISA.
There are no diagnostic skin biopsy findings that distinguish disease triggered by progesterone from other aetiologies.
Autoimmune progesterone dermatitis continues unabated without treatment. Response to treatment is variable. Some women experience a reduction in symptoms during pregnancy which is thought to be due to a natural desensitisation process that occurs with the gradual increase in progesterone during pregnancy; others experience a worsening of symptoms during pregnancy. Autoimmune progesterone dermatitis resolves at menopause and progesterone-containing hormone replacement therapy should not be prescribed.