Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Original article (1997) updated by: Ardalan Akbari, Medical Student, Faculty of Medicine, University of British Columbia, Vancouver, Canada. DermNet Editor in Chief: Adjunct Assoc. Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. October 2019.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Erythema nodosum is a type of panniculitis, an inflammatory disorder affecting subcutaneous fat. It presents as tender red nodules on the anterior shins. Less commonly, they affect the thighs and forearms [1–3].
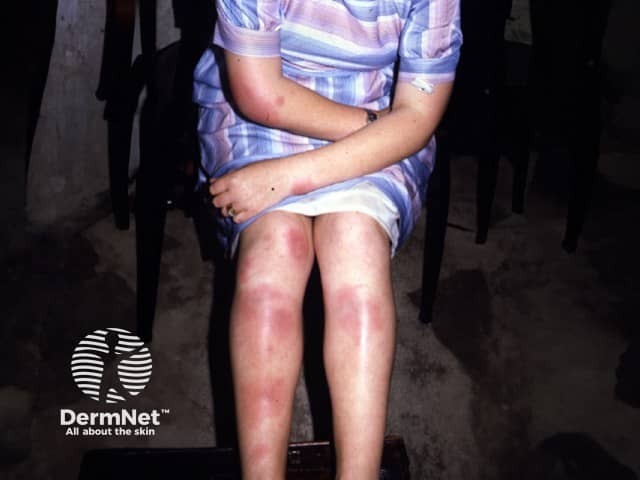
Erythema nodosum
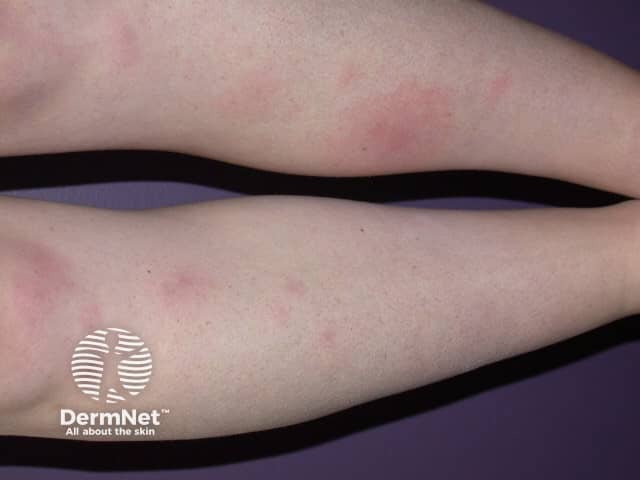
Erythema nodosum
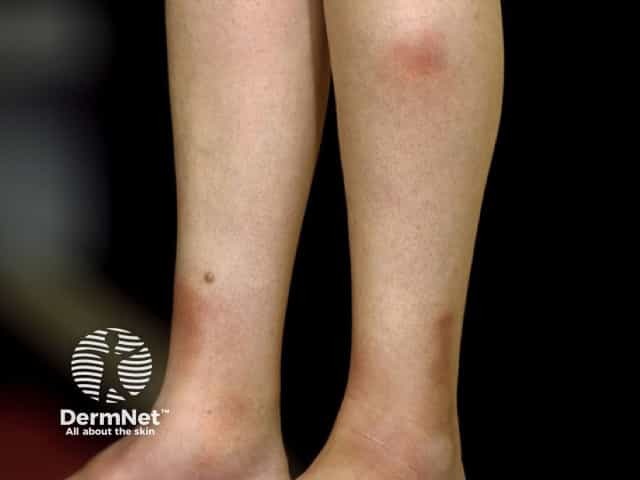
Erythema nodosum
See more images of erythema nodosum.
Erythema nodosum can occur in all ethnicities, sexes, and ages, but is most common in women between the ages of 25 and 40 [4]. It is 3–6 times more common in women than in men except before puberty when the incidence is the same in both sexes [5].
Erythema nodosum is a hypersensitivity reaction of unknown cause in up to 55% of patients [6]. In other cases, it is associated with an identified infection, drug, inflammatory condition, or malignancy [7].
Other viral and bacterial diseases associated with erythema nodosum include herpes simplex, viral hepatitis, human immunodeficiency virus (HIV) infection, Campylobacter infection, and Salmonella infection.
Erythema nodosum presents with tender bilateral erythematous subcutaneous nodules 3–20 cm in diameter erupting over one to several weeks. They are accompanied by fever and joint pain. In 50% the ankle is swollen and painful for up to several weeks. The knees and other joints can also be affected [8].
Erythema nodosum does not cause permanent scarring.
Erythema nodosum has few known complications and lesions usually resolve spontaneously. A rare complication is encapsulated fat necrosis, or ‘mobile encapsulated lipoma’ [14].
Erythema nodosum is primarily a clinical diagnosis confirmed by laboratory tests and histopathology [8]. The pathology of erythema nodosum shows inflammation primarily of the septa between the subcutaneous fat lobules without vasculitis [15].
Appropriate tests may include:
A range of causes of panniculitis should be considered in a patient with subcutaneous nodules, especially if lesions are not located on the legs, there is ulceration, or symptoms last longer than eight weeks.
Panniculitis can be predominantly septal (inflammation between lobules) or lobular (inflammatory cells within subcutaneous fat lobules) [16]. Mixed septal and lobular inflammation can occur.
Nodules due to predominantly septal panniculitis include:
Nodules due to predominantly lobular panniculitis include:
Erythema nodosum is treated based on the underlying disease. An underlying infection should be treated.
Erythema nodosum follows a relatively benign and favourable course. It is important to recognise the underlying cause, if any, and initiate symptomatic treatment [4]. Most cases resolve within days to weeks. Relapses may occur in approximately one-third of cases erythema nodosum may become a chronic or persistent disorder lasting for 6 months and occasionally for years [13].