Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Antonia Birry, Dermatology Registrar, Middlemore Hospital, Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, October 2015.
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outlook
Löfgren syndrome is an acute form of sarcoidosis. Sarcoidosis is a multisystem disorder characterised histologically by granulomas (a specific type of inflammation).
Löfgren syndrome presents with a combination of symptoms and findings:
The syndrome is named after Swedish researcher, Sven Löfgren (1910-1978), who described the symptoms in a series of 113 patients (1953).
Some populations are at greater risk of developing Löfgren syndrome for genetic and environmental reasons.
Despite intensive investigation, the cause of Löfgren syndrome and other forms of cutaneous sarcoidosis is unknown. Sarcoidosis is recognised as a cell-mediated immune response to an unknown antigen, in which activated macrophages and CD4 T-lymphocytes release cytokines that trigger formation of granulomas.
At least some cases of cutaneous sarcoidosis may be due to an unusual host reaction to one or more infective agents, such as Mycobacterium paratuberculosis, histoplasmosis and other fungi. Acute sarcoidosis is not infectious.
Löfgren syndrome commonly presents during the spring months.
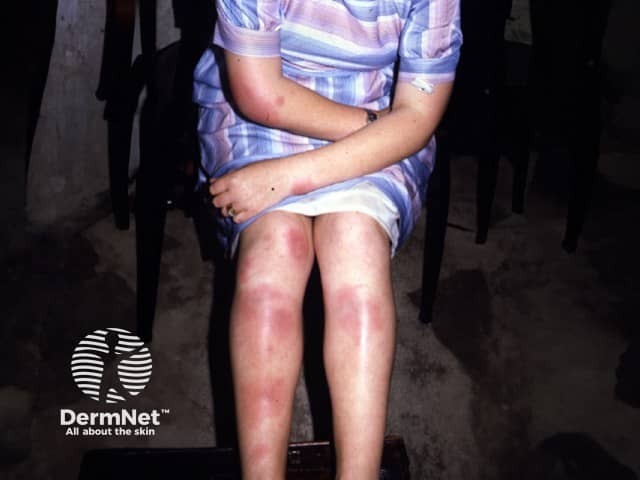
Erythema nodosum
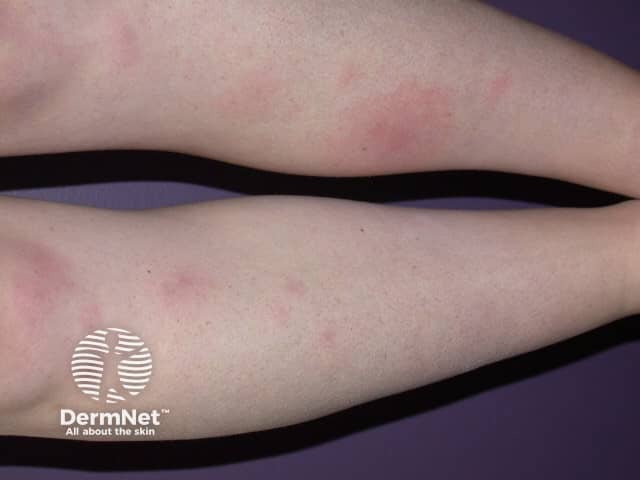
Erythema nodosum
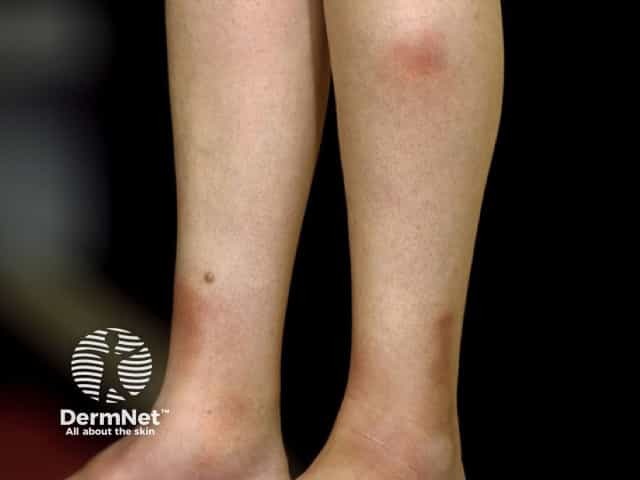
Erythema nodosum
See more images of erythema nodosum
Patients with Löfgren syndrome may present to a dermatologist, respiratory physician, ophthalmologist, rheumatologist or general practitioner because of the variety of possible symptoms.
The diagnosis may be suspected due to typical clinical features. Although not always necessary for diagnosis, diagnosis of sarcoidosis is confirmed by finding non-caseating granulomas on biopsy of lymph nodes. Biopsy of erythema nodosum reveals septal panniculitis.
Chest X-ray reveals bilateral hilar lymphadenopathy ie enlarged lymph nodes in the centre of the chest.
Blood tests may find elevated levels of:
It is important to exclude tuberculosis. Tuberculin skin test and QuantiFERON® gold blood test are negative in sarcoidosis.
Most patients with Löfgren syndrome are treated with nonsteroidal anti-inflammatory drugs (NSAIDs), which reduce discomfort and inflammation of erythema nodosum and arthritis. Other drugs occasionally used for Löfgren syndrome include:
Compression socks can reduce swelling and discomfort of erythema nodosum.
The prognosis of Löfgren syndrome is good, with complete resolution with or without treatment within 6 months to 2 years.
It is usual to repeat chest X-rays from time to time until the lymphadenopathy has fully resolved.