Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Antonia Birry, Dermatology Registrar, Middlemore Hospital, Auckland. Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, August 2015.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outlook
Lupus pernio is one of the more common forms of cutaneous sarcoidosis. Sarcoidosis is a multisystem disorder characterised histologically by granulomas (a specific type of inflammation).
Lupus pernio presents as bluish-red or violaceous nodules and plaques over the nose, cheeks and ears.
The name is derived from the Latin name for 'wolf' (lupus) and for 'chilblain' (pernio). This is because it was thought to be related to lupus vulgaris (cutaneous tuberculosis) by Besnier (1889). Lupus pernio is also called nodular or plaque sarcoidosis and sarcoidosis, lupus pernio type.
Some populations are at greater risk of developing lupus pernio. The annual incidence varies from 1 to 64 per 100,000.
Despite intensive investigation, the cause of lupus pernio and other forms of cutaneous sarcoidosis is unknown. Sarcoidosis is recognised as a chronic cell-mediated immune response to an unknown antigen, in which activated macrophages and CD4 T-lymphocytes release cytokines that trigger the formation of granulomas.
At least some cases of cutaneous sarcoidosis may be due to an unusual host reaction to one or more infective agents, such as Mycobacterium paratuberculosis, histoplasmosis and other fungi. Lupus pernio itself is not infectious.
It is uncertain why lupus pernio affects sites where the skin is cool.
Lupus pernio is usually asymptomatic, and it rarely causes itch or pain. Cosmetic disfigurement is the most common complaint.
It presents as indolent reddish-purple plaques and nodules on the nose, cheeks, lips, ears and digits. Lesions may ulcerate and later heal with telangiectatic scars.
Lesions on the nasal rim are associated with granulomatous inflammation of the upper respiratory tract. The skin lesions may extend to the nasal septum leading to nosebleeds and crusting.
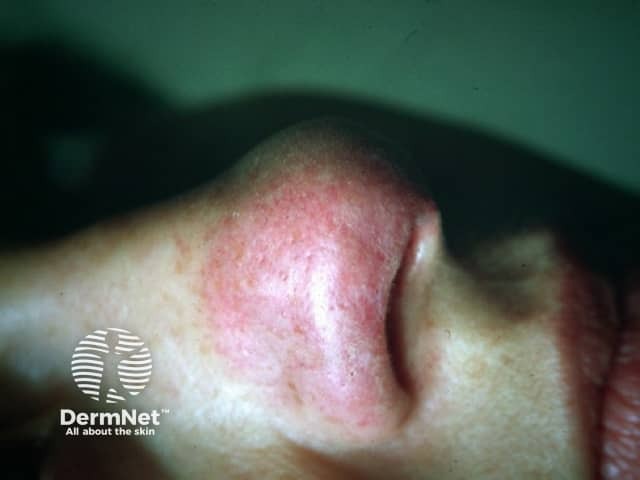
Lupus pernio. Cutaneous sarcoidosis
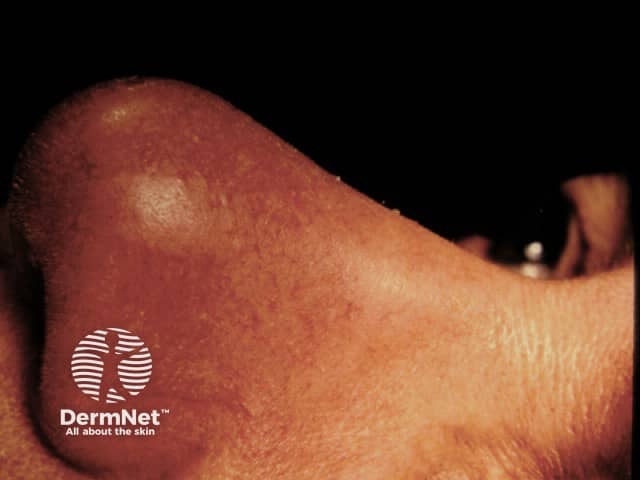
Lupus pernio. Cutaneous sarcoidosis
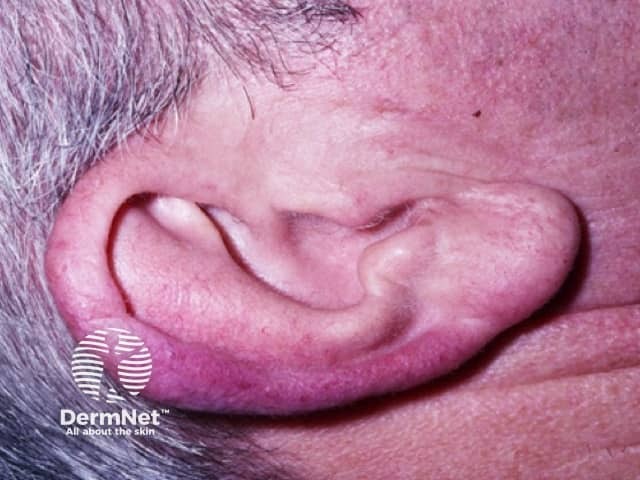
Lupus pernio. Cutaneous sarcoidosis
Lupus pernio may be recognised by its typical clinical appearance and history, but the diagnosis may difficult to establish and delayed.
Examination of the edge of the skin lesion using diascopy, or pressure with a glass slide, shows apple-jelly appearance typical of granulomatous inflammation.
Biopsy of the skin, lymph nodes or lungs confirms the diagnosis by revealing sarcoidal non-caseating granulomas.
As lupus pernio is associated with sarcoidosis in the lungs (75% of patients) and upper respiratory tract (50%), the following tests should also be performed at diagnosis and for monitoring:
It is important to exclude tuberculosis. Tuberculin skin test and QuantiFERON® gold blood test are negative in sarcoidosis.
The differential diagnosis can include various types of cutaneous lupus erythematosus.
The goal of the treatment of lupus pernio is to improve the patient's appearance and prevent scarring. The treatment chosen may depend on the severity of systemic symptoms.
The treatment has varying success. Options include:
Cosmetic camouflage may be used to disguise skin lesions.
Lupus pernio tends to persist for several years and seldom resolves spontaneously. Lung and cardiac function should be monitored.