Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2006. DermNet Update August 2021
Introduction
Demographics
Causes
Clinical features
Complications
Differential diagnoses
Diagnosis
Treatment
Outlook
Necrobiosis lipoidica is a rare granulomatous skin disorder typically described on the shin of diabetics.
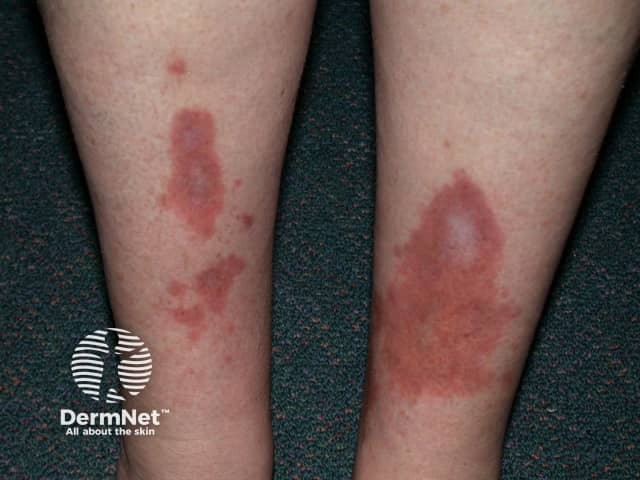
Necrobiosis lipoidica
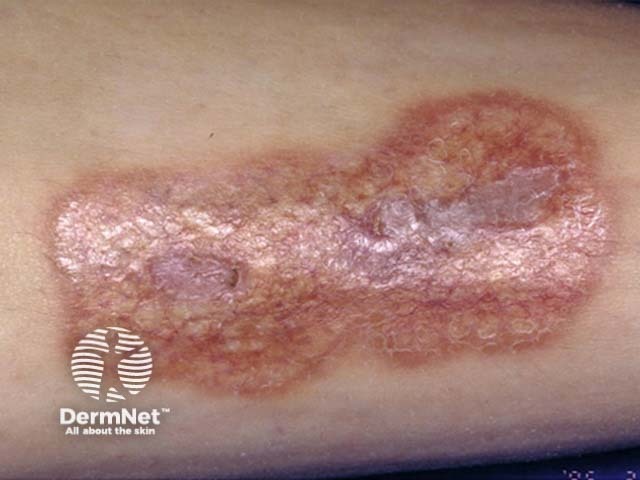
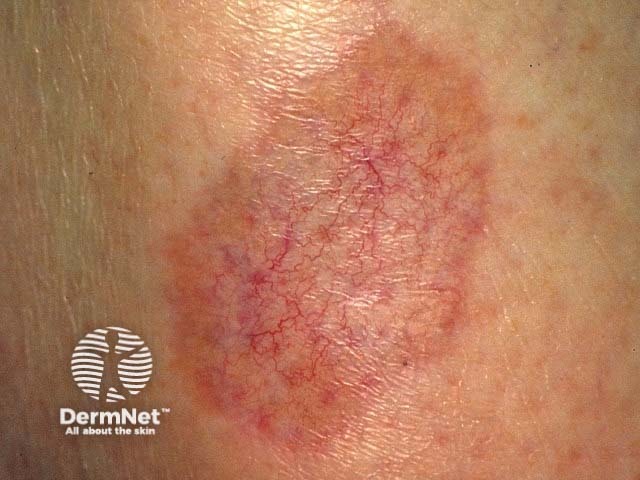
Necrobiosis lipoidica is three times more common in females than in males, and usually develops in young and middle-aged adults.
The cause of necrobiosis lipoidica is unknown. Theories have included blood vessel changes such as develop in diabetes, or antibody-mediated vasculitis.
Necrobiosis lipoidica begins as a dull red papule or plaque on the shin which slowly enlarges into one or more yellowish-brown patches with a red rim.
The patches:
In skin of colour, the patches and plaques of necrobiosis lipoidica may be hyperpigmented around the periphery with hypopigmentation developing centrally with the atrophy and telangiectases.
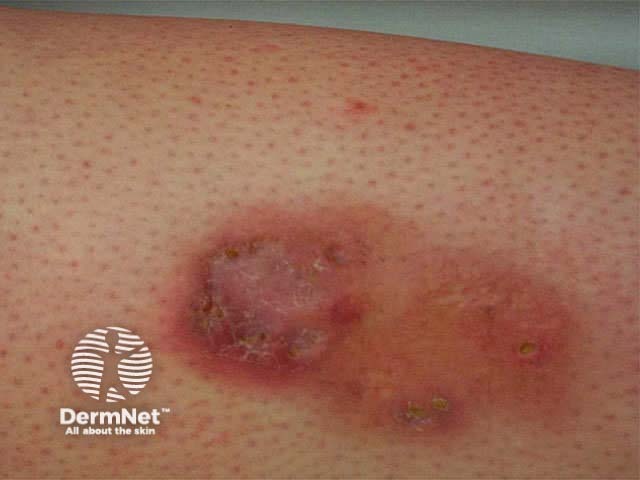
Necrobiosis lipoidica
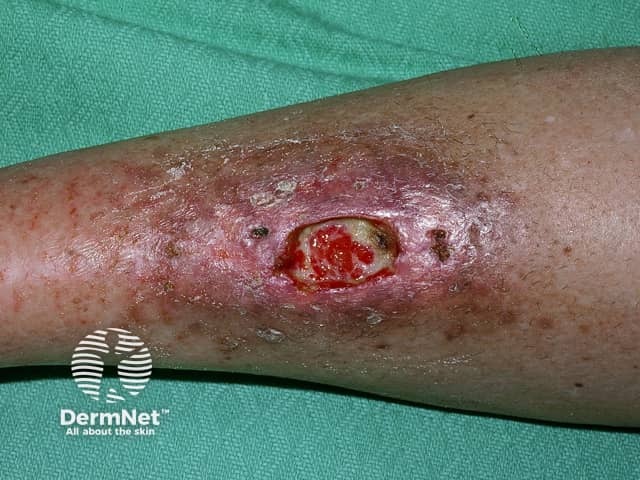
Ulcerated necrobiosis lipoidica
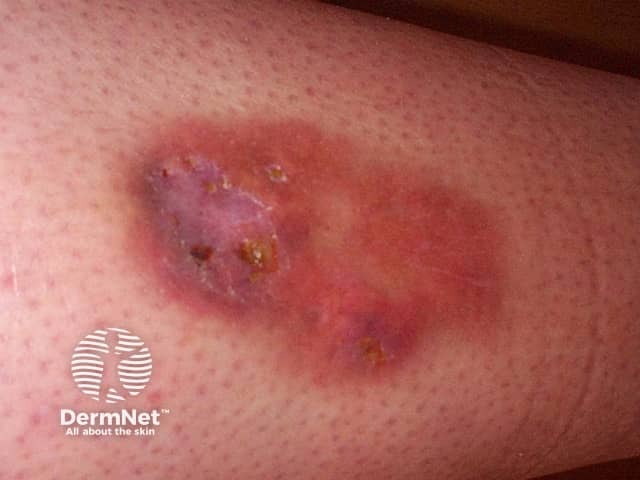
Ulcerated necrobiosis lipoidica
Necrobiosis lipoidica is diagnosed clinically when typical.
A skin biopsy may be performed to confirm the diagnosis. The histopathology is characteristic; it shows a granulomatous inflammatory reaction around destroyed collagen (necrobiosis). [see Necrobiosis lipoidica pathology].
Not all cases of necrobiosis lipoidica require treatment and treatment is generally disappointing. The following treatments are sometimes effective:
Necrobiosis lipoidica is a chronic condition that may remain stable or slowly progress over years. Spontaneous resolution has been reported.