Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Chief Editor, Hon A/Prof Amanda Oakley, January 2016.
Introduction
Relation to systemic polyarteritis
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outlook
Cutaneous polyarteritis nodosa (PAN) is a rare form of vasculitis (inflammation of blood vessels) that involves small and medium-sized arteries of the dermis and subcutaneous tissue. It is sometimes called periarteritis nodosa.
Although identical skin lesions are common in systemic PAN, cutaneous PAN should be considered a separate disease and distinguished from systemic PAN, as the clinical course and management of these conditions differ from each other.
Systemic PAN is a vasculitis that causes destructive inflammation of medium-sized muscular arteries of multiple systems including the liver, kidney, heart, lung, gastrointestinal tract, musculoskeletal and nervous systems. Systemic PAN is a potentially life-threatening form of vasculitis, whereas cutaneous PAN usually runs a chronic but relatively benign course.
Cutaneous polyarteritis nodosa often starts in childhood or adolescence. It is rare.
In most cases of cutaneous PAN, the disease is triggered by certain infections, particularly Group A streptococcus, hepatitis B, hepatitis C, human immunodeficiency virus, parvovirus B19 (the cause of fifth disease). Genetic defects lead to over-reaction to the infection.
Cutaneous PAN results from a complex interaction of autoinflammatory and autoimmune factors, and immunodeficiency.
Autosomal recessive mutations in the CERC1 gene have been implicated in some patients with cutaneous PAN. This genetic abnormality results in deficiency in the ADA2 protein (DADA2). DADA2 can also cause immunodeficiency. ADA2 is a plasma protein essential for development of endothelial cells (these line the blood vessel wall), and leucocytes (white blood cells). DADA2 leads to uncontrolled, chronic activity of neutrophils and damages endothelial cells.
Clinical features of cutaneous polyarteritis nodosa relate to inflammation or occlusion of small and medium-sized blood vessels in the skin and sometimes in other organs. It tends to have periods of activity and remission.
Vasculitic lesions are most often found on the legs and feet. Other areas that may be affected include the arms, trunk, buttocks, and head and neck. They are most likely on pressure points such as the knees, back of the foot and lower leg.
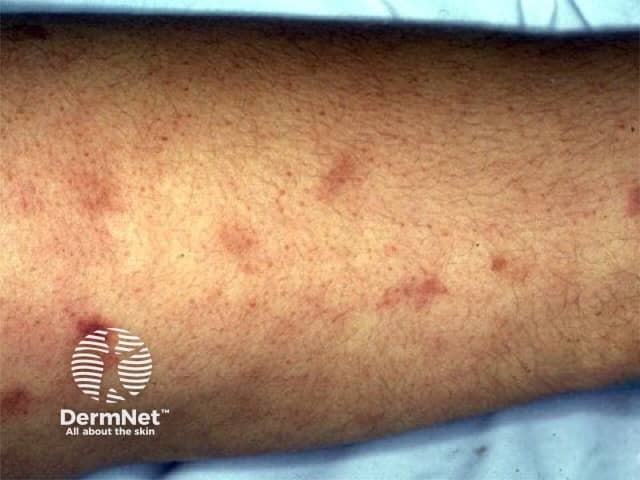
Cutaneous polyarteritis nodosa
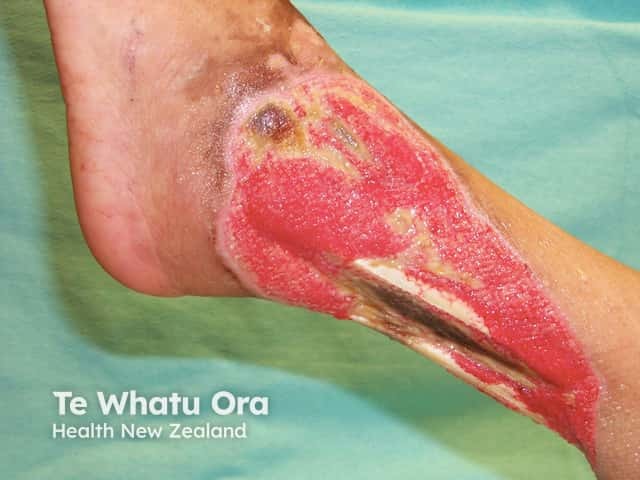
Cutaneous polyarteritis nodosa
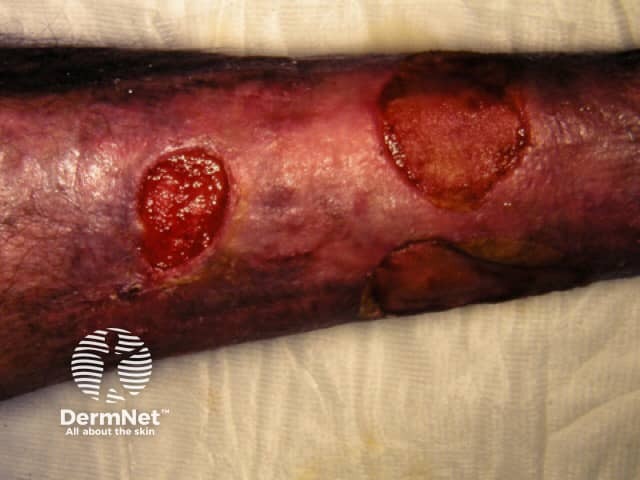
Cutaneous polyarteritis nodosa
In addition to the skin problems, patients with cutaneous PAN may also have generalised symptoms such as malaise, fever, sore throat, and joint and muscle aches and pains. Neurological symptoms may also be present and include numbness, tingling, sensory disturbances, weakness, and absent reflexes.
Skin biopsy of a typical lesion is often performed to make an accurate diagnosis of cutaneous PAN. A specimen showing panarteritis (inflammation of all blood vessels in the skin sample) is the only definitive proof of PAN.
Laboratory tests of blood samples are generally unhelpful in diagnosing or monitoring cutaneous PAN, as blood counts and chemistry are often normal. They are initially required to determine the cause of vasculitis or to exclude other organ involvement as occurs in systemic PAN.
Levels of ADA2 protein and/or CERC1 gene can be measured in some centres.
As cutaneous PAN is rare, there are no randomised trials to guide treatment. Standard treatment follows guidelines for other forms of vasculitis. The mainstay of treatment is often with oral corticosteroids (prednisone).
Other active treatments for cutaneous PAN may include:
Warfarin (with an international normalised ratio [INR] of 3) has been reported to be effective in 3 cases of cutaneous polyarteritis nodosa with improvement in livedo reticularis and healing of ulcers.
New therapies are being developed for patients with cutaneous PAN that have DADA2. These unproven treatments include:
Cutaneous PAN usually runs a chronic course lasting from months to years with exacerbations and remissions. Neurological symptoms and muscular aches and pains usually resolve over a matter of months, whilst skin lesions take longer to heal.
Remissions may occur spontaneously or as a result of treatment.
Medscape: