Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1998. Updated September 2015.
Introduction
Causes
Demographics
Symptoms
Complications
Diagnosis
Treatment
Erythema infectiosum is a common childhood infection causing a slapped cheek appearance and a rash. It is also known as fifth disease and human erythrovirus infection.
Erythema infectiosum is caused by an erythrovirus, EVB19 or Parvovirus B19. It is a single-stranded DNA virus that targets red cells in the bone marrow. It spreads via respiratory droplets, and has an incubation period of 7–10 days.
Erythema infectiosum most commonly affects young children and often occurs in several members of the family or school class. Thirty percent of infected individuals have no symptoms. It can also affect adults that have not been previously exposed to the virus.

Fifth disease
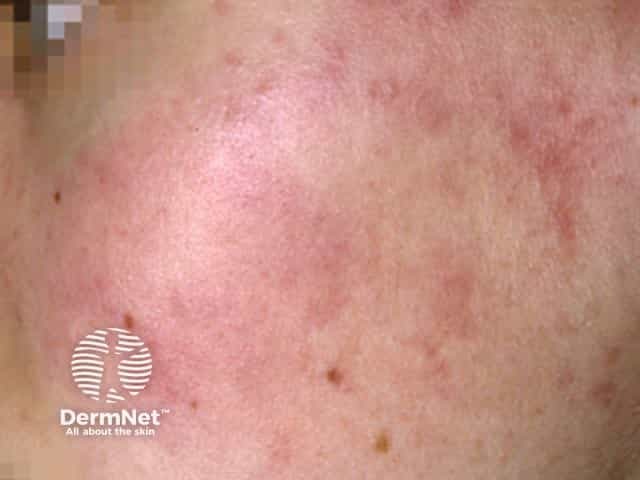
Fifth disease
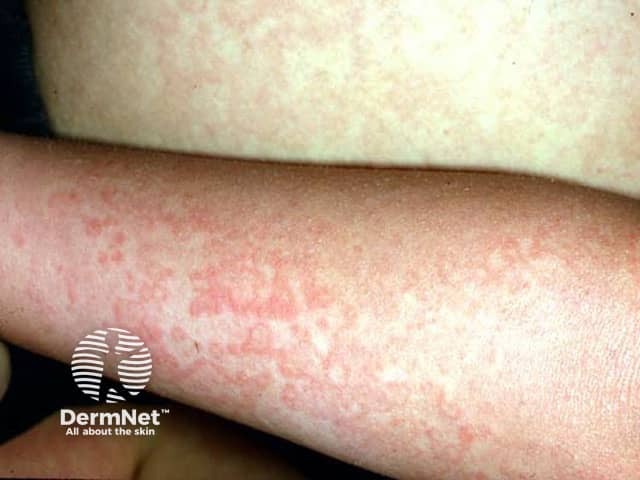
Fifth disease
See more images of erythema infectiosum ...
Parvovirus B19 infection causes nonspecific viral symptoms such as mild fever and headache at first. The rash, erythema infectiosum, appears a few days later with firm red cheeks, which feel burning hot. This lasts 2 to 4 days, and is followed by a pink rash on the limbs and sometimes the trunk. This develops a lace-like or network pattern.
Although most prominent in the first few days, the rash can persist for up to six weeks at least intermittently, and is most obvious when warm.
Although usually a mild childhood condition, erythrovirus B19 infection can result in complications. These include:
In most cases, erythema infectiosum is a clinical diagnosis in a child with characteristic slapped cheek and lacy rash. Parvovirus can cause other rashes such as a papular purpuric gloves and socks syndrome. The diagnosis can be confirmed by blood tests.
If the child is unwell, or has haemolytic anaemia, a full blood count should be performed. Ultrasound examination and Doppler examination of at-risk pregancies can detect hydrops fetalis.
Erythema infectiosum is not generally a serious condition. There is no specific treatment. Affected children may remain at school, as the infectious stage or viraemia occurs before the rash is evident.