Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Topical steroids are very important drugs used to control inflammatory skin diseases, particularly dermatitis.
In general, use a potent preparation short term (a few days or weeks) and weaker preparation for maintenance between flare-ups. Pulse therapy refers to the application of a corticosteroid for 2 or 3 consecutive days each week or two. This is useful for maintaining control of chronic diseases such as psoriasis. Generally a milder topical steroid or non-steroid treatment is used on the in-between days.
Prescribe in an appropriate base:
And in adequate quantities:
| Table 1: Topical steroids available in New Zealand | |
|---|---|
| Class 1: very potent (up to 600 times as potent as hydrocortisone) |
|
| Class 2: potent (I50-100 times as potent as hydrocortisone) |
|
| Class 3: moderate (2-25 times as potent as hydrocortisone) |
|
| Class 4: mild |
|
Corticosteroids are absorbed at different rates depending on the thickness of the stratum corneum. A mild topical steroid that works on the face may achieve little on the palm. But a potent steroid may quickly cause side effects on the face.
For example:
Absorption is greater in an ointment base, in the presence of a keratolytic agent such as salicylic acid and under occlusion.
Percutaneous absorption of topical steroids may rarely result in systemic side effects. More than 50g of clobetasol propionate or 500g of hydrocortisone each week can result in adrenal gland suppression in an adult and/or eventually Cushing syndrome. Proportionally smaller quantities may affect children.
Local side effects of topical steroids are more common and include:
The risk of these side effects depends on the strength of the steroid, the length of application, the site treated, and the nature of the skin problem. A potent steroid cream applied to the face results in side effects within a few weeks. 1% hydrocortisone cream on hands and feet would be most unlikely to cause problems.
In children, cutaneous thinning secondary to potent topical steroids appears to be at least partly reversible and is rarely a problem.
Striae Steroid atrophy and purpura Perioral dermatitis 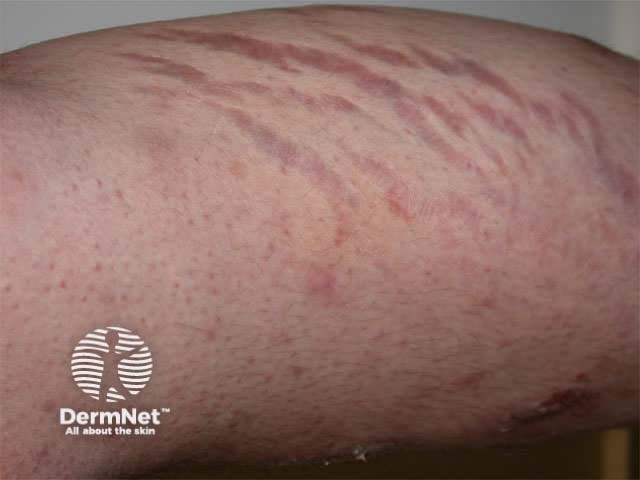
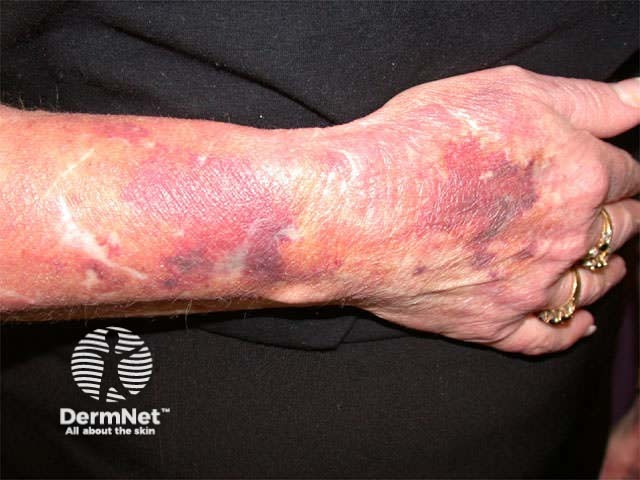
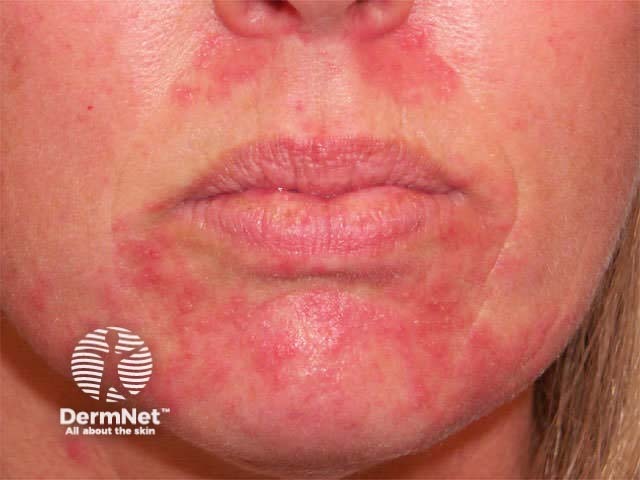
The only available injectable steroid is triamcinolone acetonide as 1ml ampoules of 10mg/ml or 40mg/ml. Blebs of 0.05 to 0.1ml can be cautiously injected into the dermis at 1cm intervals to a maximum of 1 to 2ml, for the following inflammatory skin diseases:
Injections should not be repeated for 4 to 6 weeks. The main complication, atrophy, arises if the injection is delivered into subcutaneous tissue instead of the dermis. Infection, sterile abscesses and hypopigmentation occur rarely.
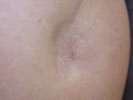 Subcutaneous atrophy |
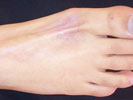 Atrophy and hypopigmentation |
Patients prescribed systemic steroids for skin diseases should be carefully advised of potential risks and adverse effects.
Acute dermatoses
Systemic steroids may be used to treat acute severe skin diseases such as plant contact allergy, autosensitisation dermatitis, flares of atopic dermatitis, Sweet disease and drug hypersensitivity syndrome. They may also be used initially to gain control in extensive or symptomatic lichen planus. Acute urticaria is better managed with oral antihistamines but if they are not effective many practitioners prescribe systemic steroids to provide the patient with short-term relief.
In general, an adult patient should be treated with 40 mg of prednisone for as long as it takes to control the skin disease properly and then it should be tapered. For acute contact dermatitis, it can be discontinued as soon as the rash is controlled (about 7 to 10 days) providing the patient is no longer in contact with the source of the eruption. Courses of three or four weeks may be adequate for other forms of dermatitis and Sweet disease.
The use of intermittent intramuscular triamcinolone 40 to 80 mg stat has fallen out of favour. It is more difficult to adjust doses, corticosteroid side effects may be as troublesome as with oral prednisone, and subcutaneous atrophy is a relatively common complication. The once-monthly dose of triamcinolone acetonide is the same as would be used for prednisone per day.
Chronic dermatoses
Chronic autoimmune skin conditions should only be treated with systemic steroids (usually oral prednisone) if they are resistant to other medications and after careful consideration of the risk / benefit ratio. Examples may include:
Systemic steroids are best avoided in psoriasis as they can make control of the disease very difficult, particularly after steroid withdrawal. In rare cases of severe psoriasis, they may be the only appropriate drug but should only be prescribed under the supervision of an experienced dermatologist.
Starting dose is usually 40 mg of prednisone with breakfast for two to four weeks. If the disease is poorly controlled, the dose may be increased to 60 to 80 mg daily but blood pressure, serum glucose and side effects will require careful monitoring. Once controlled, the dose of steroids should be reduced by half for at least two weeks. Further reduction will depend on the break-through dose, the severity of the underlying skin disease and the availability or efficacy of steroid-sparing agents. The dose of long term prednisone should be as low as possible, as for other chronic diseases, and if possible taken on alternate days.
If steroids are likely to be used for more than a few weeks, consider bone protection. Arrange a DEXA bone density scan. Prescribe calcium, vitamin D or in high risk individuals, a bisphosphonate from the first day of treatment.
Patient information
Patients on long term steroids should be told:
Cutaneous side effects of systemic steroids may include:
Discuss the diagnosis and management of contact allergy to topical steroids.
Information for patients
See the DermNet bookstore