Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2002. Updated by Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2014.
What is a corticosteroid?
Clinical features
Diagnosis
Corticosteroid classification
Cross-reactions
Treatment
Prevention
Corticosteroids, also referred to as steroids or cortisone, are a group of anti-inflammatory agents used in the treatment of many conditions and diseases. There are many different types of corticosteroids with varying potencies and actions. Topical corticosteroids are used in many inflammatory rashes. They are available in a variety of forms such as creams, ointments, lotions, eye preparations and eardrops.
Topical steroids are also commonly found in combination preparations with antibacterials and antifungal agents. These prescription and non-prescription preparations are used to treat a variety of skin, eye and external ear disorders that have become inflamed and sometimes infected.
Corticosteroids or steroids are not related to the anabolic steroids that are misused by some athletes to increase performance.
Corticosteroids were declared the Contact Allergen of the Year for 2005 by the American Contact Dermatitis Society (ACDS).
Topical corticosteroid sensitivity produces classic allergic contact dermatitis reactions. Usually this is seen as a failure to improve or a worsening of an existing dermatitis that is being treated with corticosteroids. Very rarely, corticosteroid allergy may appear as an eczematous rash in a completely different area of the body from the original dermatitis.
Very rarely, severe allergy to a topical corticosteroid is associated with allergy to oral or injected corticosteroids.
A contact allergy to topical steroids is distinct from an erythematous rash in patients that have used topical corticosteroids frequently over long periods of time and may develop topical corticosteroid withdrawal syndrome.
Allergic sensitivity to a topical corticosteroid is usually only picked up when an eczematous dermatitis being treated by a topical corticosteroid fails to respond to treatment or worsens. In cases of persistent or exacerbating dermatitis treated with corticosteroid preparations, corticosteroid sensitivity should be considered. However, it may also be due to irritation from or allergy to other components of the preparation such as preservatives. Lanolin, ethylenediamine, quaternium-15 and the antibacterial agent neomycin, are all known to be potent sensitisers.
Corticosteroid allergy is diagnosed by performing special allergy tests, ie patch tests, and in some cases intradermal tests. There are many topical corticosteroid preparations available; allergy may arise to one or more of these. Positive patch test reactions to budesonide and tixocortol-21-pivalate are a good indicator of corticosteroid allergy. These 2 corticosteroids are often included in the standard panel. Further testing with other corticosteroids should be done if these 2 indicators are positive.
Patch testing may be performed using a standard corticosteroid series. In ideal conditions, a positive patch test result to both the commercial preparation and the isolated active corticosteroid agent should be achieved to confirm the diagnosis. Corticosteroid series may vary slightly, but generally include at least the following:
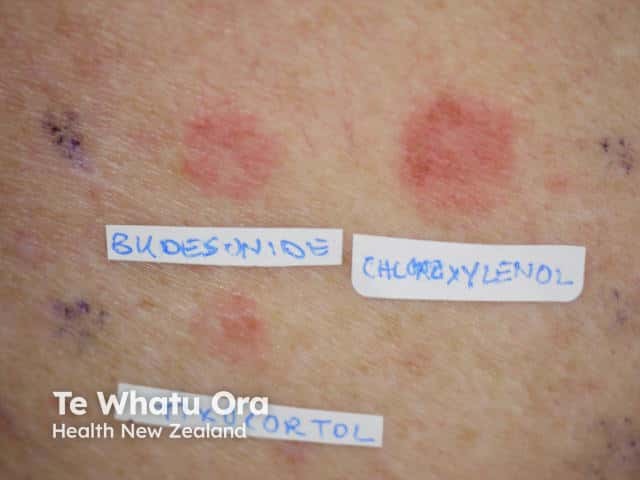
Positive patch test to topical corticosteroids
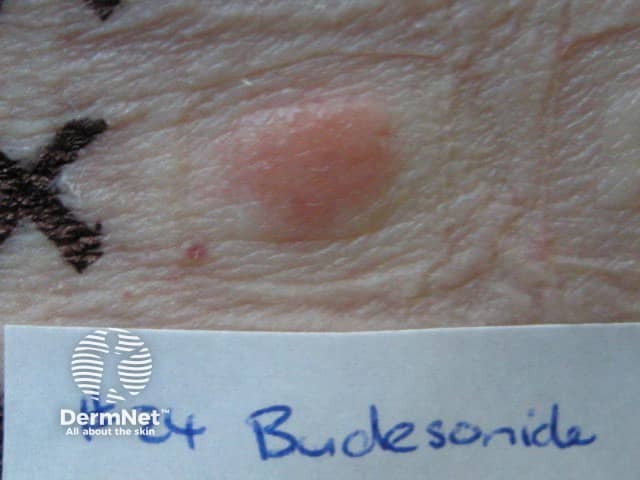
Positive patch test to budesonide
Corticosteroids are classified according to their structure. A specific compound is used to screen for class-specific reactions. When patch tests show allergy to a specific topical steroid, it is likely that the patient will also be allergic to others in the same class.
Test substance: tixocortol pivalate
Test substance: budesonide and triamcinolone
Test substance: clobetasol-17-propionate
Test substance: hydrocortisone-17-butyrate
Sometimes, people can react to corticosteroids in more than one class.
Confirmation of corticosteroid allergy requires the prompt removal of the causative agent and then management as for any acute dermatitis/eczema; this may include treatment with topical corticosteroids (one which you are not allergic to) emollients and treatment of any secondary bacterial infection (Staphylococcus aureus), etc.
Your doctor or dermatologist should give you a list of all the names of the corticosteroids or corticosteroid groups to which you are allergic. You must avoid using any preparations that contain any of the listed corticosteroids.
Many anti-inflammatory skin preparations, antibiotic creams and ointments, eye and ear preparations contain corticosteroids (hydrocortisone). If purchasing over-the-counter products alert your pharmacist to the fact that you have a contact allergy to corticosteroids and provide them with the list of the corticosteroids you are allergic to. Note that a non-prescription cream may contain an illegal corticosteroid.
Always alert your doctor to the fact that you have a contact allergy to corticosteroid so that they can prescribe you a suitable alternative if necessary.
Your dermatologist may have further specific advice, particularly if you are highly sensitive to a corticosteroid.