Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last reviewed: March 2023
Author(s): Dr Libby Whittaker, Medical Writer, New Zealand (2023)
Previous contributors: Vanessa Ngan (2002)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Where is it found?
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Lanolin is a natural product obtained from the fleece of sheep and is used in a variety of topical therapeutic and cosmetic preparations.
It is a complex mixture mainly composed of high molecular weight esters (>80%), along with aliphatic alcohols, fatty acids, sterols, and hydrocarbons. Free alcohols are considered the main sensitisers in lanolin.
The term lanolin is derived from the Latin terms lana (‘wool’) and oleum (‘oil’); sebum is extracted from sheep’s wool, cleaned, and refined. A variety of different terms are used to refer to lanolin (and its components and derivatives), such as wool alcohols, wool fat, anhydrous lanolin, amerchol, lanolin alcohol, alcoholes lanae, wool wax, and wool grease.
Lanolin is the 2023 American Contact Dermatitis Society (ACDS) Allergen of the Year, named due to the increasing frequency of allergic reactions.

Sheep wool - the source of lanolin
Lanolin, which usually acts as a protective coating in the fleece of sheep, is a good emulsifier and is found in many pharmaceutical preparations, cosmetics, and toiletries. It also has industrial uses eg, applied to metallic surfaces to prevent corrosion.
Pharmaceuticals |
Cosmetics |
Industrial |
|
|
|
The prevalence of lanolin contact allergy is debated. In patients with dermatitis undergoing patch testing, positive patch tests rates are between 1.7 and 3.3%. Some studies have found a female predominance. The rate of contact allergy to lanolin in the general population has been estimated to be lower (<0.5%).
Those with broken or compromised skin due to pre-existing dermatitis (eg, venous eczema, atopic dermatitis) or wounds (particularly leg ulcers) appear to be at higher risk of sensitisation to lanolin. Because of this, contact allergy to lanolin is slightly more common in children (higher rates of atopic dermatitis) and the elderly (higher rates of atopic and venous eczema, and lower limb ulcers).
Allergic contact dermatitis (ACD):

Positive patch test to wool alcohols at 96 hrs
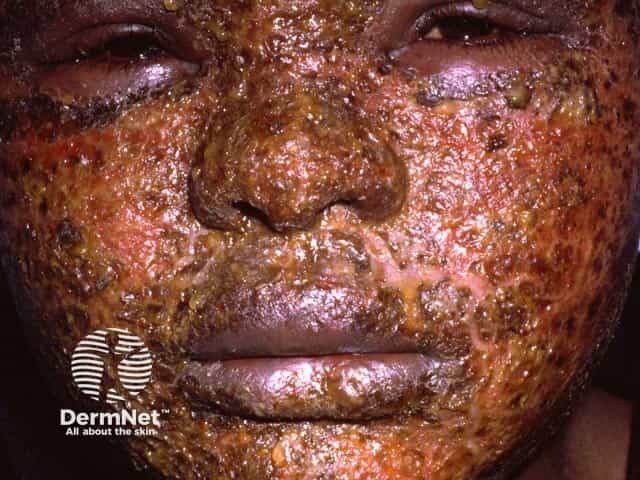
Severe acute allergic contact dermatitis - lanolin was the culprit
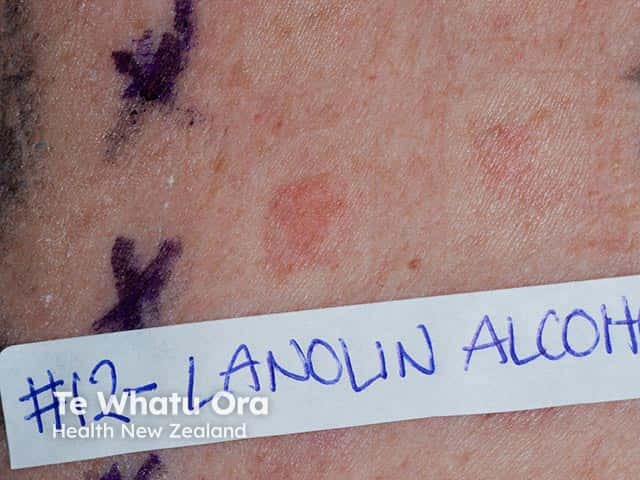
Positive patch test to lanolin alcohol
Erythema may be more difficult to appreciate in darker skin types, and postinflammatory hyperpigmentation is more common.
In the United States, non-Hispanic black patients are less likely than their non-Hispanic white counterparts to be allergic to lanolin.
Contact allergy to lanolin is diagnosed by patch testing. However, patch testing preparations vary, with no universal consensus. The composition of lanolin can also vary between different sources, breeds of sheep, geographical locations, extraction methods, and chemical modifications, making representative patch testing a challenge.
Commonly used patch testing regimes include one or more of the following:
Repeated open application tests (ROAT) may be useful for patients with questionable or weak reactions to patch testing.
Potential types of contact reactions to lanolin include:
Depending on clinical presentation, other differential diagnoses to consider include:
As with other contact reactions, once lanolin has been identified as an allergen, education and avoidance are the cornerstone of treatment and prevention.
Product labels should be checked for ingredients and products containing lanolin avoided. Lanolin and its derivatives are also known by several other names. These include:
Management of dermatitis caused by lanolin may require emollients and moisturisers or topical steroids.
For more information, see irritant contact dermatitis and allergic contact dermatitis.
Symptoms usually settle once the allergen (or irritant) is identified and avoided. Ongoing exposure (eg, at work) can cause chronic symptoms.