Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, July 2014.
Introduction Causes Demographics Clinical features Diagnosis Treatment
Disseminated secondary eczema is an acute, generalised dermatitis that arises in response to a localised inflammatory skin disease.
It is also called an id reaction, autosensitisation dermatitis, and autoeczematisation.
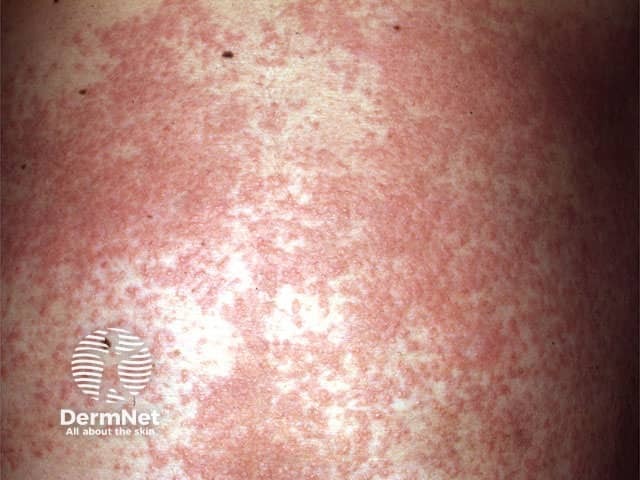
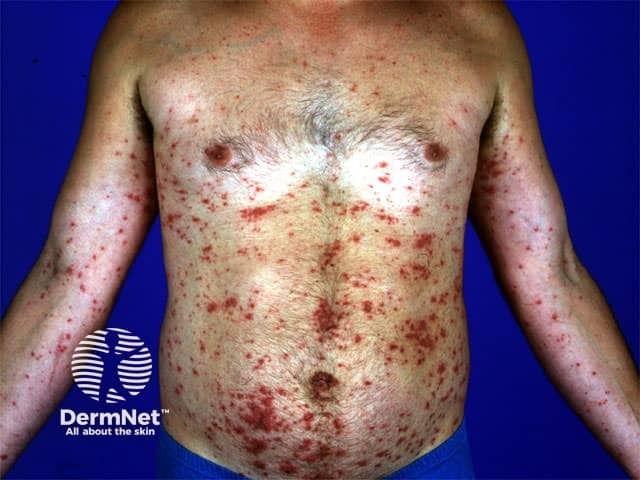
The cause of disseminated secondary eczema is unknown. Theories suggest it is an immune response to a component of the skin and/or to circulating infectious agents or cytokines.
Disseminated secondary eczema can occur in children and adults, but is typically diagnosed in older people with a neglected primary rash on the lower leg.
The common types of eczema/dermatitis that precede disseminated secondary eczema—an eczematid—are:
Infections associated with disseminated secondary eczema include:
Disseminated secondary eczema presents as an acute, symmetrical, generalised acute eczema. It tends to be extremely itchy, disturbing sleep.
Non-eczematous id reactions include erythema nodosum, acute febrile neutrophilic dermatosis, guttate psoriasis, and blistering skin conditions.
The clinical features of disseminated secondary eczema are characteristic. Finding the cause depends on taking a careful history of the initial site of a skin problem. Sometimes the patient does not associate a chronic minor rash with their current widespread and symptomatic eruption.
Additional investigations that may be considered include:
The primary rash needs to be treated vigorously. This may require systemic therapy, such as antibiotics for a bacterid or oral antifungal for a confirmed dermatophytide.
The secondary eczema is often extensive and highly symptomatic. Treatment may entail: